Introduction
Insertion of an indwelling urethral catheter (IDC) is an invasive clinical procedure that should only be performed using aseptic technique. Catheterisation of the urinary tract should only be done when there is a specific and adequate clinical indication,
as it carries a risk of infection.
This guideline does not refer to clean intermittent catheterisation (CIC). Please refer to RCH Nursing Guideline: Teaching and supporting Clean Intermittent
Catheterisation for parents and children for CIC care.
Aim
To ensure the insertion and care of the urinary catheter is carried out in a safe manner that minimises trauma and infection risks.
Definition of terms
- CAUTI- Catheter Associated Urinary Tract Infection
- Indwelling Urinary Catheter (IDC): A catheter which is inserted into the bladder, via the urethra and remains in situ to drain urine.
- Oliguric: Urine output that is less than 1 mL/kg/h in infants, and less than 0.5 mL/kg/h in children.
- Paraphimosis: occurs when the foreskin is left in a retracted position. The pain and swelling may make it difficult to return the foreskin to the non-retracted position, this may reduce blood flow to the tip of the penis which if left untreated
could lead to necrosis of the glans penis.
Indications
- To drain the bladder prior to, during, or after surgery
- For investigations
- To accurately measure the urine output
- To relieve retention of urine
- To relieve urinary incontinence when no other means is practical
Contraindications
- Confirmed or suspected urethral injury
- History of difficult catheter placement
- History of urethral strictures
- Known major abnormalities of the lower urinary tract
Preparation
Preparation of the child and family
- Gain patient/primary care givers consent for procedure
- Families/primary care givers should be given a thorough explanation of the procedure. Involve the parents where possible when providing an age-appropriate explanation of the procedure to the patient.
- Consider the need for a referral to child life therapy to assist in explaining and preparing the patient for the procedure
- Nursing staff should discuss and plan procedural pain management with the child and family prior to the procedure. This may include non-pharmacological (including distraction techniques) and pharmacological considerations including Nitrous Oxide or
sedation if necessary. For more information regarding this please see the RCH Nursing Guideline: Procedural Management.
Preparation of Environment and Equipment
Ensure the patient’s privacy is maintained throughout the procedure and that they are kept warm. Ensure there is adequate light to perform the procedure.
If complications are anticipated, the medical team should be present for insertion of the IDC.
Prepare the following equipment:
- Dressing trolley
- Catheterisation pack and drapes
- Sterile gloves
-
Non- sterile gloves, consider protective eyewear and apron
-
Appropriate size catheter (see catheter size
below)
-
Spare catheter- smaller/bigger size
- Sterile Lubricant and/or xylocaine gel*
- Sterile water to inflate balloon (normal saline can crystallise and render the balloon porous, causing its deflation and the risk of catheter loss)
- 5mL/10mL Syringe – as stated on catheter packaging
- Specimen jar
- Sterile kidney dish
- Cleansing solution (Aqueous 0.1 percent chlorhexidine or 0.9 percent saline)**
- Straps/tape to secure catheter
- Sterile drainage bag
- Waterproof sheet
- Waste bag
- A second person may be required to assist in maintaining the child’s position
* At RCH, sterile lubricating gel is commonly used, however the use of xylocaine gel may be appropriate for boys older than 3 years.
** As per Mitchell et al. (2021), there is emerging, although limited evidence, regarding the use of chlorhexidine 0.1% to reduce catheter associated urinary tract infections associated with catheter insertion.
Catheter size
Catheters are measured in French (Fr) and indicate the external diameter. There is an international colour code for the catheter sizes. Use an appropriate size catheter depending on the age of the child. Catheters that are too big or small are at risk
of urethral trauma or leakage. The rational for IDC insertion should also be considered when selecting catheter, for example a patient requiring an IDC post kidney trauma may require a larger size to provide adequate drainage of potential blood clots.
