Table of contents will be automatically generated here...
Introduction
Skeletal injury in childhood is common, due largely to patterns of childhood play and behaviour. It also has complexities absent in the adult, because the child's skeleton is more flexible than the adult's, and actively growing.
Approximately 15% of extremity fractures in children involve disruptions of the growth plate, which is 2 - 5 times weaker than any other structure in the paediatric skeleton.
The rest of the paediatric skeleton has different mechanical properties, as well as greater plasticity, than that of the adult. This explains the unique nature of some paediatric fractures (i.e. torus fractures, greenstick fractures and plastic deformation) and
the relative infrequency among children of fracture propagation and comminution.
Although the "severity" of fractures is usually less in the paediatric trauma victim than in the adult, it must be remembered that the elastic nature of a child's bones allows a greater level of energy absorption prior to the fracture. This needs to be
remembered, so the degree of the soft tissue trauma associated with a fracture is not underestimated.
Spinal injuries are rare in children, but due to their clinical importance, a high index of suspicion needs to be maintained in trauma situations. This is particularly true of the cervical spine and flexion distraction injuries in the lumbar spine. (
See chapter 1.12 for Spinal Injuries)
|
Injury type
|
Number of injuries
|
|
Upper arm (including clavicle/ scapula/ shoulder joint)
|
406
|
|
Lower arm (including elbow joint)
|
1,581
|
|
Hand (including fingers and wrist joint)
|
359
|
|
Pelvic ring
|
45
|
|
Upper leg (including hip joint)
|
209
|
|
Lower leg (including knee joint)
|
391
|
|
Foot (including toes and ankle joint)
|
86
|
|
Total
|
3,077
|
In all aspects of trauma management,
the primary survey is the first priority
Primary survey
Extremity assessment in primary purvey
Limb trauma is rarely life threatening. During the primary survey, only those musculoskeletal injuries that may be life-threatening, due to loss of blood or spinal cord injury are included.
Examples include
-
Pelvic fractures/crush injuries
-
Traumatic proximal amputations
-
Multiple open or closed fractures
1. Pelvic fractures
(see
radiology section)
Excluding a significant pelvic fracture is an essential part of any trauma assessment.
An AP pelvis x-ray is required in all trauma patients except in those who are:
-
Conscious
-
Cooperative
-
Have no distracting injury
-
Have no effects of drugs or alcholol
-
Are haemodynamically stable
-
Show no signs or symptoms which could be attributable to a pelvic fracture.
This image is required early (with lateral cervical spine) if there is unexplained haemodynamic instability.
If there is any doubt, the pelvis AP X-Ray should be performed as part of the initial trauma series.
Pelvic fractures may be
With the exception of isolated superior or inferior pubic rami fractures, they should all be discussed with the senior member of the Orthopaedic Unit.
Paediatric pelvic fractures rarely require operative fixation, and are only occasionally life-threatening.
They do, however highlight the possibility of visceral, genito-urinary and neurological injury. (see
chapter 1.8 for uretheral injury)
Examination
-
The examination for pelvic stability is an important part of the trauma assessment.
- Anterior/posterior stability is tested by grasping the ASIS - Anterior Superior Iliac Spine regions bilaterally, and performing an open book manoeuvre.
-
Lateral displacement of the pelvic wings suggests instability.
- Vertical instability can be assessed by checking the relative heights of the ASIS and the leg lengths. Any discrepancy may suggest vertical instability in the hemipelvis.
-
Any signs of instability should prompt urgent consultation with an Orthopaedic surgeon.
-
With any suspicion of urethral injury, seek surgical opinion re catherisation
-
Any unstable pelvis fracture will require a retrograde urethrogram prior to catheterisation.
-
In the presence of a stable pelvic fracture without obvious signs of urethral injury, a single attempt at catheterisation can be made.
-
Discuss with orthopaedic and surgical consultants prior to transfer.
