Table of contents will be automatically generated here...
Introduction
Children
differ from adults anatomically, physiologically, cognitively and
psychologically. The aim of this chapter is to outline these differences, and
how they influence the assessment and management of traumatic injury in
childhood. These differences will be discussed with regard to their impact on:
- Mechanism of injury
- Pattern of injury
- History
- Examination and management
Different mechanism of injury
Trauma
is the greatest contributor to childhood mortality[i]. Childhood
activities and the changing levels of maturity of children expose them to
different risks to adults. Children are more likely to fall from playground
equipment, suffer sporting and playground accidents than be involved in motor
vehicle or industrial accidents like their parents. They are, therefore, at risk in proportion to their
level of cognitive, physical and social development.[ii]
- Infants reach and grasp for objects, placing them in their mouth before 4 months of age; they roll at 3-5 months, and "cruise" around furtniture at 8-12 months. As a result, they are at risk from inhaled foreign bodies and falls. The majority of infants sustain their injuries at home.
- Pre-schoolers (1-4 years) have increased mobility and curiosity, without a refined awareness of hazards or dangers - so falls, burns and unintentional ingestions characterize the types of injury in this age group
- School age children (5-9 years) are increasingly developing skills such
as cycling, climbing and other forms of active play. Falls from playground equipment / trampolines
are common causes of injury.
Older children and adolescents
consciously engage in risk-taking behaviours, there is an increase in road
traffic accidents, assault, intentional self-harm and intoxication.
[i] Australian Institute of Health and Welfare. 2016. Leading causes of death (AIHW). [ONLINE] Available at: http://www.aihw.gov.au/deaths/leading-causes-of-death/#leading-age. [Accessed 08 March 16].
[ii] Australian Institute of Health and Welfare. 2014. Hospitalised injury in children and young people 2011-12: Injury Research and Statistics Series No.91. [ONLINE] Available at: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=60129549323. [Accessed 08 March 16].
Different patterns of injury
When involved in the same kind of accident as adults, children may suffer quite different injuries because of their different size, anatomy and physiology.
Airway injuries
Infants and small children have
smaller airways – minor injuries and slight swelling can rapidly compromise
their ability to breath. A similar
injury in different aged children can raise different concerns, and have
varying consequences. For example, nasal fractures are common in
adolescents (especially in those playing contact sports) and rarely need
immediate intervention. However, the
same injury in an infant, who is an obligate nose breather, may require immediate
assistance. Such injuries are rare in small
children – given their limited mobility and smaller, more protected noses, so
if present, a nasal injury in these age groups should raise the suspicion of
non-accidental injury.
Chest injuries
Thoracic injuries are a
significant cause of mortality in paediatric trauma. The lack of complete ossification of the ribs
and sternum mean the underlying structures are less well protected – leading to the potential for pulmonary / mediastinal injury to occur without significant signs of external injury. Children also have a relative lack of physiological reserve and higher metabolic rate can
lead to rapid desaturation in children.
Abdominal injuries
As with their thorax, the abdominal contents of children are relatively unprotected due to a thin abdominal wall with less fat and underdeveloped musculature. The liver and spleen are less protected by the rib cage and are thus at greater risk from blunt abdominal trauma. Common mechanisms of injury include motor vehicle accidents and handlebar injuries. Any bruising of the abdomen - in particular the "seat belt" sign - signifies an increased risk of intra-abdominal injury. However, the compliance of the abdominal wall means significant injury can exist with only non-specific or subtle external signs.
Head and neck injuries
Young children, with relatively
large heads and underdeveloped musculature sustain higher proportions of isolated
head injuries than older children.[i] Traumatic Brain Injury is the leading cause
of death in paediatric trauma patients. Young children are also more likely
to injure their upper C-spine region (as opposed to the lower C-spine in
adults) for the same reason - however due to the types of accidents they have cervical spine injury is rare in childen. Spinal cord injuries are
relatively uncommon in the paediatric trauma patient – however, children less
than 8 may be susceptible to SCIWORA (spinal cord injury without radiological
abnormality).
