Causes
Facial
nerve palsy can occur from a variety of causes. It can be present at birth due
to a developmental issue or it can occur from a number of acquired conditions.
From birth, it can also occasionally be associated with a syndrome. There are
approximately 50 known causes of facial palsy with the most common being due to
Bell’s palsy which is thought to be caused by a viral infection. This can occur
in both children and adults. Another main cause in children is developmental or
congenital facial palsy where the child is born with a facial palsy. Some of
the causes are listed below.
Congenital
- Developmental
- Moebius
Syndrome
Acquired
Infectious
- Bells Palsy
- Middle Ear Infections
- Ramsay Hunt
- Leprosy
Metabolic
Neoplastic
- Brain tumour
- Schwannoma
- Parotid Malignancy
- Cholesteotoma
Neurologic
- Guillain-Barre
- Multiple Sclerosis
- Myasthemia Gravis
- Iatrogenic
- Birth Trauma
Surgery
- Acoustic Neuroma
- Parotid Gland
Tramatic
- Fractured Base of Skull
- Penetrating wounds to face
Anatomy
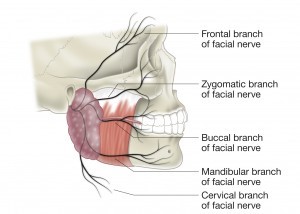
figure 1.
The anatomy of the facial nerve and its course from
the brain stem to the muscles of the face is complex taking a circuitous route
through the skull (temporal bone) and the middle ear. It exits the skull and
the passes into the parotid gland where it divides into its 5 main branches
(figure 1). From there it passes into the forward dividing more into its
individual muscular branches. Besides having nerve fibres for the muscles of
facial expression it also has nerve fibres for taste buds in the tongue,
salivary and lacrimal gland (tear) function.
Clinical
Interruption of the
nerve anywhere along its length will result in a facial palsy. The site and
cause of the interruption will then dictate the symptoms and signs that each
patient will have. The signs and symptoms will then lead the treating physician
to a potential number of investigations to ascertain what is causing the facial
palsy.
These
investigations may include tests to measure the function of the lacrimal gland
(tear production), salivary glands or taste to the tongue. Hearing tests and
nerve conduction and electromyographic studies may also be required.
Radiological imaging with CT scans and MRI scans are commonly done in the
investigation of someone with facial palsy.
Management
The management of
facial palsy is determined by the cause of the palsy and the duration of it
being present. The management needs to address the cause of the facial palsy as
well as treat the effects resulting from the facial palsy. There are types of
facial palsy that can recover and others that will not recover. The commonest
type of palsy that recovers is a Bell’s palsy, where as a developmental facial
palsy, which a child is born with, usually is permanent. In the management of
Bell’s palsy it is common to be prescribed steroids to help reduce the swelling
of the facial nerve and antiviral medication.
The resultant
facial palsy will affect the face in two ways. The first is a loss of sphincter
function round the eye, mouth and nose with the second being facial asymmetry.
Both of these can be very distressing to the patient. Eye protection is
paramount so that no damage occurs to the front of the eye (cornea) due to the
loss of blink and eye closure. This can be managed with eye drops and
lubricants, taping the eye shut at night and a variety of surgical procedures
including tarsorraphy or insertion of gold weights (Fig 2) or other devices to
improve blink.
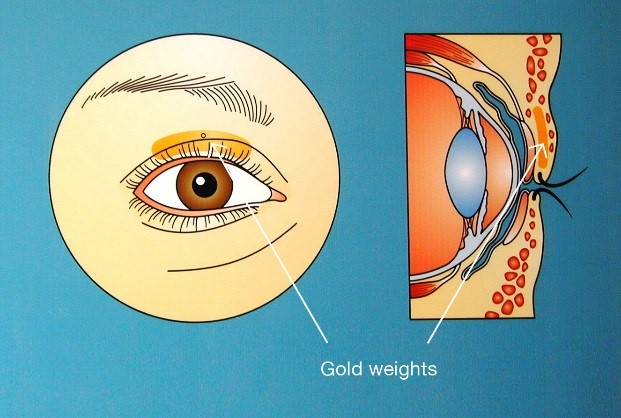
figure 2.
