Introduction
Eczema is a chronic inflammatory skin condition that affects 30% of children in Australia and causes dry, hot, itchy, red skin
Aim
To provide evidence-based strategies for the management of Eczema (atopic dermatitis) in order to improve eczema severity and reduce the negative impact on patient and family quality of life.
Definition of Terms
- Eczema (atopic dermatitis): common, chronic inflammatory skin condition, presenting as generalised skin dryness and itch. Characterised by chronic dermatitis with remission and relapse with acute flares. Caused by interplay between environmental and genetic factors.
- Flares: a worsening of the eczema
- Triggers: factors that cause the eczema to flare
- Wet dressings: dressings used in the treatment of eczema
- Infected eczema: weeping and crusting occurs when the eczema is secondarily infected by organisms such as bacteria Staphylococcus aureus, Streptococci, Candida or viruses such as Herpes simplex and molluscum contagiosum
Assessment
The UK Diagnostic Criteria for atopic eczema are:
- Must have itch
- Plus 3 or more of the following:
- History of involvement in skin creases
- Personal history of asthma or allergic rhinitis (or history of atopic disease in 1st degree relative if child is under 4 years of age)
- A history of dry skin in the last year
- Onset under the age of 2 years (not used if child is under 4 years)
- Visible flexural eczema
Erythema: redness of the skin
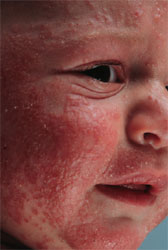 |
Discoid eczema: disc shaped, clearly demarcated eczematous patches to limbs and trunk.
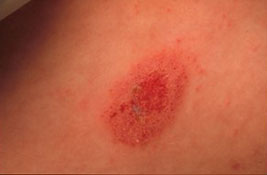 |
Bacterial secondary infection: Crusting, weeping, erythema, cracks, frank pus, or multiple excoriations. Increased soreness and itch.
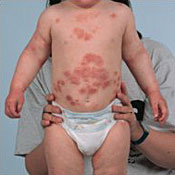 |
Assessment tools
Patient assessment should be undertaken by either a medical officer or a nurse practitioner/ consultant to grade the degree of eczema severity (mild, moderate or severe), and the presence or absence of infection.
The type and frequency of eczema treatments depend on eczema severity and the presence/absence of infection.
Eczema severity
| Clear |
Normal skin, no evidence of active atopic eczema |
| Mild | Areas of dry skin, infrequent itching (with or without small areas of redness) |
Moderate
| Areas of dry skin, frequent itching, redness (with or without excoriation and localised skin thickening) |
| Severe | Widespread areas of dry skin, incessant itching, redness (with or without excoriation, extensive skin thickening, bleeding, oozing, cracking and alteration of pigmentation) |
Management
Eczema Treatments fall into two categories - Everyday /Trigger Avoidance and Flaring /Acute
1. Everyday treatments and avoidance of triggers
These treatments are ongoing regardless of the presence or absence of eczema.
- Avoiding environmental aggravators
- Heat - such as thick layers of clothes, hot heaters, hot cars, classrooms, hot baths, thick blankets, woolen underlays or electric blankets and hot water bottles.
- Prickly/rough material - for example wool, sandpits, clothing tags.
- Potential Irritants - Avoid washing machine powders, shampoos, moisturising products that contain Sodium Lauryl Sulfate (SLS), Benzalkonium Chloride, Plants, Fragrance/Perfumes and Food products.
- Regular moisturiser, should be applied from top to toe at least twice a day even if the skin is clear of eczema to reduce the skin dryness. Apply to wet skin after bathing and reapply when skin feels dry.
- When topical steroids are in use moisturisers should be applied directly over the steroids.
- Examples of over the counter in pharmacy moisturisers: QV cream™, Cetaphil cream™, Kenkay cream™, Atoderm crème™, Avene xeracalm™ cream, Dermezetm treatment cream, CeraVetm Cream Lipikar™ AP+M.
- Creams should be removed from the tubs onto clean paper and then taken from the paper to the skin to avoid bacterial contamination of the tub.
- Avoid creams containing SLS, Benzalkonium Chloride, Plant, Fragrance/Perfumes and Food products.
- Daily cool bath (30-32 degrees C) - The face and head should be wet well and the skin should not be rinsed with fresh water after the bath. It is no concern if the child swallows some of the water.
- BATH OIL-non soap (1-2 capfuls).
- SALT - when the eczema is moderate to severe or the skin stings when the child bathes, salt (1/3 cup per 10 litres water) may be added.
- BLEACH - when the eczema moderate to severe or infected (or as recommended by healthcare professional) add white king household bleach 4% (sodium hypochlorite 4%) (12mLs per 10 litres water).