Haemodynamic instability
If signs of haemodynamic instability are also present, a PELVIC BINDER or large sheet can be wrapped around the pelvis at the level of the ASIS, and tied tightly to "close the book".
2. Amputation
-
Make sure the patient's airway is open, and that breathing and circulation are adequate.
-
Place the patient in a position of comfort, but only if doing so does not compromise stabilisation of the head and cervical spine!
-
Control the bleeding by applying an appropriate sterile dressing directly on the wound.
-
Assess for shock. If shock is present, treat for shock.
-
Elevate the stump above the level of the patient's heart.
-
Saturate the sterile dressing and stump with sterile saline.
-
Cover the dressed stump with a dry bandage.
-
If bleeding cannot be controlled, apply pressure on the appropriate arterial pressure points. Use a tourniquet only as a last resort.
-
Preserve the amputated part as follows:
-
Moisten appropriately-sized sterile gauze with sterile saline solution.
-
Wrap the severed part in the moistened sterile dressing, preserving all amputated material.
-
Place the severed part in a watertight container (plastic bag).
-
Place the container on ice or cold packs (if available).
Do not freeze or use dry
ice
Transportation of the patient should
not be delayed to search for amputated parts! Leave word as to
destination, and indicate how to preserve the amputated parts to
the person in charge at the scene of the accident.
3. Open fractures
-
Great confusion surrounds the clinical decision of what dictates an open fracture.
-
The most useful approach is to assume that any wound in close proximity to a fracture communicates with that fracture.
Simple Guide Grade 1
<1 cm wound Grade 2 1-10 cm wound Grade 3 >10 cm wound
-
Broad-spectrum antibiotics should be administered, typically, first generation cephalosporins +/-aminoglocosids if severe (Grade 3).
-
Tetanus immunization status should be checked.
-
Add penicillin if gross contamination with soil, etc. This should be removed and wounds should be covered with sterile dressings.
-
Wound should be viewed once, covered with sterile dressing, and then only reviewed by the Orthopaedic team for a definitive care decision.
-
If possible, polaroid or digital photographs should be taken prior to covering the wounds, in order to limit the number of times the dressing is disturbed , increasing chances of later deep-wound infection.
-
Control bleeding with direct pressure and do not attempt to ligate or clamp bleeding points in conditions of poor light and equipment, for fear of causing further vascular damage or damage to adjacent structures (e.g. nerves).
-
Review of tetanus status (see chapter 1.24)
-
Obtain and record the patient's vital signs. Repeat en route as often as the situation indicates.
-
Transport, keeping the patient warm.
-
Record all patient care information, including the patient's medical history and all treatment provided.
Secondary survey
-
The secondary survey is only to be commenced after the primary survey has been completed, and the child is stable.
-
Continue to monitor the child fully
-
Reassess -A B airway, respiratory rate, oxygen saturation -C heart rate, blood pressure, capillary refill time -D mental state
-
If there is any deterioration detected in these parameters, the primary survey MUST be repeated immediately, and measures taken to rectify the problem.
-
During the secondary survey, a systematic head-to-toe examination is carried out involving the front and the back of the child, top-to-toe.
Included in this will be
Spinal assessment
All trauma patients require log-roll and assessment of the thoracolumbar spine by inspection and palpation.
-
If conscious and cooperative, without back pain or signs of injury, no x-rays are required.
-
If any of these criteria cannot be met, AP and lateral views of the spine are required to exclude injury to the spine.
-
Until the spine can be cleared, continue spinal immobilisation and spinal precautions.
-
Vigilance for flexion distraction injuries to the lumbar spine is particularly important.
-
This injury is classically sustained by a lap-seatbelt-restrained child and is commonly associated with duodenal and/or pancreatic injury.
Limb assessment
The examination should include:
- Inspection: for discolouration, deformity, swelling and wounds.
- Palpation: gently for warmth, pulses*, capillary refill, tenderness and crepitation.
