Key points
- An allergy is when the body’s immune system overreacts to something that is normally harmless.
- The substance that causes an allergic reaction is called an allergen.
- Avoiding triggers is the best way to manage allergies.
- Most allergic reactions are mild, and you can manage them with antihistamine medicine.
- Anaphylaxis is the most serious type of allergic reaction; it is a life-threatening emergency.
- Children with anaphylaxis should always carry their adrenaline device and their Action Plan for Anaphylaxis.
- If your child is having an anaphylactic reaction, you should lie them flat or sit them up, inject them with adrenaline and call an ambulance (000) immediately.
What is an allergy?
An allergy is when the body overreacts to something that is normally harmless. Allergic
reactions happen because the immune system thinks the substance – known as an allergen – is dangerous and tries to fight it off.
Some common allergies include:
Pollens, dust mites and animal fur and dander are unlikely to cause severe allergic reactions.
What causes allergies?
Allergies are thought to be a mix of genetic and environmental factors. If you have allergies, your child is more likely to develop allergies in general, but not your specific allergies.
There are ways to reduce the risk of your child getting allergies, such as:
- Eating a balanced diet, rich in fibre, vegetables and fruit during pregnancy
- Avoiding smoking during pregnancy and/or around your baby
- Breastfeeding for at least six months, if you can
- Introducing solid foods around six months of age when your child is ready
- Slowly giving your child common food allergens in their first year of life, including cow’s milk, wheat, egg, nuts, sesame and seafood.
If your child has eczema, managing their condition well may also reduce their risk of food allergies.
Signs and symptoms of allergies
Mild to moderate allergic reaction
|
Severe allergic reaction (anaphylaxis)
|
Condition
- A reaction that affects different parts of the body.
|
Condition
- A reaction that affects breathing and/or how blood moves around the body. It is an emergency that needs urgent treatment.
|
Common symptoms
- Hives, welts or wheals (red, lumpy rash, like mosquito bites).
- Tingling feeling in or around the mouth.
- Stomach pain and/or vomiting.
- Diarrhoea.
- Facial swelling.
|
Common symptoms
One or more of the following:
- Trouble breathing and/or swallowing.
- Wheezing, coughing or choking.
- Tongue swelling.
- Throat swelling and/or tightness.
- Trouble talking or a hoarse voice.
- Dizziness and/or collapse.
- Pale skin and floppiness (infants and young children).
- For insect bites: stomach pain and vomiting.
There may or may not also be symptoms of a mild to moderate reaction, such as a rash.
|
|
Management
|
Management
- A doctor will prescribe an adrenaline device (such as an EpiPen® or Anapen® autoinjector).
- You and your child (if they are old enough) must know how to use it and always keep it nearby – especially when out of the house.
- Care for it properly so it will work in an emergency.
- Store it at room temperature (not in a fridge and avoid direct sunlight.
- Replace it before the end of the expiry month (usually 12 to 18 months).
- Work with a doctor to prepare a custom ASCIA Action Plan for Anaphylaxis.
- It lists their emergency contacts, known allergens and anaphylaxis first-aid instructions.
- Keep a photo of it on your phone and print copies for your child’s childcare or school.
- Your child could wear a medical alert bracelet or pendant to tell others that they have a serious condition.
|
Your child’s first allergic reaction
The first time your child has an allergic reaction, it is a good idea to note their symptoms and possible triggers. For example, did your child’s skin develop itchy, raised patches after touching a cat? You could take photos of any visible signs as well.
Take your child to see their doctor shortly after their reaction. They may refer your child to an allergy specialist for testing. This usually involves a skin-prick test or blood test.
Make sure to avoid the suspected trigger until you see a doctor. Occasionally, your child may have a more serious reaction the next time they are exposed to the trigger.
What to do during an allergic reaction
Mild to moderate food allergy
An oral antihistamine medicine (liquid or tablet) should help your child with symptoms of mild to moderate allergies. There are three main types of non-drowsy antihistamines: cetirizine, loratadine
and fexofenadine – these are all available over-the-counter at pharmacies. A doctor or pharmacist can suggest the best medicine for your child's needs.
Mild to moderate allergies can take a few hours to get better.
Severe allergy (anaphylaxis)
Your child will need adrenaline (epinephrine) during an anaphylactic reaction. This medicine reverses the effects of anaphylaxis by increasing blood pressure and making it easier to breathe. Antihistamines will not help with anaphylaxis.
Anaphylaxis first aid
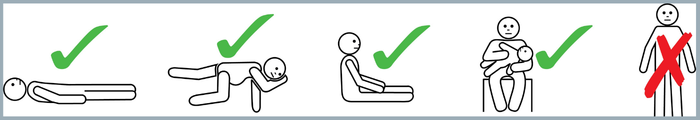
- Lie your child down flat, if possible. If it is hard for them to breathe in this position or difficult to keep them still, sit them up with their legs out.
- Remove the safety cap from the adrenaline device (blue cap on EpiPen®, black needle shield and grey cap on Anapen®) and inject the adrenaline into their outer mid-thigh, with or without clothing. If they do not have an adrenaline device, call an ambulance (000) immediately.
- Call an ambulance (000).
- If your child still shows signs of anaphylaxis after five minutes, you can give them a second dose of adrenaline. This will not harm them.
- Start cardiopulmonary resuscitation (CPR) if your child becomes unresponsive and is not breathing.