When selecting a catheter, always choose the smallest size that will provide adequate urinary drainage and minimise bladder neck and urethral trauma.
Consider silicone catheter if for long term use.
|
Age
|
Weight
|
Foley
|
|
Neonate
|
<1200g |
3.5 Fr umbilical catheter
|
|
Neonate
|
1200-1500g
|
5 Fr umbilical catheter
|
|
Neonate
|
1500-2500g
|
5 Fr umbilical catheter or size 6 Fr Nelaton
|
| Neonate | 2.5-3.5kg | 6 Fr Nelaton (non-balloon IDC) |
|
0-6 months
|
3.5-7kg
|
6 Fr or 6 Fr Nelaton |
|
1 year
|
10kg
|
6 – 8, preferably 8
|
|
2 years
|
12kg
|
8
|
|
3 years
|
14kg
|
8-10
|
|
5 years
|
18kg
|
10
|
|
6 years
|
21kg
|
10
|
|
8 years
|
27kg
|
10-12
|
|
12 years
|
varies
|
12-14
|
For PICU: Any patient under 6 months of age, on Extracorporeal Life Support (ECLS) require a Nelaton Catheter. Foley catheters are contraindicated in this patient population.
Balloon Size
Only use sterile water to inflate balloon.
The balloon size is written in mL or cc on the inflation valve/catheter connector and on the packaging.
Procedure for insertion of urinary catheter
The need for an IDC should be discussed with the patients’ medical team prior to insertion. Medical approval for IDC insertion should be ordered and/or documented.
Ensure patient privacy.
The following clinical procedures should be completed in line with principles in the RCH Policies and Procedures: Aseptic Technique.
Female child
- Perform hand hygiene
- Place child in supine position with knees bent
- If soiling evident, clean genital area with soap and water first
- Clean trolley/work surface with detergent
- Identify and collect all equipment for procedure
- Perform hand hygiene
- Open dressing pack (aseptic field) and prepare equipment without contaminating the aseptic field or sterile items
- Pour cleaning solution onto tray
- Perform aseptic hand wash and don sterile gloves
- Apply sterile drapes/towel
- Separate labia with one hand and expose urethral opening. In neonates, the urethral meatus is immediately above the hymeneal fringes (use non-dominant hand for the dirty procedures, and dominant hand for the clean procedures).
- Using chlorhexidine-soaked swabs held in forceps in the other hand clean the labial folds and the urethral opening. Move swab from above the urethral opening down towards the rectum. Discard swab after each urethral stroke into waste bag or designated
waste area. Repeat 2-3 times.
- Remove catheter wire if a 6Fr catheter is used
- Lubricate catheter
- Insert catheter into the urethral opening, upward at approximately 30-degree angle until urine begins to flow.
- Inflate the balloon slowly using sterile water to the volume recommended on the catheter. Check that child feels no pain. If there is pain, it could indicate the catheter is not in the bladder. Deflate the balloon and insert the catheter further into
the bladder.
ALWAYS ensure urine is flowing before inflating the balloon.
Note that in a child under 6 months a balloon is
not typically used. In this case be especially mindful that strapping is
secure.
- Withdraw the catheter slightly until resistance is felt and attach to drainage system
- Remove gloves and perform hand hygiene
- Secure the catheter to the thigh with either a catheter securement device or tape
- Clean trolley and dispose of used articles into waste bag
- Perform hand hygiene
If unable to pass the catheter after 2 attempts,
discontinue procedure and seek senior medical team assistance
Note: Labial fusion affect up to two per cent of girls aged three months to six years. It is most common in those aged one to two years. If present, inform medical staff before attempting to insert IDC.
