Translated resources
This page is available in 16 community languages.
Please note: the information on these translated pages is not an exact translation of this page.
Key points
- Asthma is a common condition that affects the lungs and airways.
- It causes the muscles around the airways to tighten and become inflamed, making it harder to breathe.
- There are two main types of asthma medicine: preventers and relievers.
- Make sure your child knows how to take their asthma medicine, and that you understand how to help them.
- If your child has asthma, they should have an Asthma Action Plan. They should always have access to their action plan, along with any asthma medicine they need.
- Call an ambulance (000) immediately in an asthma emergency.
What is asthma?
Asthma is a common condition affecting the airways. These are the passages that allow air to flow into and out of the lungs.
People with asthma have sensitive airways. When something triggers a reaction in their airways, three main changes cause symptoms and make it harder to breathe:
- The airways get swollen and inflamed
- The inflammation creates a sticky mucus that clogs up the airways
- The thin muscles inside the airways tighten and get narrower. This makes breathing harder.
Many children will outgrow asthma before they start high school. While there is no cure for the condition, almost all children with asthma can play sport and lead active lives with the right treatment and management.
Asthma flare-ups
When asthma symptoms get worse than normal, it is called a flare-up, exacerbation, episode or asthma attack. A flare-up can happen quickly or develop slowly.
Air gets trapped inside the lungs during an asthma flare-up. This makes it harder to breathe in and out (especially out), causing symptoms like wheezing and coughing.
Why do some people get asthma?
Experts do not yet know why some people develop asthma and others do not. However, there are some clear risk factors, such as:
- Family history of asthma
- Other allergic conditions like eczema, hay fever and food allergies
- Exposure to environmental triggers, such as cigarette smoke.
Wheezing is very common in babies and toddlers, but not all children who wheeze have asthma. Doctors can diagnose children with asthma from their first birthday onwards. However, most will grow out of it as they get older.
What causes asthma?
Many things can cause an asthma flare-up in someone with asthma. The most common is a viral respiratory infection, such as the common cold.
Other common asthma triggers include:
- exercise
- changes in the weather or windy conditions
- allergens such as dust mites, pollen or animal fur
- cigarette smoke or vape mist
- pollution
- some medicines.
Even the smell of cigarette smoke on clothes or furniture can trigger an asthma flare-up. Avoid smoking or vaping in your home, car or around your child.
While it is not always possible to predict an asthma flare-up, it is helpful to know possible triggers so you can reduce your child’s risk. Some children need daily medicine to prevent asthma symptoms; others only get symptoms in certain situations –
for example, after playing sport.
Signs and symptoms of asthma
The symptoms of asthma can vary from mild to severe.
Mild asthma flare-up
Most asthma flare-ups are mild. They will often last two to three days, or sometimes longer.
The three most common signs of a mild asthma flare-up are: trouble breathing, wheezing and coughing.
Trouble breathing
Your child may:
- feel out of breath while resting
- breathe fast
- have tightness in their chest
- need to work harder to breathe
- not be able to talk normally due to feeling out of breath.
- lack energy.
Wheezing
Wheezing is when your child’s breathing makes a high-pitched whistling sound – usually heard when your child breathes out.
Coughing
Coughing from asthma usually happens:
- at night or in the early hours of the morning
- when the temperature is cool
- during exercise.
If your child has a cough without wheezing or breathing problems, asthma may not be the cause.
Severe asthma flare-up
A severe asthma flare-up is more serious. Your child may:
- struggle to breathe and become very upset
- find it hard to speak a full sentence
- feel lethargic or very tired
- make deep sucking movements in their throat or chest
- have a worsening cough or wheeze.
Asthma emergency
An asthma emergency can be life-threatening. Your child may:
- be extremely short of breath
- not be able to speak more than one or two words at a time
- feel very drowsy and exhausted
- go limp or lose consciousness
- have a blue tinge around their lips.
How to care for asthma
The goal of asthma care is good asthma control. This generally means:
- Symptoms less than twice a week
- No need for care in a hospital emergency department
- No need for oral steroids
- No limits on physical activity.
See a doctor
If your child has problems breathing, wheezing or coughing, you should speak to their doctor about asthma. The more you can share about your child's symptoms, the better. Think about whether certain things seem to trigger their symptoms – for example,
do they get worse when they have a cold, pat a cat, or after exercise?
A doctor may give them asthma medicine to see if it helps, if they suspect your child has asthma.
Get an Asthma Action Plan
An Asthma
Action Plan explains how to prevent and manage asthma flare-ups. If your child has asthma, work with their doctor to create a customised Asthma Action Plan. You should review the plan with your child's doctor every twelve months, or sooner if their
condition changes.
Keep your child’s Asthma Action Plan in a place where you can easily find it, and ensure anyone caring for them knows they have asthma and what to do during a flare-up. It is a good idea to take photos of the plan on your phone. You should also print
copies for your child to carry with them and to give to their childcare or school.
Avoid asthma triggers
Help your child avoid things that you know can cause asthma symptoms. For example, if pollen triggers their asthma, you may want to keep them inside on forecast high-pollen days. If dust gives them symptoms, you may need to vacuum their room more often.
Know your medicines
There are two common types of medicine for children with asthma: relievers and preventers.
Both medicines come in different forms, but most are inhaled through the mouth, so they get to the lungs where they are needed. Some common devices are: metered-dose inhalers or ‘puffers,’ and dry-powder inhalers.
