Nasogastric (NG) fluids for short term rehydration or maintenance fluids in children beyond the newborn period
Refer to local guidelines for advice re NG tube insertion and management
Follow specialised fluid guidance for
- Neonates
- Long term nasogastric feeding
- Situations where specialised fluid management is required eg diabetes, cardiac, metabolic and renal conditions
See also
Intravenous fluids
Dehydration
Gastroenteritis
Key points
- Whenever possible, the enteral route (oral or nasogastric) should be used for fluids
- Shocked children require intravenous resuscitation. See Resuscitation: care of the seriously unwell child
- Serial weights are the best measure of acute changes in fluid status. Clinical signs can help estimate the severity of dehydration but are often imprecise
- Rehydration treats dehydration, not the underlying cause. Careful and regular clinical review is required
Background
- Nasogastric (NG) fluids are a safe and effective method of maintaining hydration and correcting dehydration in most children, and are generally well tolerated in pre-school age children
- Advantages over IV fluids include safety, less risk of electrolyte derangement, more rapid recovery from gastroenteritis, and the option to give nutritional fluids eg expressed breast milk (EBM) or formula
Assessment
Indications for NG fluids:
- Rehydration in the setting of gastrointestinal losses, or a period of sustained inadequate intake (see Dehydration to assess degree of dehydration)
- Replacing usual intake where acute illness interferes with usual intake eg bronchiolitis, gingivostomatitis, viral infection
- Replacement of ongoing losses
Contraindications to NG fluids
- Child who is 'nil by mouth' or fasting
- Shock or the critically unwell child
- Possible bowel obstruction: bilious vomiting, severe abdominal distension, ileus
- Altered conscious state, or other risk of aspiration
- Facial trauma, suspected base of skull fracture
Red flags
Children with the following features should be discussed with a senior clinician:
- Age
<6 months
- Severe dehydration, electrolyte abnormalities or hypoglycaemia
- High risk of increased anti-diuretic hormone secretion eg acute CNS and significant pulmonary conditions (although any unwell child is at risk)
- Short gut or other chronic gastrointestinal disorder
- Craniofacial abnormalities
Management
Investigations
- Usually no investigations are needed, unless required for the underlying condition
- Consider blood glucose and electrolyte monitoring in young infants, and those with ongoing significant losses or NG fluid support requirement beyond the initial 4-6 hour rehydration phase. Oral rehydration solutions (ORS) eg GastrolyteTM,
HydralyteTM, PedialyteTM are hypotonic; hyponatraemia can occasionally occur
Treatment
Approach to prescribing NG fluids
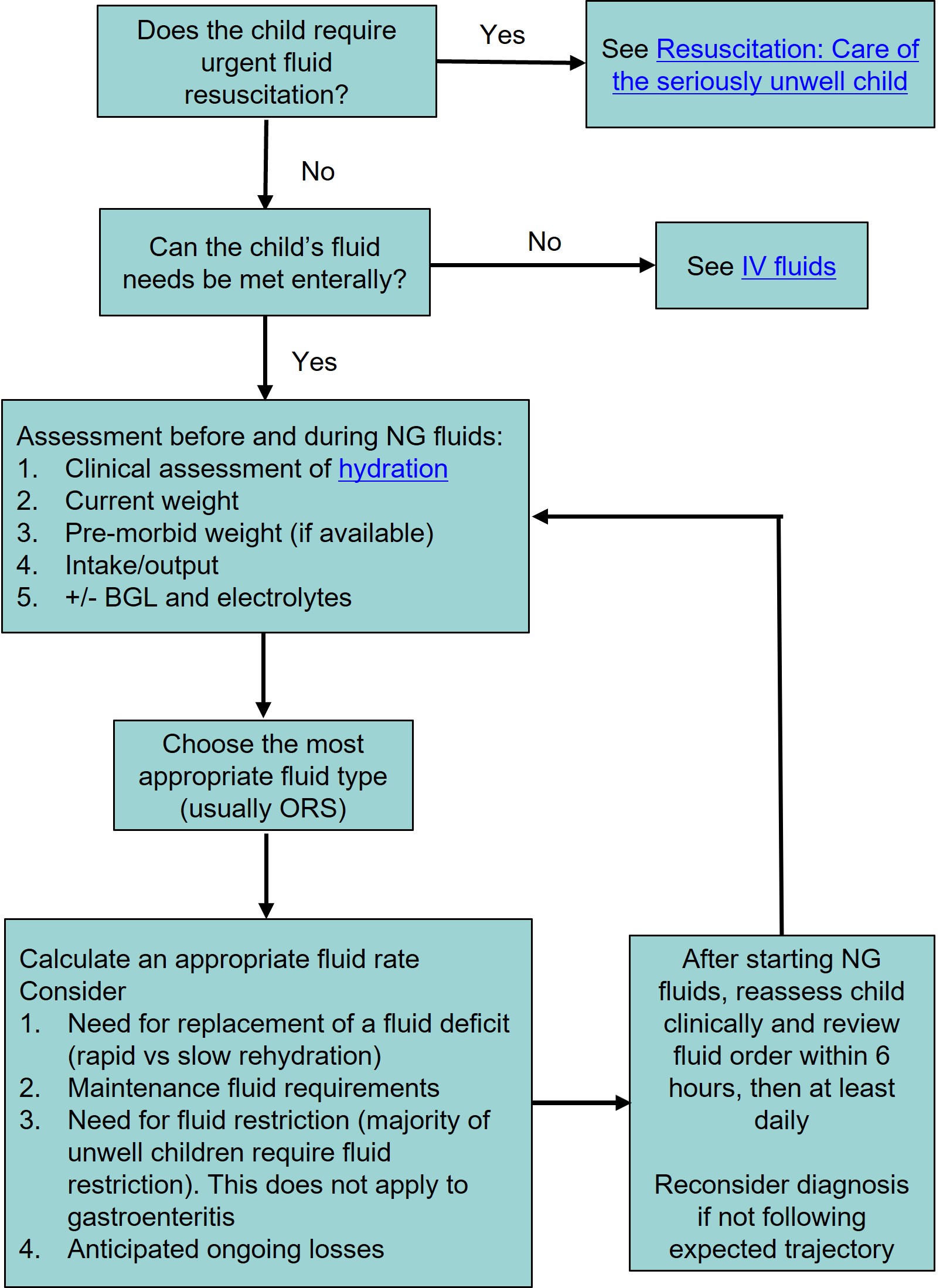
Choice of fluid
Rehydration
- ORS should be used for rehydration in all children over 1 month of age
- While electrolyte content and palatability may differ, there is no clinically significant difference between available ORS fluids
Maintenance
-
An infant who is milk fed should resume their usual feed type (EBM or formula) once rehydration is complete, orally or via NGT if unable to drink
- Cease any fortification (eg concentrated formula or additives) in gastrointestinal illness as higher osmotic load may lead to increased diarrhoeal losses. Consider risk of electrolyte derangement if