- All three ingredients can be added together to the bath water. If skin infection present it is preferred to not add bath oil.
- Consider Vitamin D oral daily supplementation for moderate to severe eczema or if the baby is breast fed. This is especially important throughout Colder/Winter months.
2. Flaring treatments
These treatments should be commenced as soon as there is a flare (when the skin is rough - like sandpaper, an increase in redness or itch levels), and stopped when the symptoms are controlled and re-started if flaring again. As the eczema is better controlled the need for topical steroids will decrease.
2.1 Topical steroids and anti-inflammatory creams
Topical steroids are required once or twice daily until the skin is completely clear to reduce skin inflammation. They can be applied to broken and infected skin.
- There is no requirement to use topical steroids ‘sparingly’ or for regular breaks from steroids during treatment for eczema flares. Steroids should be applied liberally/generously followed by moisturiser. Steroid cream dosage for application should be calculated the " Fingertip Unit" method.
- For mild facial eczema use a weaker potency (than for body) steroid such as hydrocortisone 1% twice a day as required. These are available in cream and ointment eg Cortic™, Sigmacort™. No prescription is required.
- For moderate facial eczema which is non-responsive to steroids (such as hydrocortisone 1%) a pimecrolimus (Elideltm™ cream) can be prescribed by medical/nurse practitioner as a non-steroid alternative to use as a second line treatment. Can be used twice a day in sensitive areas such as face, eyelid and groin.
- For body and scalp use a stronger steroid (than the face) example Advantan™ or Elocon™. These are available in cream, ointment, fatty ointment and lotion.
- As the eczema is better controlled the need for topical steroids will decrease.
2.2 Moisturisers
2.3 Bathing
2.4 Medications
Antihistamines are not routinely used for eczema unless it has been triggered by an allergic, environmental allergens or insect bites. They can assist with the eczema itch. Use with caution as directed by medical practitioner, in children under 12 months of age.
2.5 Tar creams
Used when the skin is lichenified (thickening of the skin) or for discoid eczema. Tar creams should not be applied to the face, groin and flexures. These creams can be applied directly over the steroid creams and under the moisturiser. A suggested compound for a tar cream is 3% LPC in zinc cream (example KenKay™ dual purpose cream). No prescription necessary but require a compounding pharmacy
2.6 Wet dressings
Used for moderate to severe eczema or when the children are waking from the itch.
If the wet dressings (example Tubifast™) are not readily available wet clothes (onesie, leggings/T Shirt) can be used instead. A dry layer of clothing may be applied over this however remove the top layer when dry and if awake. Wet dressings should only be needed for 3-5 nights.
Wet dressings using Tubifast tm
The wet dressing/clothes regime is as follows:
- Mild eczema
- Moderate eczema
- Once to twice daily for 3 days
- Nightly until the eczema is clear and then recommence nightly if flaring
- Severe eczema
- Four times a day for 3 days only (Admission or HITH may be referred to assist during this acute phase)
- Then taper to twice daily for one week
- Then nightly until the eczema is clear and then recommence nightly if flaring.
Cool compress
- Can be used for immediate relief of itch especially to face
- Wet a cloth (example chux towel or rediwipe) with water and plain bath oil
- Apply cool, wet cloth to itchy areas for 5 -10 minutes, then apply a moisturiser post compressing
- Age dependent, children should be encouraged to learn this technique rather than scratching
- Using a thermal water spray to the itchy area is another option
| Wet dressings
 Cool compresses
 |
Management of Complications - Infected eczema
Secondary bacterial infection
Is a common complication of eczema as the skin is not intact and thus more vulnerable to infection. Infection can make eczema worse and more difficult to treat. Bacterial infection should be suspected if there is crusting, weeping, frank pus, cracks, multiple excoriations increased soreness and itching. A common causative bacterium is Staphylococcus aureus which is commonly found on eczema skin.
Secondary viral infection
Is caused by herpes simplex virus (HSV) is characterized by a sudden onset of grouped, small white or clear fluid filled vesicles, satellite or "punch out" lesions, pustules, and erosions. It is often tender, painful and itchy.
NOTE: most patients with viral infected eczema, invariably also have a bacterial skin infection as well. Assess using appropriate skin swabs to identify causative organism.
Other viruses that may cause the eczema to flare are molluscum contagiosum and coxsackie A6 virus (hand foot and mouth disease).
Secondary bacterial infection 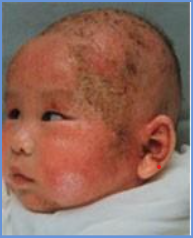
|
Secondary herpes simplex 1 infection
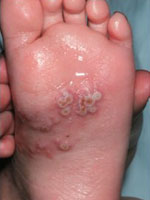 |
The principles of managing infected eczema are:
- Remove the crusts with a wet disposable cloth (example chux or rediwipe) and gently wipe. This is best done when bathing.