Extremities and Exposure
Blunt trauma may result
in bone fractures in the adult population, while the cartilaginous nature of
children’s bones tends to prevent them from fracturing. However, lack of a
fracture does not mean absence of injury. Protective equipment and
clothing can be harder to obtain for children compared to adults. The varying and
constantly changing sizes of growing children make correct sizing of helmets,
car restraints and so on difficult and expensive for families. Older children may succumb to peer group
pressure and refuse to use protective wear such as knee splints, wrist guards
and helmets. Finally, the larger surface area /
volume ratio puts children at greater risk of hypothermia following their
trauma.
Non-accidental injuries
Suspicion may be aroused
by:
-
Delay in seeking medical
treatment for a significant injury
- Inconsistencies in the history
provided – either over time, or between caregivers
-
A history / mechanism of injury
that isn’t consistent with the child’s developmental stage (for example a
1-month old “rolling” off a bed).
-
Obvious caregiver impairment – (eg appearing intoxicated)
-
Allegation of non-accidental injury raised by either caregiver
or child
It
is important to remember that age is one of the most important risk factors in
non-accidental injury – with the majority of abusive fractures being seen in
children <12 months.
Some
injury patterns are more suggestive of a non-accidental injury:
- Bruising
in children <9months old
- Bruising
to the face, ears, buttocks, back or hand
- Bruising
in the shape of an object / ligature
- Posterior
rib fractures
- Multiple
injuries, with fractures at different stages of healing
Where
non-accidental injury is suspected, local policies must be followed. This typically involves consultation with a
senior clinician, social worker and forensic medical service. Where there are immediate safety concerns Child
Protection Services need to be contacted to ensure the safety of that child or
their siblings.
[i] Bayreuther J et al. Paediatric trauma: injury pattern and mortality in the UK. Arch Dis Child Educ Pract Ed 2009. 94(2):37-41
Differences in taking a history
Given the wide spectrum of injuries sustained by children and
their range of developmental stages, health care practitioners need to be
skilled at obtaining a history from parents, care-givers, children and other
health-care providers. Consideration
should always be given to whether the mechanism of injury described is
consistent with the child’s developmental age.
AMPLE is an acronym used for gathering a brief history of
patient and event in the context of a minor injury.
A Allergies – in children
this may be unknown
M Medications - typically fewer than in the adult population
P
Past
medical history - Children are generally healthy and don’t usually present with
complex medical histories. However, practitioners should ask about previous
injuries – a history of recurrent presentations with injuries may raise
suspicion for NAI.
L
Last
ate - important if procedural sedation is
required or the patient needs to go to theatre
E
Event -
what happened?
Immunisation and birth history are also important elements of the history which need to be documented:
- Immunisation status
- All children are given routine immunisations during early childhood. It is
important to check from the schedule if the presenting child is up to date or
will need immunisation.
- Birth history
- As children get older, this becomes less significant. However, in the infant
and young child, details of birth history may be important. Postnatal
respiratory difficulties may contribute to a condition worsening beyond what
would be expected based on the injury.
Where children
are more severely injured, they may arrive at hospital via the emergency
services. It is common in this situation to use a
formal handover tool such as the IMIST - AMBO tool. This acronym stands for:
- I Identification
- M Mechanism
of injury
- I Injuries
detected
- S (Vital)
Signs
- T Treatment
started / given
- A Allergies
(if known)
- M Medications
- B Background
conditions
- O Other information
Examination and management
Primary survey
The function of the
Primary Survey is to rapidly identify and manage immediate life threats. It focuses on the following:
- catastrophic haemorrhage control
- Airway with cervical spine
protection
- Breathing
- Circulation and haemorrhage
control
- Disability
- Exposure
Airway
Paediatric airway is smaller
- In the small airway, there is greater risk of airway obstruction from small foreign bodies.
- Children with loose deciduous teeth may have one dislodged into the airway.
- Small amounts of swelling of the smaller paediatric airway, will result in a relatively greater reduction in airway diameter than would occur in the larger airway of the adult.