fortified feeds continued in other illnesses
- Older children should also transition from ORS to age-appropriate nutrition as soon as possible. ORS can be used as a short-term maintenance fluid if a child is not tolerating oral intake
- If specialised fluids or longer-term enteral nutrition are required, consult with relevant specialty team or dietetics
Calculation of volume and rate
Maintenance fluid rates and fluid restriction
- Maintenance rates can be calculated using this maintenance fluids calculator
- 2/3 maintenance is appropriate for the majority of unwell children requiring hydration support, particularly in respiratory and CNS infections
- Full maintenance fluids may be appropriate for well children who are not drinking adequately (eg fasting for surgery), and in the maintenance phase of gastroenteritis
Maintenance fluid requirements calculated by the '4:2:1 rule'
| Weight (kg) |
Full maintenance mL/day |
mL/hour |
| 3 – 10 |
100 x weight |
4 x weight |
| 10 – 20 |
1000 + 50 x (weight-10) |
40 + 2 x (weight-10) |
| 20 – 60 |
1500 + 20 x (weight-20) |
60 + 1 x (weight-20) |
| >60 |
2400 mL/day is the normal maximum amount |
100 mL/hour |
Note
- The calculation of maintenance fluid requirements by the '4:2:1 rule' (see maintenance fluid requirements table below) provides adequate enteral hydration, but may be substantially less than the usual feeds that a well infant drinks
- Younger babies need a higher volume of enteral milk (150-200 mL/kg/day. See table in Additional notes) to meet nutritional and growth requirements, but this higher volume should not be used as a basis for maintenance fluid
prescribing in unwell children
- Infants can return to their usual feed volumes in mild illness or in the recovery phase
Administration
- NG fluids can be run continuously (rapid or slowly) or as bolus feeds, depending on the clinical scenario
- Continuous feeds may be better tolerated where there is respiratory distress, vomiting or diarrhoea
- Bolus feeds at age and condition-appropriate intervals are often well tolerated and can provide comfort (eg 3-hourly feeds in mild-moderate bronchiolitis, or in recovery phase)
- Breast feeding can usually continue during both rapid and slow rehydration
Rapid NG rehydration
- Used to correct moderate dehydration in common illnesses where the goal is to expedite clinical improvement for discharge to home care (eg gastroenteritis)
-
Not suitable in (See slow NG rehydration section below):
- dehydration from lower respiratory tract infections, meningitis or significant electrolyte abnormalities
- age
<6 months
- significant comorbidities present
- abdominal pain
- Children with severe dehydration need IV fluid resuscitation
- Use ORS at 10-25 mL/kg/hr for 4 hours (See hourly rate range table below)
- There is evidence for rapid rehydration at a rate of 25 mL/kg/hr. However, some centres recommend rates of 10-12.5 mL/kg/hr. Thus, a range is provided
- Use clinical judgment (see dehydration) and seek senior clinician support if unsure
Hourly rate range for rapid NG rehydration (not intravenous rehydration)
| Weight on admission |
10 mL/kg/hr |
25 mL/kg/hr |
Total infusion time |
| 7 kg |
70 mL/hr |
175 mL/hr |
4 hrs |
| 8 kg |
80 mL/hr |
200 mL/hr |
4 hrs |
| 9 kg |
90 mL/hr |
225 mL/hr |
4 hrs |
| 10 kg |
100 mL/hr |
250 mL/hr |
4 hrs |
| 12 kg |
120 mL/hr |
300 mL/hr |
4 hrs |
| 14 kg |
140 mL/hr |
300 mL/hr* |
4-4.5 hrs* |
| 16 kg |
160 mL/hr |
300 mL/hr* |
4-5.5 hrs* |
