Fracture Guideline Index
See also:
Lateral condyle fracture of the humerus - Fracture clinics
-
Summary
-
How are they classified?
-
How common are they and how do they occur?
-
What do they look like - clinically?
-
What radiological investigations should be ordered?
-
What do they look like on x-ray?
-
When is reduction (non-operative and operative) required?
-
Do I need to refer to orthopaedics now?
-
What is the usual ED management for this fracture?
-
What follow-up is required?
-
What advice should I give to parents?
-
What are the potential complications associated with this injury?
1. Summary
Due to the potential poor outcomes, all lateral condyle fractures require prompt orthopaedic consultation. Prompt recognition and treatment are essential to avoid complications and prevent functional impairment.
Undisplaced fractures can be immobilised in an above-elbow backslab with the elbow flexed to 90 degrees and supported in a sling. Follow-up in fracture clinic should occur within 7 days with x-ray.
Minimally displaced (
<2 mm gap) can be managed with either immobilisation only or closed reduction with percutaenous pinning.
All displaced fractures (>2 mm gap and/or angulation of the lateral condyle) will need to go to theatre either for closed reduction and percutaneous pinning or open reduction.
2. How are they classified?
Lateral condyle fractures involve a fracture line entering into the elbow joint. The Milch classification system (Table1) classifies the fracture according to the location of the fracture line in relation to the capitellar ossification centre.
Table 1: Milch classification of lateral condyle fractures.
|
Type
|
Frequency
|
Description
|
|
.jpg)
|
Rare
|
The fracture line goes through the capitellar ossification centre
Equivalent to a Salter-Harris type IV fracture
|
|
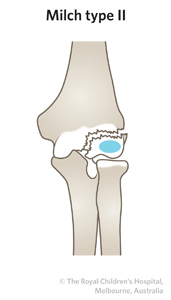
|
Most common
|
The fracture line runs medial to the capitellar ossification centre
Equivalent to a Salter-Harris type II fracture
|
3. How common are they and how do they occur?
Lateral condyle fractures of the elbow are the second most common paediatric elbow fracture after supracondylar fractures. They account for 12-20% of elbow fractures in children. The peak age of incidence is six years.
They usually occur as a result of indirect forces being applied to the elbow following a fall on an outstretched hand. Angular and rotational forces are thought to contribute.
4. What do they look like - clinically?
The child will present with pain, limited elbow range of motion (ROM) and swelling at the lateral aspect of the elbow.
|
|
Lateral condyle fractures can frequently look benign with minimal swelling and minimal deformity, which can lead to delays in presentation and recognition of the fracture. |
5. What radiological investigations should be ordered?
Anteroposterior (AP) and lateral x-rays of the elbow should be obtained without splinting. If there is clinical suspicion of injury in the forearm or wrist then separate films of these areas should be ordered.
If a lateral condyle fracture is suspected or minimally displaced on x-rays, then oblique views are often useful.
|
|
These fractures do not require splinting prior to imaging as there is usually less pain and swelling. This allows subtle fracture lines to be more visible on x-ray.
|
6. What do they look like on x-ray?
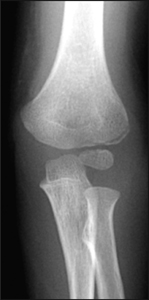
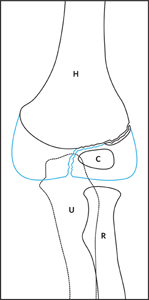
Undisplaced lateral condyle fracture
.jpg)
Figure 1: Three year old girl with an undisplaced fracture of the lateral condyle. An undisplaced lateral condyle fracture may be difficult to see on plain x-ray. The presence of anterior and posterior fat pad signs may be the only clue. Oblique views may be useful in undisplaced lateral condyle fractures.
Minimally displaced lateral condyle fracture (<2 mm gap)
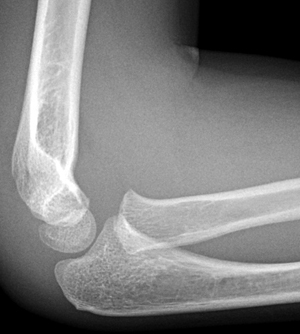
Figure 2: Seven year old boy with a displaced lateral condyle fracture (<2 mm gap). In the AP view, a metaphyseal fracture line can be observed just proximal to the growth plate above the capitellum. On the lateral view, a minimally displaced fracture appears as a second line visible above capitellum.