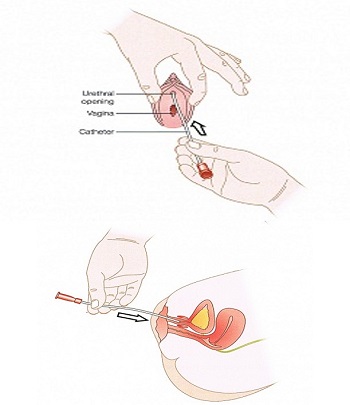
Images courtesy of RCH NDD Stomal Therapy
Male child
- Perform hand hygiene
- Place child in supine position
- If soiling evident, clean genital area with soap and water first
- Clean trolley/work surface with detergent
- Identify and collect all equipment for procedure
- Perform hand hygiene
- Open catheter pack (aseptic field) and prepare equipment needed without contaminating the aseptic field or sterile items
- Pour cleaning solution onto tray
- Perform hand hygiene and don sterile gloves
- Lift the penis and gently retract the foreskin if non-circumcised until the urethral meatus is just visible. Do not force the foreskin back, especially in infants. A sterile gauze swab can be used to hold the penis (use non-dominant hand for the dirty
procedures, and dominant hand for the clean procedures).
- Using other hand, clean the urethral opening with chlorhexidine-soaked swabs held in forceps. Use a circular motion from the urethral opening to the base of the penis. Discard swab into waste bag or designated waste area.
- Lubricate catheter. For post urology surgery consider using xylocaine gel and/or extra lubricating gel to increase lubrication of the urethra and decrease risk of trauma.
- Remove the wire if using a 6Fr catheter
- Hold the sides of the penis with slight upward tension and perpendicular to the child's body (see image below). Insert the catheter.
- When the first sphincter is reached (at level of pelvic floor muscles) gently bring the penis down to face the child's toes, apply constant gentle pressure. On reaching bladder neck, resistance may be felt. If resistance is felt the following strategies
should be considered:
- Increase traction on penis and apply gentle pressure on the catheter
- Ask the child to take a deep breath
- Ask the child to cough and bear down e.g. try to pass urine
- Gently rotate the catheter.
- Remove the catheter and utilise a second tube of lubricant
If unable to pass the catheter seek assistance from treating medical
team or urology registrar. DO NOT use force as you may damage the urethra.
- Advance the catheter and gently insert it completely into the urethra until the connection portion.
- ALWAYS ensure urine is flowing before inflating the balloon.
- Inflate the balloon slowly using sterile water to the volume recommended on the catheter. Check that child feels no pain. If there is pain, it could indicate the catheter is not in the bladder. Deflate the balloon and insert the catheter further into
the bladder. Note
that in a child under 6 months a balloon is not typically used. In this
case be especially mindful that strapping is secure.
- Withdraw the catheter slightly till resistance is felt and attach to drainage system
- Reposition the foreskin if applicable
- Remove gloves and perform hand hygiene
- Secure the catheter to the upper thigh or abdomen in older children with either catheter securement device or tape
- Clean trolley and dispose of used articles into waste bag
- Perform hand hygiene
If unable to pass the catheter, discontinue
procedure and seek senior medical team assistance
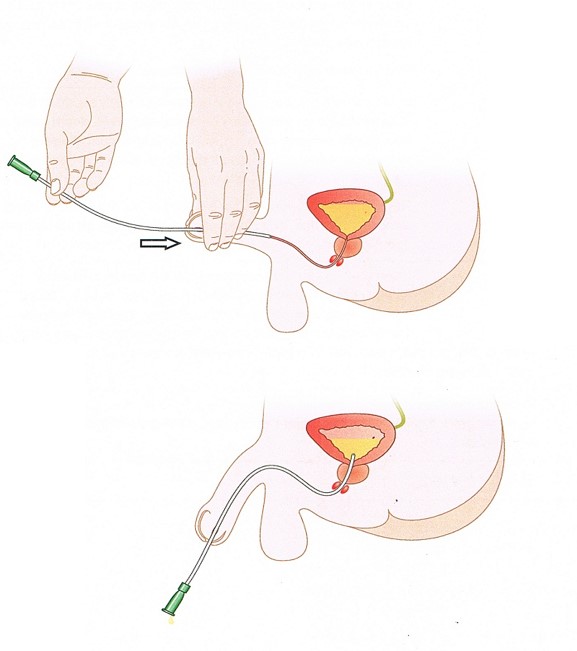
Images courtesy of RCH NDD Stomal Therapy
Securing catheter
Securing the catheter and drainage bag tubing prevents excessive traction and tissue trauma against the bladder neck, preventing urinary tract infections, and catheter dislodgement.