- Steroid cream can be applied over open skin and presence of infection, however FIRST remove the crusts and weeping.
Daily plain water bath adding
- White king™ household bleach 4% (sodium hypochlorite 4%) to the cool bath water (30 – 32 degrees). The dilution should be 12 mLs per 10 Litres of water.
- Salt can be added to decrease stinging and to help settle inflammation and itch. The dilution is 100 grams or 1/3 cup per 10 Litres of water.
- Bleach baths
For bacterial infections
- A bacterial swab may be ordered by medical / nurse practitioner to confirm infection and bacterial sensitivities or if suspecting a multi resistant organism e.g MRSA
- Oral antibiotics prescription may be required (example cephalexin or flucloxacillin) for 5 to 10 days.
For viral infections likely caused by HSV
- Prescription required for oral acyclovir as soon as possible and within 48 hours of onset of symptoms. Little benefit will be realised if treatment is delayed beyond onset of symptoms after 72 hours (unless patient is immunocompromised or has progressive clinical state)
IV acyclovir may be used for severe infections, those who are systemically unwell and febrile patients and those patients with threatened eye involvement.
*Urgent Ophthalmology review if the infection is near the eye(s).
Possible investigations
Inpatient admitted, for eczema, should have bacterial skin swabs taken.
- This swab should be collected from an open, excoriated, or crusted eczema lesion. Allowing determination of causative organism, and to identify organism resistances to assist with antimicrobial prescribing.
For patients attending the Outpatient Department,
- A skin swab should be taken from an infected eczema lesion when MRSA is suspected or to verify a bacterial organism.
- Patient and parent nasal swabs are only required for patients who are experiencing recurrent infections and boils when suspecting ongoing nasal carriage.
Viral swabs may be needed to confirm causative organism, this should be collected from the base of a fresh blister.
Documentation - Eczema Treatment Plan
All patients should have an Eczema Treatment Plan completed before they are discharged/go home.
See EMR smart phrase “Eczema treatment plan”
Product List RCH Dermatology
Referrals
Patients may require to be seen by other specialties. A medical referral is required for Paediatrician, Allergist, RCH Dermatology/Eczema Clinic and HITH.
| Eczema NEW clinic appointments |
Eczema Clinic Coordinator |
9345-6441 (Mon-Fri) |
| Allergy testing and advice |
Immunology or RCH Allergy Department or private allergist |
9345-6180
|
Family require ongoing support for eczema treatment / management at home. See link for referral criteria. RCH HITH traffic light eczema Aug22 |
Wallaby Ward Hospital in the Home (HITH) |
9345-4770
Email: Wallaby.Ward@rch.org.au |
Medical complications ie. FTT, low iron/vitamin D
|
General Medicine |
9345-6180 (Mon-Fri) |
Follow up appointment recommendations
| Mild eczema |
General Practitioner |
|
| Moderate eczema |
General practitioner or Specialist Clinics – Eczema Clinic - NEW
|
2 - 4 weeks, if improved to mild then discharge to General Practitioner |
| Severe eczema |
Specialist Clinics – Eczema Clinic - NEW
|
1 - 2 weeks, then as per mild and moderate |
For further assistance the Dermatology Registrars can be paged via switchboard 9345 5522.
Allergy
In the event of an immediate reaction (such as urticaria and angioedema) to a food and/or severe persistent eczema in a baby, medical / nurse practitioner to refer for specialist allergy evaluation.
Refer to immunologist, allergist for Skin Prick Test (SPT) and dietician if food allergies are proven on SPT or ImmunoCAP IgE test.
Visit ASCIA for more information: https://www.allergy.org.au/images/pcc/ff/ASCIA_FAST_FACTS_Eczema_and_Food_Allergy_2020.pdf
Parent education information
Prior to discharge discuss the everyday treatments – avoidance of environmental triggers - overheating, rough prickly materials, and ensure regular and ongoing use of moisturisers and eczema baths.
Give guidance on eczema treatment plan
Encourage the families to undertake the Eczema Triggers Questionnaire to help identify most likely to least likely triggers and E learn for education and demonstration of how to apply the topical treatments.
Eczema resources
For clinical staff:
For parents:
Evidence table
Eczema Management Evidence Table
Please remember to
read the disclaimer.
The development of this nursing guideline was coordinated by Emma King, Nurse Practitioner and members of Dermatology Department and Allergy Department, and approved by the Nursing Clinical Effectiveness Committee. Reviewed and updated by Melissa Dallinger & Danielle Paea, December 2025.