See also
Resuscitation: Hospital Management of Cardiopulmonary Arrest
Acute pain management
Key points
- Usually due to minor trauma (eg nose picking) or friable nasal mucosa
- Epistaxis in children <2 years is rare and should prompt consideration of child abuse or underlying systemic disease
- Try simple measures to stop bleeding first
- Effective resuscitation is vital if circulation is compromised (rare)
- Seek early ENT opinion if bleeding is severe or difficult to stop
Background
Epistaxis in children is usually from Little's area (see diagram), located on the anterior septal wall. The bleeding is usually venous, of brief duration, and often recurrent
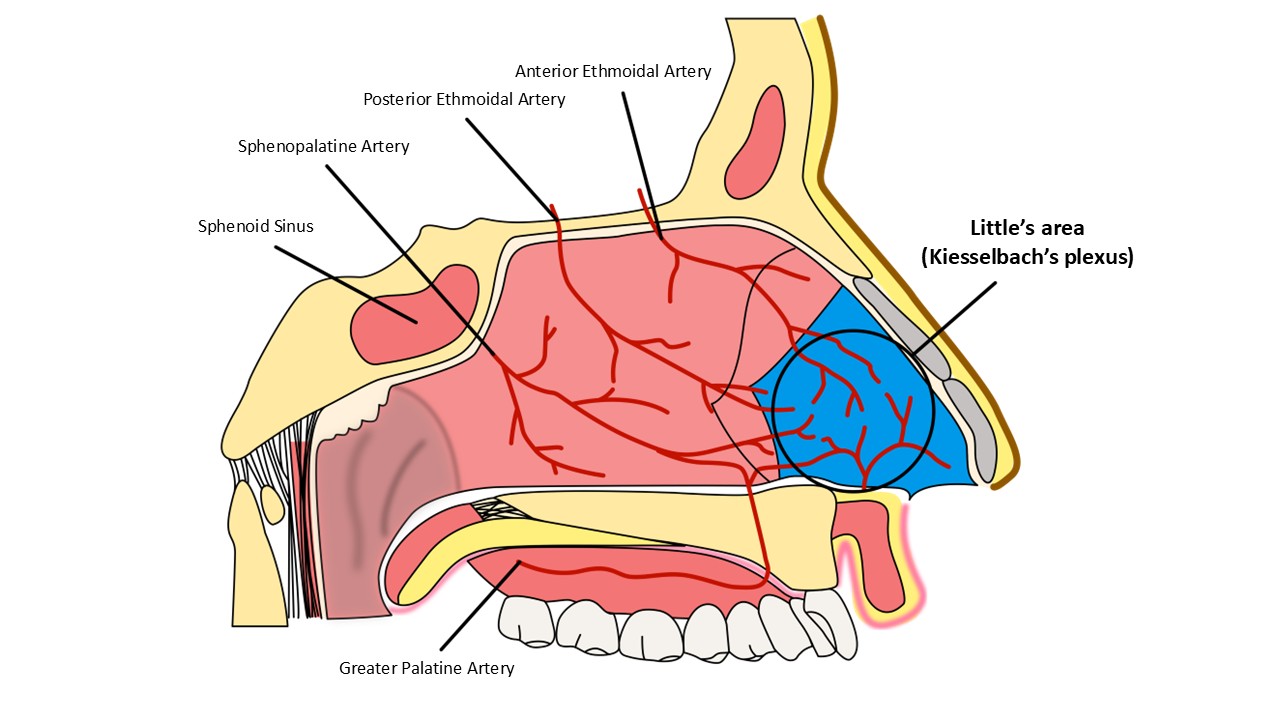
Common causes
- Minor trauma: nose picking, rubbing, sneezing, coughing or straining
- Friable nasal mucosa: upper respiratory tract infection, drying of mucosa (air conditioning/heating), allergic rhinitis
- Medications: topical nasal steroids, NSAIDs, fluvoxamine, chemotherapy
Rarer causes
- Foreign bodies: suspect with unilateral foul discharge. Button batteries require urgent removal
- Nasal polyps
- Bleeding diatheses: von Willebrand disease, ITP, haematological malignancies
- Vascular malformations: hereditary haemorrhagic telangiectasia
- Nasopharyngeal tumors: juvenile angiofibroma in adolescent males
Assessment
History
Consider underlying diagnosis/cause if:
- recurrent, frequent episodes
- easy bruising, gum bleeding, prolonged bleeding after minor cuts
- family history of bleeding disorders
- history of bleeding after surgical challenges eg dental extractions, tonsillectomy, circumcision
- medication history
Red flags
- Age <2 years: high association with trauma, child abuse or underlying illness
- Bleeding >30 minutes despite adequate pressure
- Bilateral bleeding suggests a systemic cause or significant trauma
- History of syncopal episode, haematemesis, melaena or haemodynamic instability
Examination
- Airway/Breathing: assess for compromise (facial trauma)
- Circulation: shock is rare but possible
- Identify site of bleeding: use a headlight/otoscope to look for active bleeding, clots or prominent vessels in Little's area
Management
Investigations
- Often not indicated for single, self-limiting episodes
- Consider FBE, coagulation screen and group and hold/crossmatch in severe/recurrent bleeding, a history suggestive of bleeding disorder or signs of haemodynamic compromise
Treatment
If signs of shock
- Fluid resuscitation
- Tranexamic acid (TXA)
- Consider activation of massive transfusion protocol (MTP)
Try simple measures first to stop the bleeding
- Position child sitting up in a comfortable position eg on parent's lap
- Tilt head forward to prevent swallowing blood
- Apply firm pressure to the anterior portion (cartilage) of the nose against the septum with thumb and forefinger
- Aim to hold continuous pressure for 10 minutes. If the nosebleed continues, continue pressure for another 10 minutes
- Consider placing a cool towel or covered icepack on the back of their neck
- Instruct child to breathe through the mouth and spit out any blood into a kidney dish

If persistent bleeding
- often due to inadequate treatment / pressure
- cautery or packing may be required
- consider application of topical vasoconstrictor eg 1-2 sprays of oxymetazoline 0.05%