- Tubing should be secured to the upper thigh for females
- To avoid meatal erosion in male patients caused by prolonged catheter pressure, secure the urinary catheter to upper thigh, or, for older male patients, securing to the abdomen and positioning in a soft curve towards the femur may be more appropriate.
Special precautions
Rapid drainage of large volumes of urine from the bladder may result in hypotension and/or haemorrhage. If concerned clamp catheter if the volume seems excessive. Release clamp after 20 minutes to allow more urine to drain. A medical review of the child
should be requested.
For post obstructive diuresis IV replacement of fluid and electrolytes may be required. This should be discussed with the treating medical team.
Documentation
Insertion of the IDC should be documented in the LDA activity.
- Including catheter type, length and size
- Amount of water instilled into balloon
- Document all procedures and cares involving IDC cares
Ongoing nursing management
- Measure urine output as indicated 1 – 4 hourly, assessing the colour and concentration of urine output.
- Unless otherwise specified by the treating team, normal paediatric urine output is 1-2mL/kg/hr. Report any variation from this to the treating medical team.
- Certain drugs will increase diuresis, such as diuretics and ACE inhibitors.
- If oliguric ensure catheter is not blocked (see troubleshooting below).
- Record fluid balance.
- The IDC insertion site and securement should be assessed at least once a shift- observe for leaking at catheter site, tension or twisting of catheter, redness and discharge. Report and document any abnormalities to the medical team immediately.
- IDC drainage bags should be emptied once a shift at a minimum.
- Position drainage bag to prevent backflow of urine or contact with the floor. Gravity is important for drainage and prevention of urine backflow. Ensure the drainage bag is below the level of the bladder, is not kinked or twisted and is secured.
- Assess daily for ongoing need of IDC
Drainage system
Adherence to an aseptic continuously closed method of urinary drainage has been shown to markedly reduce the risk of acquiring a catheter associated infection. Breaches to the closed system should be avoided.
Consider changing the catheter tube and/or bag based on clinical indicators including infection, contamination, obstruction or if system disconnects. If the equipment is damaged or leaks, replace system and/or catheter using aseptic technique and sterile
equipment.
Hygiene
- Routine hygiene should be maintained with routine bathing/showering, including daily clean IDC insertion site with warm soapy water and more frequently if build-up of secretions is evident
- Uncircumcised boys should have the foreskin gently eased down over the catheter after cleaning.
- Always check the strapping of the catheter is secure after hygiene is performed.
Infection
- Consider daily the need for the IDC to remain in situ. Remove as soon as no longer required to reduce risk of Urinary Tract Infection (UTI).
- Cloudy, offensive smelling or unexplained blood-stained urine is not normal and needs further investigation. Other signs of infection include fever and abdominal pain.
Specimen collection
- Urine for urinalysis or culture should be collected fresh from the needleless sampling port of catheter tubing (not drainage bag), this should be completed in line with the
Aseptic
Technique Procedure.
- Large volumes e.g. 24hr collection, can be collected from drainage bag.
Troubleshooting
Catheter
not draining/ blocked/patient oliguric (under 0.5m/kg/hr)
- Check catheter/tubing not kinked
- Check catheter is still secured to patient and that it hasn't migrated out of bladder
- Assess patient’s hydration status to ensure they are not dehydrated. Consider the need to perform a bladder scan to assess bladder volume. Escalate to medical team if concerned.