- Active movement: if the child is cooperative
- Passive movement: Excluding the cervical spine, and not when there is an obvious extremity fracture or dislocation, as further soft tissue injury may be inflicted unnecessarily.
It is important during this stage to identify limb-threatening injuries, including
1. Vascular injury
The cardinal signs of vascular injury are quoted to be:
-
Abnormal (absent or reduced) pulses;
-
Impaired capillary return;
-
Decreased sensation;
-
Rapidly expanding haematoma;
-
Overlying bruit;
-
(N.B. Pallor and reduced temperature compared to the uninjured side can also be important signs)
Unfortunately, the presence of a pulse on Doppler examination, or by palpation, does not exclude the possibility of significant vascular injury. Therefore, constant reassessment must be maintained. The presence or suspicion of vascular injury should be
urgently discussed with a vascular specialist.
2. Compartment syndrome
Compartment syndrome occurs with injuries producing a rise in the interstitial pressure within a closed (or only partially-opened) osseofascial compartment, to the point that tissue circulation is compromised.
-
Injuries with high risk for compartment syndrome -High energy injury -Tibial shaft fracture (especially open) -Forearm fracture -Supracondylar fracture -Crush fracture of the foot.
-
The cardinal clinical features include:
- Pain out of proportion to the injury
- Pain, which is not controlled with standard
analgesia
- Pain on passive stretching of muscles in
compartment
-
Firmness of compartment on palpation
-
Diminished sensation of nerves passing through
compartment (late).
- Skeletal muscle remains electrically responsive for up
to 3 hours after the onset of total ischaemia, and peripheral
nerves conduct impulses for an hour after complete
ischaemia.
-
Because tissue perfusion in a compartment is dependent on arteriolar and capillary perfusion gradients rather than systolic arterial pressure, compartment syndrome can occur despite the presence of peripheral pulses, capillary refill, and lack of pallor.
- Pain and aggravation of pain by passive stretching of
the muscles in the compartment in question are the most sensitive
(and generally the only) clinical findings before the onset of
ischemic dysfunction in the nerves and muscles.
-
Thus the presence of limb injury with a high risk of compartment syndrome in an obtunded trauma patient will require careful monitoring of his/her compartment pressures.
- Distal pulses only disappear late in the clinical
process, and by this time irreversible muscle damage has
occurred.
Treatment
-
Constant neurovascular observation - pulses/perfusion/ peripheral nerves/motor/sensory.
-
Early review by Orthopaedic Unit, if suspicious.
-
Release constricting dressing /split plaster to skin. Re-evaluate.
-
Orthopaedic urgent review if no resolution of symptoms.
-
Fasiotomies may be necessary.
Limb fractures
| Clavicle |
Femur |
| Humerus |
Tibia |
| Radius and Ulna |
Ankle and Tarsus |
| Metacarpals |
Metatarsals |
| Phalanges Hand |
Phalanges Foot |
Assessment
-
Suspect a limb fracture where there is pain or swelling, deformity or loss of function of any limb.
-
Examine the child for other injuries ie other fractures, head or abdominal injuries.
-
Examine the affected limb carefully for neurovascular injury (as above).
-
Realign and splint the fracture early - a plaster slab is often useful as a temporary measure.
-
Joint dislocations should be reduced and splinted as soon as possible, especially ankle, hip, and knees.
-
Immobilising in a position of relative alignment can achieve significant analgesia, as well as improvements in skin/limb perfusion to the limb.
-
Provide adequate analgesia (
see chapter 1.20).
-
X-ray all suspected fractures, including joints above and below.
-
Consider whether this could be a non-accidental injury
-
Consider any differential diagnoses i.e. septic arthritis, osteomyelitis, and acute leukaemia.
-
With a history of minimal trauma and atypical bony architecture, consider pathological fracture.
-
Assess the fracture radiologically and describe it according to the Salter-Harris classification.