Cautery
Cautery is indicated if simple measures fail, and a visible vessel is identified on the anterior septum. Seek senior assistance if cautery is required. Consider procedural sedation if the child is unlikely to tolerate procedure
Cautery procedure video
- Use a good headlight
- Achieve haemostasis by applying gauze soaked in Co-Phenylcaine or topical lignocaine 1% with adrenaline 1:100,000 (0.3mL/kg, max 3mg) to the site for 10-15 minutes and continue to apply pressure
- Apply a silver nitrate stick to the area surrounding the bleeding point first, then the vessel itself. Keep contact for only a few seconds until a white eschar appears
- Simultaneously cauterising both sides of the nasal septum with silver nitrate may be required and is not thought to increase the risk of septal perforation
- Wipe away excess silver nitrate with saline-soaked gauze/cotton to prevent staining/burns
- Apply antibiotic ointment or Vaseline to keep moist
- If these measures fail, nasal packing may be required
Anterior nasal packing
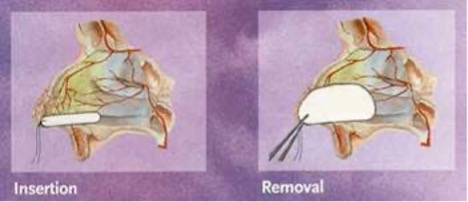
- Seek senior assistance if unfamiliar with procedure
- Any nasal packing is unlikely to be tolerated in the young child, especially given it may be required to remain in situ for 48 hours. Consider whether the procedure is appropriate for their age and development
- If site of bleeding known, insert unilateral anterior nasal pack
- Nasal packing may dislodge clot posteriorly, be prepared with a kidney dish for the child to spit clot out
- Use an appropriately sized prefabricated nasal tampon e.g. Merocel® (non-resorbable)
- Can attempt nasal packing without water soluble lubricating gel first, consider coating if insertion is difficult
- Insert along the floor of the nasal cavity until the string reaches the nose then irrigate with saline to expand. Tape string to the cheek
- Resorbable tampons (eg Surgicel™, Floseal™) are preferred for young children or those with bleeding disorders to avoid the trauma of removal
- Discharge home and review in 48 hours if tolerated
- Moisten with saline prior to removal
If the bleeding site cannot be visualised (profuse/posterior), or bilateral packing is required, consult ENT.
Consider consultation with ENT when
- severe or persistent bleeding
- bilateral anterior packing or posterior packing is required
- age <2 years old or unable to tolerate packing
Consider transfer when
Children requiring care beyond the level of comfort of the local healthcare facility
Consider discharge when
Bleeding has stopped
Parents education provided (see below)
Discharge information
- If simple measures are used to stop bleeding, discharge with education on management at home and on recurrence
- Preventative measures eg no nose blowing for one week, no nose picking, sneeze with an open mouth
- Advise that a smaller nosebleed may occur when the scab falls away
- If there is crusting and the mucosa appears infected, consider treatment with a topical antibiotic ointment (eg mupirocin)
- If dry cracked mucosa contributing, petroleum-based gel (eg Vaseline™) should be applied daily in the morning until healing. Use twice daily for one week if cautery or packing was required
- For frequent recurrences, consider ENT review as an outpatient
Parent information sheet
Nosebleeds
Last updated April 2026