Displaced fracture >2 mm
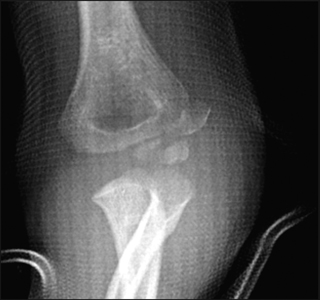
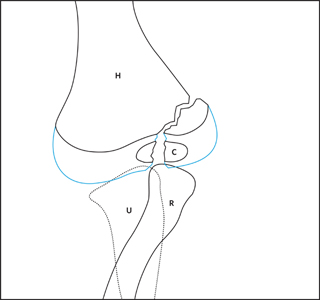
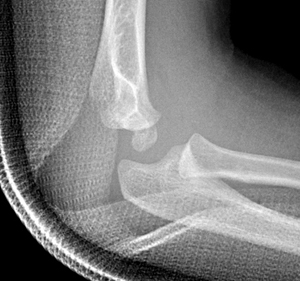
Figure 3: AP and lateral view of a displaced lateral condyle fracture (Milch type I) in a four year old boy. The AP in this instance provides the most useful information. It shows a displaced fracture fragment (>2 mm). The ulna is laterally subluxated. Notice that the majority of the soft tissue is located laterally.
7. When is reduction (non-operative and operative) required?
Undisplaced fractures can be immobilised in an above-elbow backslab with the elbow flexed to 90 degrees. No reduction is required.
Minimally displaced (
<2 mm gap) can either be managed with immobilisation alone or with closed reduction and percutaneous pinning.
All displaced fractures (>2 mm gap and/or angulation of the lateral condyle) will need to go to theatre either for closed reduction and percutaneous pinning or open reduction.
8. Do I need to refer to orthopaedics now?
|
|
Due to the potential for poor outcomes, all lateral condyle fractures require prompt orthopaedic consultation.
|
Patients should be kept nil orally until a decision about surgery is made. For open fractures, tetanus immunisation status should be assessed.
9. What is the usual ED management for this fracture?
All lateral condyle fractures require an orthopaedic consult in the ED (see above). Undisplaced fractures can be immobilised in an above-elbow backslab with the elbow flexed to 90 degrees and supported in a sling.
10. What follow-up is required?
For undisplaced fractures, follow-up in the fracture clinic within 7 days with repeat x-ray is required. It is usually necessary to remove the backslab to obtain adequate views of the fracture at review.
For fractures that go to theatre, follow-up should be arranged by the consulting orthopaedic team.
11. What advice should I give to parents?
The backslab and sling should be worn under clothing (e.g. loose fitting shirt) and not through the sleeve.
Close follow-up is required to ensure that the fracture remains in the correct position.
In the majority of minimally displaced fractures, union will occur. Fractures managed with operative intervention have a high union rate.
12. What are the potential complications associated with this injury?
Complications include:
a) Delayed union (Figure 4)
Figure 4: X-ray series showing delayed union of lateral condyle fracture in a five year old. A) Acute injury showing lateral condyle fracture. B) At one month, minimally healing is evident. C) The fracture required internal fixation.
b) Nonunion: this is a common outcome for nonoperative treatment of displaced lateral condyle. The risks of nonunion increase with increased degree of displacement or angulation of the fragment.
c) Growth disturbance
d) Elbow stiffness
e) Overgrowth at the lateral condyle can cause an unsightly bump on the outside of the elbow
|
|
This fracture has a significant risk of problems if undertreated. Prompt recognition and treatment are essential to avoid complications and prevent functional impairment.
|
See
fracture clinics for other potential complications.
References (ED setting)
Beaty JH, Kasser JR. The elbow: Physeal fractures, apophyseal injuries of the distal humerus, avascular necrosis of the trochlea, and T-condylar fractures. In Rockwood and Wilkins' Fractures in Children, 7th Ed. Beaty JH, Kasser JR (Eds). Lippincott Williams & Wilkins, Philadelphia 2010. p.533-93.
Tejwani N, Phillips D, Goldstein RY. Management of lateral humeral condylar fracture in children. J Am Acad Ortho Surg 2011; 19: 350-58.
Feedback
Content developed by Victorian Paediatric Orthopaedic Network.
To provide feedback, please email rch.orthopaedics@rch.org.au