- The patency of a catheter can be checked via the sampling port or catheter tubing. A blocked catheter should be flushed via the catheter tubing, this is of particular importance in case of blood clots or mucus (for example after a bladder augment).
The following techniques to check for patency and/or flush a catheter
should be completed using standard aseptic technique.
|
Checking
catheter patency via Needleless Sampling Port
|
Checking
catheter patency and flushing via Catheter Tubing
|
- Clamp catheter below the sampling point.
- Scrub sampling point vigorously with 70% alcohol and 2% chlorhexidine-soaked gauze or swabs for at least 15 seconds and allow to air dry prior to accessing port
- Attach luer lock syringe and gently flush 10mLs of normal saline into the catheter.
- Pull back on the syringe to withdraw saline/urine.
- If saline is not coming back on suction, gently reinject 10mLs of normal saline and let urine drain by itself without sucking back on the syringe. It may be that the catheter tip is stuck to the bladder wall. So, ensure the saline
is flushing easily and urine is subsequently flowing back by itself, without any suction.
- At no time should force be used to instil fluid when checking for patency or flushing a catheter.
|
- Clamp catheter and disconnect the catheter bag.
- Attach a catheter tipped syringe (Toomey Syringe) to the catheter tubing (where the catheter bag has been disconnected) and gently flush 10mLs of normal saline into the catheter.
- Pull back on the syringe to withdraw saline/urine.
- If saline is not coming back on suction, gently reinject 10mLs of normal saline and let urine drain by itself without sucking back on the syringe. It may be that the catheter tip is stuck to the bladder wall. So, ensure the saline
is flushing easily and urine is subsequently flowing back by itself, without any suction.
- At no time should force be used to instil fluid when checking for patency or flushing a catheter.
- Consider attaching a new/clean drainage bag to the catheter.
|
Catheter leaking
- Ensure the catheter is still draining and that the urine is not overflowing around a blocked catheter. See above for tips regarding catheters not draining.
- If the catheter is a balloon catheter, make sure the balloon is still inflated. Hold the catheter tubing securely in the same position and empty the balloon to make sure the amount that has been placed initially in the balloon is still present. If
not, reinflate the balloon to its initial volume with water. Deflation of the balloon happens easily with a 6Fr catheter.
- Check catheter size is correct for age/size of the child. Use of a balloon catheter in neonates
should only be with consultation with the treating medical team.
- Consider the need to remove and reinsert a new catheter in consultation with the treating medical team.
Removal of urinary catheter
Discuss with
treating team prior to removal
Equipment required for removal
- Non-sterile gloves, consider protective eyewear and apron
- 5mL/10mL syringe – as stated on catheter packaging
- Waterproof sheet
- Kidney dish / receiving container
Procedure
- Explain procedure to child and family and gain consent.
- Check amount of water used to inflate IDC balloon.
- Gather equipment required for removal
- Ensure patient privacy and have patient in supine position.
- Place waterproof sheet and/or kidney dish between patient legs.
- Perform hand hygiene & don gloves.
- Deflate balloon completely and remove any straps/tapes
- ALWAYS
check the balloon is not inflated prior to removal of IDC. Gently withdraw catheter on exhalation if possible, with rotation movements if necessary.
Once inflated, the balloon won’t deflate to its total initial flat state and the balloon portion of the catheter will remain larger than the catheter itself.
- If resistance felt and catheter cannot be easily removed do not force, leave catheter in situ and consult medical team.
Consider cutting the catheter at the balloon inflation point to ensure the balloon is deflated.
Once removed inspect
catheter for intactness. Report to medical team if not intact.
- Perform hand hygiene.
- Document catheter removal in the LDA activity.
- Observe for urine output post catheter removal. Unless otherwise specified by the treating team, normal paediatric urine output is 1-2mLs/kg/hr.
- If the patient has not passed adequate urine 6 – 8hours post catheter removal, assess the patient’s hydration status and consider the need to perform a bladder scan. Discuss findings with the treating medical team.