Salter Harris Classification of
Fractures
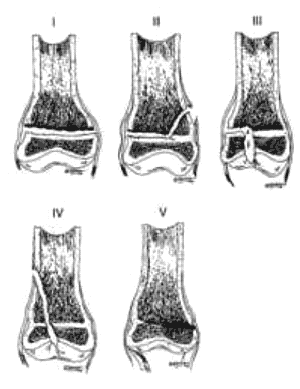
Reduction
Decide whether the fracture requires reduction.
-
Urgent reduction may be required where there is skin or vascular compromise, or in joint dislocations. Occasionally this is required prior to x-ray, particularly in the case of ankle or subtalar fracture dislocation.
-
If in any doubt, seek an opinion from the Emergency Consultant or Orthopaedic Registrar.
-
At RCH, reductions of selected fractures are performed in the Emergency Department under appropriate anaesthesia ( Bier's block) by accredited personnel.
Always obtain post-reduction X-rays to ensure that the position of the fracture is acceptable in plaster. Always check post-reduction renovascular status. A change should prompt consultation with an Orthopaedic surgeon.
Plaster care and follow-up
Every child who is to be discharged with a fracture must have appropriate discharge and follow-up arrangements in place.
Plaster instructions
If a plaster has been applied, verbal instructions regarding plaster care and the dangers of encircling plasters must be given to the parents or guardian. In addition, the "Plaster instructions" Parent Information Leaflet should be given to the parents or
guardian.
Plaster checks
If an encircling plaster has been applied, a plaster check should be arranged for the following day, preferably by the patient's GP. A covering letter to the GP is required.
General practitioner follow-up
Undisplaced greenstick fractures or fractures (such as a fractured middle-third of clavicle), which are unlikely to require further treatment, may be referred to the patient's GP for follow-up.
Fracture Clinic
All other fractures should be followed up in the Fracture clinic. Most fractures should be followed up in 7 days with an Xray performed prior to the clinic.
Analgesia
Ensure the patients have access to adequate analgesia for their child and are aware how to use it.
Specific management of upper limb fractures
Clavicle
Right clavicular fracture
a. Middle third Sling for 2-3 weeks.
-
Inform parents of the lump that will develop at the fracture site, and may be visible for up to one year.
-
No contact sports for six weeks.
-
No review of re-Xray necessary.
b. Medial/lateral third - Seek advice.
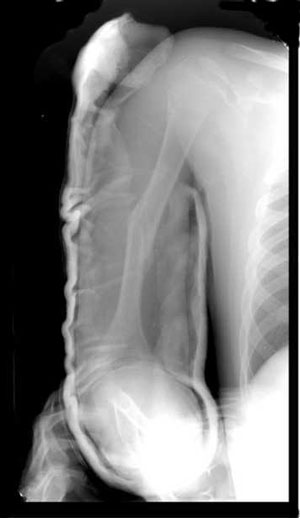
Humerus
Surgical neck fracture
a. Surgical neck
-
Undisplaced - sling for 3 weeks, follow in fracture clinic in 7 days.
-
Displaced - frequently treated with sling alone - seek advice.
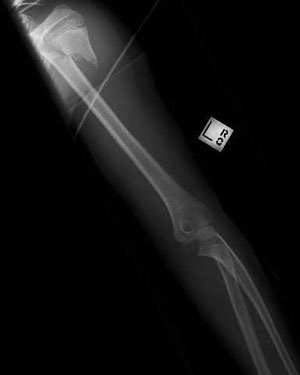
b. Shaft
Humerus shaft fracture
-
Check the integrity of the radial nerve
-
Undisplaced - collar and cuff. A "U"-shaped plaster slab may be applied to the humerus to reduce movement and minimise knocks.