When a facial palsy will not recover then the
duration of the palsy determines the management. Muscles that lose their nerve
supply lose their ability to function in approximately 18 months to 2 years. So
if the patient presents prior to this time frame it may be possible to use a
new nerve supply to make the facial muscles function again. This would be
through utilising nerve grafting or nerve transfer procedures. If the patient
presents later then a number of other surgical options may be required.
The aims of surgery
for reconstruction of facial palsy are to restore facial harmony, protect the
eye, and provide symmetry of the face at rest and with expression with minimal
unwanted motion (synkinesis).
Facial palsy reconstruction
Early surgical options
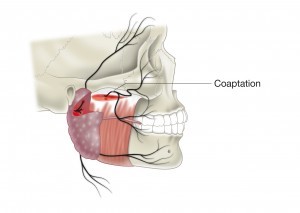
figure 3.
In patients who
have had an injury to the facial nerve through an accident such as a laceration
to the face, head injury with a fractured base of skull or surgical division of
the nerve in tumour surgery and they present with a year of the injury then
nerve grafts and nerve transfers are options available to them. These
procedures provide new nerve fibres to the muscles of facial expression and
restore motion to the face. These options include cross facial nerve grafts,
masseteric nerve transfer (figure 3) and hypoglossal nerve transfers.
Late surgical options
There are two
groups of procedures for patients who present with a congenital palsy or an
established long term facial palsy. These two groups are static procedures
aimed at improving symmetry without providing motion and dynamic procedures
that provide facial motion.
Static procedures
For eye protection
include:
- Gold weight
insertion in the upper eyelid (figure 2)
- Tarsorraphy
(partially joining the eyelids together)
- Palpebral springs
For restoration of
facial symmetry at rest include:
- Nerve / facial
muscle excisions
- Facial slings –
These types of procedures include Tendon or fascial slings to lift up the paralysed
face to minimise facial droop (figure 4).
- Brow, Face and Neck
lifting procedures (figure 5) to restore facial position at rest
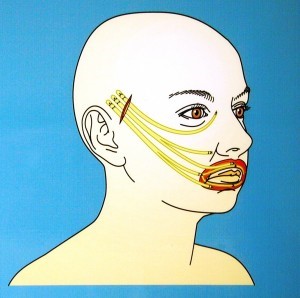
figure 4.
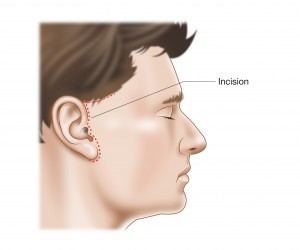
figure 5.
Dynamic procedures
For restoration of
smile - muscle transfer procedures.
The mainstay of
facial reanimation for long term and congenital types of facial palsy are
procedures known as free vascularised muscle transfers where new muscles and
nerves are inserted into the paralysed face to restore facial motion. The most
common muscle used for this is the gracilis muscle in the upper inner thigh,
which is an expendable muscle (figure 6).
A
portion of the muscle is taken from the leg with its own nerve and blood
vessels and transferred into the face to recreate smile with upper lip
elevation. The muscle is inserted into the face through a facelift style
incision and then the blood supply to this new muscle is reconnected to the
blood vessels in the face with the use of routine microsurgery.
The nerve supply to the new muscle is then connected to a new nerve either by a
cross facial nerve graft or to the masseteric nerve in a two stage or one stage
procedure schematically demonstrated in figure 7.
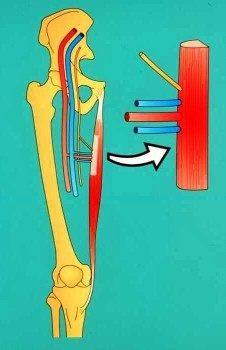
figure 6.
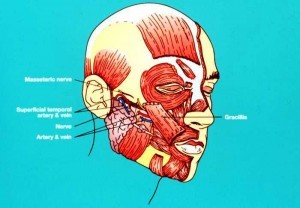
figure 7.