Relatively larger tongue and smaller oral
cavity
- The relatively larger tongue and smaller oral cavity means that, in the child, the tongue is more likely to obstruct the airway than in the adult. This makes it essential that there is correct positioning of the head jaw to open the airway.
Infants have a relatively larger
occiput
- The large occiput of the infant flexes the head forward when he/ she is placed prone on a flat surface. This is important in airway-opening manoeuvres and cervical spine immobilisation.
To achieve a neutral position, it may be necessary to lift the chin or place a pad under the torso of the infant. - Care must be taken not to hyper-extend the neck, as this may result in airway obstruction or spinal cord damage in the event of a cervical spine fracture.
Infants are nose breathers.
- In the first 4-6 months of age infants breathe exclusively through the nose, and will experience respiratory distress if the nose is blocked. Care must be taken to ensure that the nares are patent in cases of infant trauma.
Trachea is more cartilaginous and soft
- The cartilaginous nature of the paediatric airway makes it more subject to collapse and obstruction than the adult airway if the child is not positioned appropriately.
- The tonsils in toddlers and young children may be enlarged, contributing to airway obstruction and making nasal passage of an endotracheal tube difficult.
Larynx is higher and more anterior.
- The larynx sits at the level of the 2nd - 3rd cervical vertebrae in the young child, compared with the 6th -7th cervical vertebrae in the adult.
- The positioning of the larynx makes its visualisation in the paediatric airway more difficult than in the adult.
- This has huge implications for intubation. A more detailed discussion of endotracheal intubation is included in Chapter 1.3
Only an experienced clinician should
attempt intubation in the young child.
Shape of the epiglottis
- The epiglottis of the young child is horseshoe-shaped and projects posteriorly at 45o. This makes the technique of tracheal intubation more difficult.
Cricoid ring is the narrowest point in the
airway
- This also has implications for endotracheal intubation.
- The clinician is not able to confirm endotracheal tube size by viewing the tube pass through the narrowest section of the airway, as in adult intubation.
- The cuff of the endotracheal tube sits at the level of the cricoid ring, which then takes up valuable airway diameter. In addition, the cricoid region is lined with pseudo-stratified, ciliated epithelium bound to areolar tissue, which is susceptible
to oedema. For these reasons, an uncuffed endotracheal tube is used for paediatric intubation.
The trachea is short
- The paediatric trachea is comparatively shorter than that of the adult, which increases the risk of dislodgement of the endotracheal tube. Techniques for securing the airway are discussed in chapter 1.3.
Cervical Spine
- Larger head, in particular in the occipital region. This has been previously discussed with regard to the airway. However, it is also very important in cervical spine alignment. The ligaments of the paediatric vertebral column are relatively lax, compared to
those in the adult spinal column. This increases the likelihood that movement of vertebrae may occur, resulting in injury to the normal spinal cord (i.e. spinal cord injury without radiographic abnormality [SCIWORA])
- The fulcrum is at C1 - 2 not C 6 - 7. Therefore, cervical spine injuries in children under the age of eight most commonly occur in the first three vertebrae, whereas in the adult, injuries tend to be lower in the vertebral column.
Breathing
Ribs positioned more horizontally
- The ribs of the infant are positioned more horizontally than those of the adult. This means that with inspiration the ribs only move up, and not up-and-out, like the adult rib cage. This limits the capacity to increase tidal volumes.
Adult chest x-ray showing arched ribs:
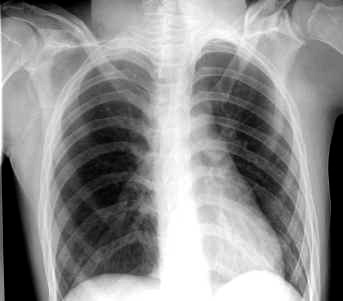
Neonate chest x-ray showing flattened ribs:
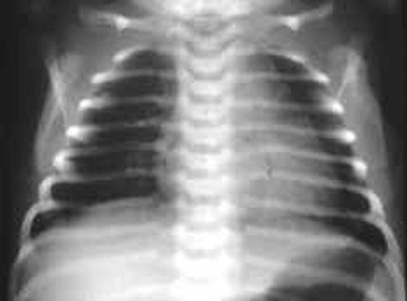
Thin chest wall
- Upper and lower respiratory noises can be referred to other areas of the chest when auscultating, making it difficult to localise adventitious sounds.