-
Transverse/displaced/comminuted: seek advice.
c. Supracondylar
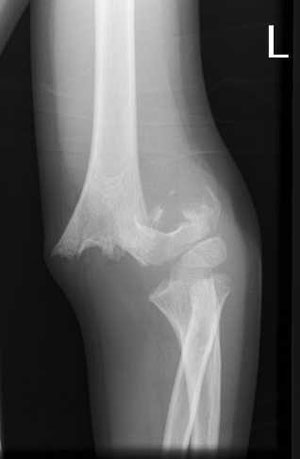
Supracondylar fracture
-
Specifically, check the integrity of the radial artery, radial nerve, median nerve and ulnar nerve.
-
If vascular compromise, extend the elbow until perfusion returns. Avoid excessive flexion.
-
Undisplaced - collar and cuff with elbow flexed. A "sleek" gusset across the elbow can be helpful to maintain elbow flexion, but ensure there is no compression or tension placed on the tissues. Place stockingnet over arm and torso. (Ensure maintenance
of normal distal neuro/vascular examination).
-
Angulated/displaced/comminuted: seek advice.
d. Epicondylar:seek advice.
e. Intra-articular: seek advice.
Radius and ulna
a. Shaft
-
Undisplaced - above-elbow plaster, fracture clinic with Xray in 7 days.
-
Displaced: seek advice.
b. Distal end
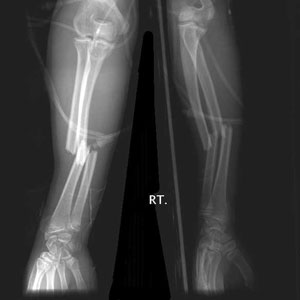
Radius and ulna fracture
-
Undisplaced and non-deformed clinically - above elbow plaster, fracture clinic with Xray in 7 days.
-
Displaced and clinically deformed - LAMP in emergency department. For further information, see Local Anaesthetic Manipulation Procedure (LAMP) Guidelines.
-
If contraindications to LAMP - admit under Orthopaedics for GAMP
-
Above elbow plaster, fracture clinic with Xray in 7 days.
-
Totally displaced with fracture-ends not touching, General Anaesthetic Manipulation Procedure (GAMP) in theatre.
Metacarpals
Check carefully for rotation at fracture site.
-
Undisplaced - volar slab, fracture clinic with Xray in 7 days.
-
Displaced - seek advice.
Phalanges (hand)
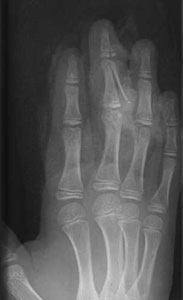
Fracture of middle finger
-
Check carefully for rotation at fracture site, or mallet-finger deformity.
-
Intra-articular fractures require anatomical reduction.
-
Undisplaced - strap to adjacent finger, fracture clinic with Xray in 7 days.
-
Displaced - seek advice - some may be reduced under digital block.
Lower limb fractures
Femur
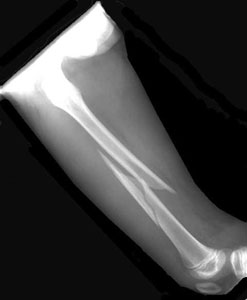
Femur fracture
-
Ensure adequate analgesia with entonox, opoids and a femoral nerve block. Neurovascular status must be documented prior to nerve block administration.
-
Apply simple skin traction using skin traction kit.
-
Admit under Orthopaedics.
Tibia
Tibial fracture
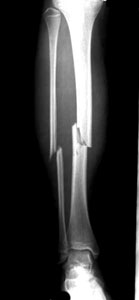
-
Undisplaced - above knee plaster, fracture clinic with Xray in 7 days.
-
Displaced - may need manipulation, admit under Orthopaedics.
-
Toddlers' fracture - a clinical diagnosis in a child where a fractured tibia is suspected on clinical grounds, but an abnormality is not detected on the Xray by the treating doctor.
-
Exclude septic arthritis/osteomyelitis
-
Apply an above-knee plaster for pain relief, allow weight-bearing, as child desires.