| 18 kg |
180 mL/hr |
300 mL/hr* |
4-6 hrs* |
| 20 kg |
200 mL/hr |
300 mL/hr* |
4-6.5 hrs* |
* Maximum rate of many NG pumps is 300 mL/hr. If rate exceeds pump maximum rate, divide target volume of fluid by 300 mL, eg for 18 kg child, if aim is 450 mL/hr for 4 hours (1800 mL), this can be given as 300 mL/hr for 6 hrs
Slow NG rehydration
- Preferred in children with moderate dehydration and conditions where high/rapid fluid volumes are not appropriate
- In the first 24 hours: replace 5% fluid deficit over the first 6 hours. Clinically reassess, and if ongoing hydration support is required, give daily maintenance volume over the next 18 hours. To calculate rate, see slow NG rehydration
table below
- Subsequent 24 hours: Replace remaining deficit if still indicated, in addition to daily maintenance volume
Recommended hourly rate for slow NG rehydration
| Weight on admission |
Rate of slower NG rehydration
(Moderate dehydration - replaces 5% deficit plus maintenance) |
| Weight |
mL/hr
0-6 hrs
(Deficit replacement – based on 5% deficit) |
mL/hr
7-24 hrs
(Full 24-hour maintenance volume, over remaining 18 hours) |
| 3 kg |
25 mL/hr |
15 mL/hr |
| 4 kg |
35 mL/hr |
20 mL/hr |
| 5 kg |
40 mL/hr |
25 mL/hr |
| 6 kg |
50 mL/hr |
30 mL/hr |
| 7 kg |
60 mL/hr |
40 mL/hr |
| 8 kg |
70 mL/hr |
45 mL/hr |
| 9 kg |
75 mL/hr |
50 mL/hr |
| 10 kg |
85 mL/hr |
55 mL/hr |
| 12 kg |
100 mL/hr |
60 mL/hr |
| 15 kg |
125 mL/hr |
70 mL/hr |
| 20 kg |
165 mL/hr |
80 mL/hr |
| 30 kg |
250 mL/hr |
95 mL/hr |
After rehydration
- Aim for a rapid return to age-appropriate fluids and nutrition. Breastfeeding should continue
- There is no benefit to gradual reintroduction of milk after rehydration, nor to giving dilute milk or formula
- Usually, no dietary restrictions are required. If increased diarrhoeal losses after lactose-containing or high fructose fluid and foods, consider a 1-2 week period of lactose free milk/formula and avoidance of fruits/juice
Replacement of ongoing losses
- In addition to maintenance rates, consider the need for replacement of ongoing losses, including diarrhoea, vomiting, drain output
- Losses can be replaced mL for mL with ORS. Calculations may be based on each previous hour or each 4-hour period, depending on the situation eg 200 mL of diarrhoea over 4 hours can be replaced with ORS at 50 mL/hr over the next 4-hour period
Fluid balance
Assessment of hydration status at least daily is required to titrate NG fluid requirements
Repeated weights are the best measure of fluid status. Weight should be taken at the start of treatment and then at least daily. In addition, document inputs and ongoing losses (including urine output), with at least 12 hourly subtotals
If vomiting occurs, slow fluids temporarily and consider ondansetron if ≥6 months age (see Vomiting)
If significant abdominal pain or ongoing vomiting, seek senior clinician review
Consider consultation with local paediatric team when
- Severe dehydration
- Electrolyte or glucose abnormalities
Consider transfer when
Children requiring care above the level of comfort of the local hospital.
For emergency advice and paediatric or neonatal ICU transfers, see Retrieval services
Additional notes
Standard enteral fluid volumes (ie EBM/formula) to meet nutritional and growth requirements in well children
| Age (months) |
mL/kg/day |
| 0-3 months |
150-200 |
| 4-6 months |
130-150 |
| 7-9 months |
120-150 |
| 10-12 months |
90-100 |
Last updated April 2026