Diaphragmatic breathing
- In infancy, the diaphragm is the most significant respiratory muscle. It is important to decompress the stomach where possible, to stop it impinging on diaphragmatic excursion.
- The greater compliance of the chest wall in infants and young children also explains the significant intercostal retraction that occurs in children when the airway is obstructed, or there is a decrease in lung compliance.
Intercostal retraction:

Fewer Type 1 fibres in respiratory muscles
- Infants and young children exhaust more quickly than adults, because of the smaller number of fatigue-resistant, Type I fibres in their respiratory muscles.
Respiratory rate varies with age
- Young children have significantly higher metabolic rates than adults, and therefore have a higher oxygen demand, which in turn results in higher respiratory rates.
- However, the normal respiratory rate in young infants varies greatly, and consequently respiratory rate should be interpreted in light of other respiratory findings. Normal respiratory rates for various age groups are provided in
Appendix 1 at the end of the chapter.
Heart rate
- Heart rate will be influenced by respiratory insufficiency. Infants become bradycardic when hypoxic.
Circulation
Blood volume is relatively larger, but absolute volume is smaller
- Neonates have 85-90ml/kg compared to 75-80ml/kg in infants, 70-75ml/kg in children and 65-70ml/kg in adults
- Relatively small volumes of blood will constitute significant blood loss in small children, ie: a 100ml haemorrhage experienced by a 5 kg child represents the loss of approximately 10% of their total blood volume.
- Monitor and record all blood loss, including amounts that would be insignificant in the adult patient.
- The size of the child will also determine the amount of fluid required for fluid resuscitation. This will be discussed in greater detail in
the fluid management documentation.
Systemic vascular resistance is lower
- Systemic vascular resistance increases from birth to adulthood, and is evident in the increase in blood pressure as the child grows. Appendix 1 at the end of the chapter provides normal blood pressure values for different age groups.
Hypotension is a late sign
- Children have very efficient compensatory mechanisms, and will remain normotensive until they have lost large intravascular volumes (25%).
Renal tubule Urine Volume - Urine output is commonly used to assess circulatory adequacy.
- Urine output = 1-2 ml/kg/hr in children/infants
- Urine output = 0.5 ml/kg/hr in adults
Fixed-stroke volume
- To increase cardiac output, infants are limited to increasing their heart rate as they are unable to increase stroke volume.
Smaller vessels / more subcutaneous tissue
- It is often extremely difficult to obtain vascular access in young children and infants, due to the size of their veins and the increase in subcutaneous tissue during infancy.
Relatively healthy cardiovascular system - The cardiovascular system of the infant and child is generally healthy. So fluid resuscitation is less of a concern than in adults, where cardiac disease is more prevalent.
Disability - Central Nervous System (CNS)
Open sutures, presence of fontanelle
- The anterior fontanelle can be palpaed in most children up to the age of 12 - 18 months before it closes permanently, and the posterior fontanelle may be palpated in some children up to the age of 2 months.
- It is important to recognise a bulging or sunken fontanelle and the relevance of these findings.
- In the trauma setting, the bulging fontanelle will suggest a rise in intracranial pressure, which may be a result of intracranial bleeding.
- The sunken fontanelle may suggest significant intravascular losses.
- The cranial sutures do not fuse until the head has reached adult size, providing some limited protection to the brain tissue by allowing limited expansion.
Thinner cranial bones
- The thinner cranial bones of children do not afford as much protection to the brain tissue as the thicker bones of the adult skull.
Head relatively larger
- The proportions of head to body in the infant and small child are significantly larger than in the adult. This will result in greater heat loss from the surface of the exposed head.
- The size of the head relative to the body also results in a higher centre of gravity, which in turn contributes to a higher incidence of head trauma in children.
Cognitive and psychological development varies with
age
- Variation in the developmental age of the child will impact on the strategies used to evaluate and manage neurology.