-
Fracture clinic in 7 days.
Ankle and Tarsus
Medial malleolar
-
Undisplaced - below knee plaster, fracture clinic with Xray in 7 days.
-
Displaced - will need manipulation or open reduction. Admit under orthopaedics.
Metatarsals
Fracture 1st metacarpel / cuniform /navicular / distal calcaneum
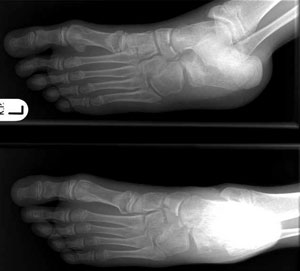
-
Undisplaced - lower leg plaster slab, fracture clinic with Xray in 7 days.
-
Displaced - seek advice; may need admission under Orthopaedics.
Phalanges (foot)
-
Undisplaced - padded bandage, fracture clinic with Xray in 7 days.
-
Displaced - reduce under entonox, digital block, seek advice.
Joint injuries
Elbow dislocation
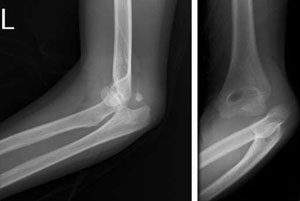
-
Joint injuries incorporate a wide spectrum of injuries in trauma, from open dislocations of large joints down to subtle ligamentous instabilities of small joints.
-
Peri-articular fractures can be difficult to distinguish clinically from dislocations or fracture-dislocations, and sensible use of appropriate imaging modalities is vital for timely and effective treatment.
-
Severe deformity of a limb at or near a joint can produce severe compromise of the soft tissue envelope, and this is particularly true around the ankle where prolonged dislocation can lead to skin necrosis.
-
Traction in the long axis of the limb will reduce most of these dislocations or fracture-dislocations without causing any significant harm. In the case of the complete arterial occlusion in severely displaced humeral supracondylar fractures or proximal
tibial fractures, correction of alignment with gentle traction may re-establish circulation to the limb.
-
Rapid swelling of a joint (within minutes or 1-2 hours) suggests a haemarthrosis and significant intra-articular damage. Disruption of the joint capsule at the time of injury may allow intra-articular bleeding to escape from the confines of the joint,
producing more diffuse swelling of the region. In the lower leg, it can be associated with compartment syndrome. Swelling occurring
-
over several hours is usually due to synovial fluid, but can still represent significant injury to the joint.
-
Any puncture wounds adjacent to joints (especially the knee and the metacarpophalangeal joints) must be assumed to communicate with the joint, and so will require exploration, debridement and thorough irrigation. This is usually best performed in an operating
room with a tourniquet and good quality lighting.
-
In young children, the presence of multiple ossification centres and the large proportion of unossified cartilage, can make the interpretation of plain radiographs difficult. If doubt exists regarding the appearance of a joint on plain films, a comparison
film of the contralateral joint should be utilised (especially with regard to the elbow).
References / further reading
-
Roche C, Carty H. Spinal trauma in children. Pediatr Radiol 2001; 10:677-700.
-
Musgrave DS, Mendelson SA. Pediatric orthopedic trauma: principles in management Crit Care Med 2002; 11:431-43.
-
Flynn JM, Skaggs DL, Sponseller PD, Ganley TJ, Kay RM, Leitch. The surgical management of pediatric fractures of the lower extremity. Instr Course Lect 2003; 52: 647-59.
-
Flynn JM, Sarwark JF, Waters PM, Bae DS, Lemke LP. The surgical management of pediatric fractures of the upper extremity. Instr Course Lect 2003; 52:635-45.
-
Whitesides TE Jr, Heckman MM. Acute compartment syndrome: Update on diagnosis and treatment. J Am Acad Orthop Surg 1996; 4: 209-18.
-
Existing clinical practice guidelines for cervical spine and fractures . Internet resource at Royal Children's Hospital, Melbourne Australia.