Complications
- Inability to catheterise
- Ensure appropriate catheter size has been selected based on the age/size of the child
- Escalate to the treating medical team and consider the need for a referral to the urology team.
- In young girls, the urethra can be difficult to localise and the catheter can go directly in the vagina. In this case, leave the first catheter in the vagina and use another one to place immediately above, which will be more likely
to go in the urethra.
- Urethral injury may occur from trauma sustained during insertion or balloon inflation in incorrect position: it is very important to ensure the catheter is in the bladder before inflating the balloon, this can be confirmed by visualising the stream
of urine prior to balloon inflation.
- False passage (catheter pushed through urethral wall): The risk of false passage is higher when using a smaller catheter, ensure catheter size utilised is appropriate for child’s age and size.
- Paraphimosis due to failure to return foreskin to normal position following catheter insertion:
- To minimise risk, always replace the foreskin to normal position in non-circumcised patients and check at catheter care or nappy change that the foreskin is in place.
- Urethral strictures following damage to urethra
- Infection
- To minimise risk of infection insertion of IDC’s must be performed using surgical aseptic technique with sterile gloves.
- Regular hygiene should be maintained whilst IDC is in situ.
- Where possible avoid disconnecting the IDC circuit to minimise risk of contamination
- Monitor for and report signs of infection including fever, offensive smelling urine, unexplained blood or cloudy urine.
- Consider daily the need for the IDC to remain in situ. Remove as soon as no longer required to reduce risk of Urinary Tract Infection (UTI).
- Psychological trauma
- Haemorrhage
Discharge information
Some children will be discharged from the hospital with their IDC insitu. It is important to teach the families how to care for the catheter, how to perform hygiene, how to monitor the output and how to troubleshoot. Refer to Kids Health
Info Fact Sheet: Indwelling urinary catheter
Companion documents
Other RCH IDC resources available:
Evidence Table
| Reference |
Source of evidence
|
Key
findings and considerations |
| Anderson, C., & Herring, R. (2019). Pediatric Nursing Interventions and Skills. In M. Hockenberry, D. Wilson, & C. Rodgers (Eds.) Wong’s Nursing Care of Infants and Children (pp. 701-704). St. Louis, Missouri: Elsevier. |
Textbook |
Bladder catheterization procedure. Male and female specific IDC insertion techniques. · Sizing of catheter for paediatric age groups · Use of lignocaine gel
|
| Galiszewski, J. M. (2017). An intervention to improve the catheter associated urinary tract infection rate in a medical intensive care unit: direct observation of catheter insertion procedure. Intensive and Critical Care Nursing. 40
(2),26– 34. https://doi.org/10.1016/j.iccn.2017.04.002 |
Case control study |
Insertion technique of IDC for male and females. Cleansing of area for insertion of IDC
- Equipment needed for IDC insertion.
- Preparing patient for the procedure
- Retract gently once balloon is filled, until you feel resistance to check position and security
|
Gould, C., et al. (2019) Guideline for prevention of catheter associated urinary tract infections. Centers for Disease Control and Prevention.
https://www.cdc.gov/infection-control/media/pdfs/Guideline-CAUTI-H.pdf
|
Guidelines |
- Indications for IDC insertion
- Inappropriate uses for IDC insertion
- Only insert IDC if necessary and minimise duration as appropriate, particularly those at risk of CAUTI
- Insertion steps of IDC
- Must be an appropriately trained health care professional inserting IDC
- IDC maintenance: maintaining a closed drainage system, when to replace IDC and collecting system, keeping an unobstructed drainage system.