Exposure
Relatively small size
- The smaller the child, the greater the likelihood that a single impact will injure multiple organ systems.
Higher BMR and surface area
- The higher metabolic rate results in greater consumption of oxygen and other metabolites, and for this reason, higher respiratory and heart rates.
- The larger surface-area to body-mass ratio results in greater heat loss for infants and children.
Increased glucose requirements but decreased glycogen
stores
- A higher metabolic rate results in increased glucose usage.
- Infants have relatively small glycogen stores when compared with those of an adult. For this reason, it is essential to monitor plasma glucose in sick and injured infants.
Secondary survey
Chest
Chest wall is more compliant.
- Blunt chest trauma may not result in a rib fracture in the infant and young child, due to the increased elasticity and compliance of the chest wall.
- However, the force may be transmitted through the cartilaginous ribs to the underlying structures, which may sustain significant internal injuries.
Increased mobility of the mediastinal
structure
- The increased mobility of the mediastinum increases the likelihood that the injured child may develop a tension pneumothorax from a simple pneumothorax, or transect a small mediastinal vessel as the mediastinum shifts.
Abdomen
Relatively thin abdominal wall
- The abdominal wall in children is relatively thin, comprised of less muscle and subcutaneous fat than in adults.
- For this reason, the abdominal wall in children provides less protection to abdominal organs.
Abdominal organ proportions and placement
- Trauma to the abdominal region is more likely to result in liver or spleen damage in the child compared to the adult, as these organs take up a greater proportion of the abdominal cavity in the child.
- The bladder in infants is an intra-abdominal organ, increasing the risk of bladder damage in abdominal trauma.
Diaphragm is more horizontal
- The diaphragm of the child is flatter and less dome-shaped than that of an adult, and consequently, tends to push the liver and spleen lower below the rib cage
Musculoskeletal
Growth plates not fused
- The epiphyseal plate does not fuse until children reach skeletal maturity, which occurs after puberty.
- Until this time, fracture through the growth plate can seriously affect future growth of the fractured bone.
- Assessment and management of the fracture may differ significantly for this reason. This will be discussed in greater detail in Chapter1.14.
- The presence of an open growth plate and areas of cartilage will also influence radiograph interpretation.
Cartilaginous bones
- The bones of children are more cartilaginous and flexible than those of adults, and for this reason, green stick fractures are common in children i.e: fracture of supracondylar rather than dislocation of elbow.
Conclusion
Children and infants differ, both anatomically and physiologically, from adults. These differences will have an impact on the assessment and management of paediatric trauma. However it is important to recognise that the basic principles of trauma care
- airway, breathing and circulation - remain the same, regardless of the age of the patient.
Appendix 1
Normal paediatric vital signs by age group
| Age group |
Respiratory rate |
Heart rate |
Min Systolic BP |
| Term baby |
40-60 |
100-170 |
50 |
| 3 month |
30-50 |
100-170 |
50 |
| 6 month |
30-50 |
100-170 |
60 |
| 1 year old |
30-40 |
110-160 |
70-90 |
| 1-2 years |
25-35 |
100-150 |
80-95 |
| 2-5 years |
25-30 |
95-140 |
80-100 |
| 5-12 |
20-25 |
80-120 |
90-110 |
| >12 years |
15-20 |
60-100 |
100-120 |
Reference List
Advanced Life Support Group. (1997). Advanced Paediatric Life Support. (2 ed.). London: BMJ Publishing Group.
Manley, L. K. (1987). Pediatric trauma: Initial assessment and management. Journal of Emergency Nursing, 13(2), 77-87.
Ojanen Thomas, D. (1988). The ABC's of Pediatric Triage. Journal of Emergency Nursing, 14(3), 154 - 159.
Semonin-Holleran, R. (1991). Paediatric trauma patients: Differences and implications for emergency nurses. Journal of Emergency Nursing, 17(1), 24 - 33.
Soud, T. (1992). Airway, breathing, circulation, and disability: what is different about kids? Journal of Emergency Nursing., 18(2), 107-16.