After an anaphylactic reaction
Your child will need to be monitored in hospital for at least four hours after an anaphylactic reaction to make sure they are stable. If it is the first time your child has had an anaphylactic reaction, their treating team will talk with you about their
condition, create an Action Plan and prescribe your child an adrenaline device. They will also help you organise follow-up care.
Helping your child avoid allergic reactions
The best way to manage allergies is to avoid known triggers. This is not always easy – especially if your child is allergic to things in the environment like pollen.
- Environmental allergies: Reduce your child’s exposure to their allergen.
- If they are allergic to pollen, try to keep them inside on high-pollen days. You could give them an oral antihistamine before they go outside.
- If they are allergic to dust mites, vacuum their room and living spaces more often, and wash their bedding in hot water every week.
- If they are allergic to animal fur or dander, teach them to keep their distance from pets and wash their hands after touching them.
- Insect allergies: Encourage your child to avoid insects when playing outside. They should also wear shoes.
- If they are allergic to bees or wasps, watch out for any swarms or nests. It is best to get them removed by a professional.
- If they have had an anaphylactic reaction to a stinging insect, they are more likely to have another if they are stung again. Speak to your child’s doctor or an allergy specialist about special treatments for insect allergies.
- Medicine allergies: Tell health professionals about your child’s allergy before they prescribe any new medicine.
- Latex allergies: Inform health professionals of your child’s latex allergy before they touch or treat your child.
- Many medical supplies contain latex, such as gloves, catheters and some bandages.
- Food allergies: Teach your child not to share or swap food with others, and to be careful when eating outside of home.
- If they are eating at a restaurant, it is best to tell the staff about their allergies.
Avoiding allergic reactions at childcare and school
In Victoria, childcare centres and schools must have their own anaphylaxis management policy. They must also train staff on how to prevent and manage allergic reactions.
Talk to your school or childcare centre about your child's allergies and what relevant policies they have in place. It is a good idea to speak with their educators, too.
When to get help
|
Call an ambulance (000) if:
|
- your child is having an anaphylactic reaction (symptoms like trouble breathing and/or noisy breathing, wheeze or persistent cough, throat swelling, dizziness and/or collapse, and stomach pain and vomiting for insect bites).
- use their adrenaline device before calling an ambulance, if they have one.
|
|
Go to a hospital if:
|
- you think your child is having a mild or moderate allergic reaction, but you are not sure how to treat it.
- your child’s reaction is getting worse.
|
|
See a doctor or health professional if:
|
- you think your child has had an allergic reaction for the first time.
- your child is having a mild or moderate allergic reaction, and you have given them antihistamines, but you are still concerned.
|
|
Look after your child at home if:
|
- they are having a mild or moderate allergic reaction, but you are following their Action Plan and they are getting better.
|
Common questions about allergies and anaphylaxis
My child has had a mild allergic reaction to some things. Should I buy an adrenaline device just in case they have an anaphylactic reaction one day?
There is no need to buy an adrenaline device for your child unless a doctor believes they need one. If you are worried about your child’s allergies, it is best to speak with an allergy specialist. They will prescribe your child an adrenaline device
if they believe your child has anaphylaxis or is at greater risk of an anaphylactic reaction.
Do allergies change over time?
Allergies can change over time. Some become more troublesome, and others become milder or completely go away. People may also develop new allergies as they get older. If you are worried that your child’s allergies are getting worse, there are
simple treatments that can help – speak with their doctor.
My child has asthma and anaphylaxis. What are the best ways to keep them safe?
If your child has asthma and anaphylaxis, it is very important for them to control their asthma. This will reduce their risk of serious breathing problems during a severe allergic
reaction. You should take your child to see their doctor if they are using their asthma reliever more than once a week; this is a sign their asthma may not be under control.
If my child is having an anaphylactic reaction and their adrenaline device has expired, should I still give it to them?
Expired adrenaline devices do not treat anaphylaxis as effectively. However, it is still better to use an expired device than no device if that is all that is available in an emergency.
Should my child have their adrenaline device in hospital?
If your child is in hospital, they should have their adrenaline device with them. Make sure to let staff know that they have it. They will ask you about your child’s allergies and let you know where to store the device for quick and easy access.
When you leave the hospital, remember to take the device home. If your child used it in hospital, make sure a health professional gives them a new prescription.
How long after an allergic reaction can my child return to childcare or school?
Your child can return to childcare or school when they are feeling well again and their symptoms have gone away. If they only have a mild reaction, they may be fine within hours. However, if they have a severe allergic reaction, it may take anywhere
from one day to a few days.
My child has been anxious and upset since they had an anaphylactic reaction. What can I do to help them?
Anaphylaxis is a scary experience for anyone to go through. It is important to support your child while they are recovering and encourage them to share how they are feeling. You may want to talk with your child about how they managed their anaphylactic
reaction, and what they should do if it happens again.
If your child is nervous to eat or struggling to get back to their routine after a few weeks, you may want to speak with their doctor about extra support. Allergy and Anaphylaxis Australia also have some great resources about anxiety linked to allergies.
For more information
Developed by The Royal Children’s Hospital Emergency department, with input from the Allergy and Immunology department. We acknowledge the input of RCH consumers and carers.
Reviewed December 2025
Please always seek the most recent advice from a registered and practising clinician.