In the normal shoulder joint, the ball-shaped top of the upper arm bone (humerus) fits into a cup-shaped part of the shoulder bone (scapula). A shoulder dislocation occurs when the “ball” part of the humerus pops out of the “cup” part of the shoulder bone.
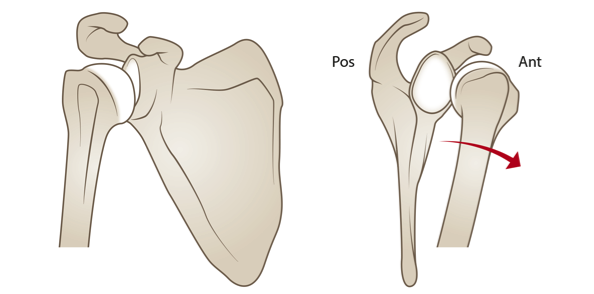
Shoulder dislocation occurs in teenagers much more often than in smaller children.
Signs and symptoms of shoulder dislocation
This injury often occurs when a sudden force is transmitted up the arm to the shoulder, such as when playing sports or from a fall. It can result in damage to the supporting ligaments and occasionally, the surrounding bone structures.
When this occurs the shoulder will be very painful with restricted movement, and will have an abnormal shape.
First aid for shoulder dislocation
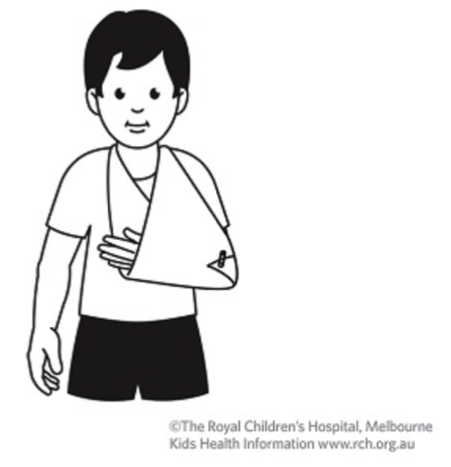 If parents have paracetamol or ibuprofen available, they may give it to their child.
If parents have paracetamol or ibuprofen available, they may give it to their child.
Parents should take their child to the nearest Emergency Department as soon as possible to allow for the shoulder to be relocated (put back into place) under controlled conditions by a medical professional. This is particularly important if it is the first time somebody has had a dislocation, as there are other injuries, such as breaks or fractures that have a similar appearance through an x-ray and it is important to check for them first.
Treatment in hospital
Relocation of the shoulder usually occurs in the Emergency Department, often under some form of sedation. X-rays will be taken again afterwards to confirm that the shoulder is back in position, and to check for any associated injuries. Your child’s arm will be placed in a sling.
Care at home
Applying ice to the shoulder for 20 minutes every three to four hours will be helpful in reducing inflammation, particularly for the first 48 hours after the dislocation. Your child may experience some discomfort, however the relocation of the shoulder should relieve most of the pain associated with the injury. Regular pain relief with paracetamol or ibuprofen may be helpful in the first few days after injury.
The sling should be worn for one to two weeks. The sling may be removed if required during that time, but the upper arm should remain by your child’s side. Your child should avoid reaching overhead or out to the side during this period.
It is a good idea for your child to undertake regular exercises of the elbow, wrist and fingers on the injured arm to stop them from becoming stiff. Your child’s arm may come out of the sling for these exercises, but their elbow should remain tucked against their side.
Here is a suggested routine your child should try approximately every two hours starting the day after their injury:
- Make a fist and then stretch out your fingers, repeat 10 times
- Face your open palm to the roof, rotating the arm to then face the floor, repeat 10 times
- Extend your elbow to point your hand towards the floor, then flex up to touch your shoulder with your fingertips, repeat 10 times.
- Flex and extend at the wrist, repeat 10 times.
Follow-up
Due to the risk of recurrent injury or ongoing shoulder instability, a follow-up appointment for this type of injury is very important.
An orthopaedic surgeon, sports medicine physician or physiotherapist should review the shoulder and the post-relocation x-rays to check to see if the ‘cup’ part of the shoulder blade has been injured, as this increases the chance of the ‘ball’ part of the shoulder slipping out again in the future.
Your orthopaedic surgeon, sports medicine physician or physiotherapist may discuss the option of an MRI to check for features of ongoing instability. There is emerging evidence that this is beneficial, particularly if done early. However, it does involve an additional cost and is not covered by Medicare.
After the sling is removed
Physiotherapy should commence one to two weeks after injury to build up strength in the muscles responsible for shoulder stability. Your child’s physiotherapist or sports medicine physician will discuss any planned return to sport with you and your child, but this should not be rushed.
Key points to remember
- A shoulder dislocation involves the ‘ball’ of the upper arm popping out of the ‘cup’ part of the shoulder blade, but there is often subtle damage done to the surrounding ligaments or cartilage making it easier for the same injury to recur in future.
- It is very important to attend early follow up with an appropriate professional to check for any features of instability. It is possible that this will involve some further imaging.
- A formal physiotherapy program should commence approximately one to two weeks after injury.
- Gentle exercises of the hand wrist and elbow should commence from the day after injury.
For more information
Common questions our doctors are asked
Wouldn’t it be better to leave the sling on for longer?
Whilst the sling is important in the first week to prevent accidental re-dislocation, if it is worn for too long the muscles around the shoulder can start shrinking which itself can contribute to instability. It’s important to get the arm moving again, ideally with the oversight of a physiotherapist.
It’s been a couple of weeks and my child’s shoulder feels fine, can they just skip the follow up?
It is highly recommended that patients attend their follow up appointment due to the chance of recurrent injury and the impact this can have on your child’s ability to play sports. If there are subtle injuries associated with the dislocation that make instability more likely, any surgical treatment of these is much more successful if done early.
Is it important that follow up occur with a specialised paediatric doctor or physiotherapist?
Most dislocations occur in teenagers, in whom the management is very similar to adults. Your local orthopaedics, sports medicine and/or physiotherapy service will have the appropriate skills to assess and manage this injury.
Developed by The Royal Children's Hospital Emergency and Orthopaedic departments. We acknowledge the input of RCH consumers and carers.
Developed September 2020
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit
www.rchfoundation.org.au.