- PPE use: standard precautionsRoutine hygiene – water and soapy water for cleaning meatus when IDC insitu
|
| Government of Western Australia Department of Health. (2019). Urethral Catheterisation Neonatal Guideline. https://www.cahs.health.wa.gov.au/-/media/HSPs/CAHS/Documents/Health-Professionals/Neonatology-guidelines/Urethal-Catheterisation.pdf |
Guideline |
Procedural guideline for IDC insertion of a neonate – male and femal
- Preparation of environment and equipment
- Specimen collection procedure
- Position drainage bag to prevent backflow of urine or contact with the floor.
- Gravity is important.
|
| Hucker, J., Lawson-Wood, H. (2023) Indwelling urinary catheter insertion 1: children and young people. Nursing Times. 119(3). |
Double-blind peer reviewed |
- Clinical indications
- Considerations
- Preparation of patient
- Attach to thigh or groin
- Do not attach catheter to leg
|
| Macqueen, S., Bruce, E., Gibson, F. (Eds.). (2012). The Great Ormond Street Hospital Manual of Children’s Nursing Practices. Wiley-Blackwell, 734-744 |
Manual |
- Insertion technique
- Preparation of patient and equipment
- Strapping to abdomen or thigh not leg
|
| National Health and Medical Research Council (2020). Australian Guidelines for the Prevention and Control of Infection in Healthcare. Canberra: National Health and Medical Research Council. https://www.nhmrc.gov.au/sites/default/files/documents/infection-control-guidelines-feb2020.pdf
P164 p173 |
Guideline |
The risk of infection is related to the method and duration of catheterisation, and the quality of catheter care. The longer the urinary catheter is in place the greater the risk of infection.
- Minimise duration of catheterisatio
- HCW should be trained and competent in insertion and maintenance of urinary devices
Table 24,
- Clean urethral meatus with sterile normal saline before insertion of catheter.
- Use sterile single-use lubricant when inserting catheter.
- Use aseptic closed system and standard aseptic technique to empty urinary drainage bags.
- Daily meatal and periurethral hygiene through routine bathing or showering.
|
| Mitchell, B., et al. (2021). Effectiveness of meatal cleaning in the prevention of catheter-associated urinary tract infections and bacteriuria: an updated systematic review and meta-analysis. BMJ Open 11(6). |
Systematic review |
Some potential benefit of using antiseptics, compared with non-antiseptics for meatal cleaning to prevent bacteriuria and or CAUTI was identified Antiseptics (chlorhexidine or povidine-iodine) may be of value for meatal cleaning
on the incidence of CAUTI, compared with comparator agents (saline, soap or antimicrobial cloths)
|
| Newman, D. (2007). The Indwelling Urinary Catheter Principles for Best Practice. Journal of Wound, Ostomy and Continence Nursing, 34(6), 655-661. |
Overview of practice |
The best method of stabilization has not been well-defined. Several best-practice models in the nursing literature recommend that the catheter be secured or anchored to the upper thigh in women and upper thigh or abdomen in men.The
male lower urinary tract benefits from having the urethra in a straight position.
|
| Royal Children’s Hospital. Teaching and Supporting Clean Intermittent Catheterisation for Parents and Children. https://www.rch.org.au/rchcpg/hospital_clinical_guideline_index/Teaching_and_supporting_Clean_Intermittent_Catheterisation_for_parents_and_children/ |
Guideline |
Images for male and female catheterisation
|
|
Royal College of Nursing. (2021). Catheter Care- RCN Guidance for Healthcare Professionals. |
National standards |
Indications for IDC insertion
- Aseptic technique/environment when performing IDC insertion/care
- Paraphimosis definition
|
Starship Hospital. Urinary Catheter Management. https://starship.org.nz/guidelines/urinary-catheter-management/
|
Guideline |
- Contraindications
- Catheter securement
- Preparation of the child and family
- Labial fusion
- Foley size
|
Please remember to
read the disclaimer.
The revision of this nursing guideline was coordinated by Amy Carle, CNS, Day Surgical Unit and Nursing Research, and approved by the Nursing Clinical Effectiveness Committee. Updated October 2024.