Relievers
- Control asthma flare-ups when they happen
- Relax muscles inside the airways so that air can get through more easily
- Works very quickly – usually in minutes
- Used during an asthma flare-up or sometimes before exercise to prevent symptoms.
Preventers
- Prevent asthma flare-ups and manage symptoms
- Reduce swelling and inflammation, and dry up mucus
- Needs to be taken every day, even when your child is well.
If your child has a preventer and/or reliever, they should see their doctor regularly. The doctor will check their dose and make sure the medicines are working properly.
It is very important to learn how to use asthma medicines, so you can support your child and make sure they get a full dose of medicine. If your child uses a puffer, they should always use a spacer to make sure more of the medicine gets to their lungs, where it is needed.
Asthma management in children
In September 2025, the Australian
Asthma Handbook updated its guidelines for managing asthma in children and young people. Below are the current guidelines for different age groups in Australia. Some young people will need other treatment, based on their symptoms.
|
Under six years
|
Six to 12 years
|
Over 12 years
|
Recommended treatment
- Reliever when symptoms occur.
- Preventer for children with frequent asthma flare-ups or ongoing and difficult symptoms.
|
Recommended treatment
- Reliever when symptoms occur.
- Preventer for children with frequent asthma flare-ups or ongoing and difficult symptoms.
|
Recommended treatment
- Inhaled anti-inflammatory reliever (AIR) when symptoms occur.
- Single-inhaler maintenance and reliever therapy (SMART).
- When the same inhaler is used every day as a preventer and as a reliever when symptoms occur.
|
Common medicines
- Reliever: Salbutamol
- Preventer: Fluticasone propionate or montelukast.
|
Common medicines
- Reliever: Salbutamol
- Preventer: Ciclesonide, fluticasone, montelukast or budesonide-formoterol.
|
Common medicines
- Reliever and preventer: Budesonide-formoterol.
|
What to do during an asthma flare-up or emergency
Asthma flare-up
Follow your child’s Asthma Action Plan during an asthma flare-up. It will explain what to do and whether to increase their medicine dose.
Monitor your child's condition as you follow their Action Plan. Over time, it should get easier for them to breathe, and their other symptoms should ease. However, if their symptoms come back or do not stop, and reliever medicine does not help, this is
an asthma emergency.
Asthma emergency
An Asthma Action Plan should advise what to do in an emergency, based on your child’s condition and medicines. Refer to these instructions if you can.
You can also follow the four steps of asthma first aid (sometimes called ‘4x4x4’):
- Sit your child upright. Try to stay calm.
- Give your child four separate puffs of a Salbutamol reliever puffer (usually blue or grey).
- First, shake the puffer.
- Attach a spacer, if available.
- Put one puff into the spacer, then ask your child to take four breaths from the spacer. You may hear a click as they breathe.
- If you do not have a spacer, your child should have four puffs directly from the puffer. Give them one puff at a time and ask them to take one slow, deep breath in and hold it as long as they can. Repeat four times.
- Wait four minutes. If your child’s asthma does not improve, give four more puffs, then wait four more minutes.
- Call an ambulance (000) immediately if your child still cannot breathe properly. Keep repeating step two while you wait for the ambulance.
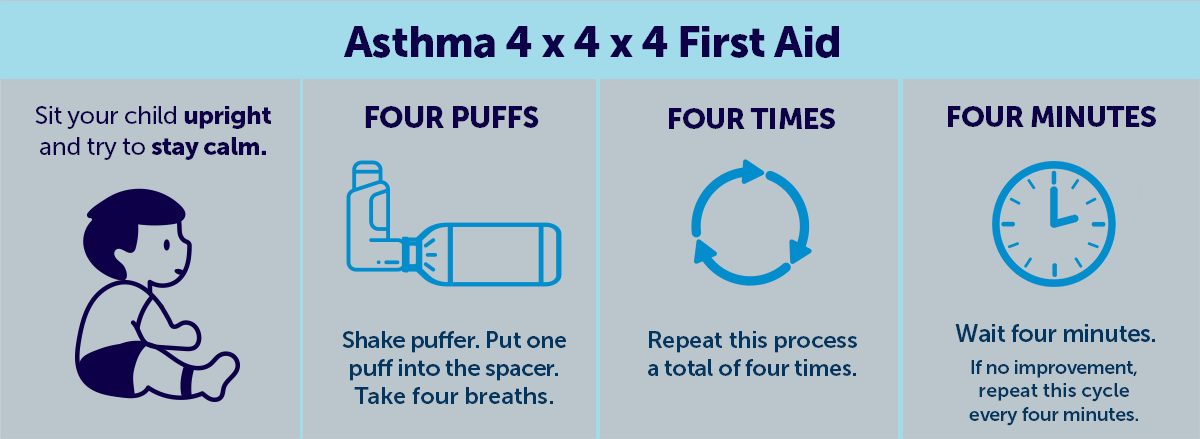
Figure one: Graphic showing the four steps of asthma first aid.
Other asthma medicines have different emergency instructions. For example, if your child has a Terbutaline inhaler, they will only need two puffs instead of four. Follow instructions for other medicines in your child’s Asthma Action Plan.
After an asthma flare-up or emergency
Your child should see their doctor within a week of an asthma flare-up or emergency to make sure they have fully recovered. This is a good chance to review their Asthma Action Plan and ask any questions, such as when they can return to sport. If your
child does not have a preventer, you may want to discuss whether it may help.
When to get help
Call an ambulance (000) if:
|
- your child has asthma symptoms, but has never had asthma before.
- your child is struggling to breathe.
- your child is drowsy or has a blue tinge around their lips.
- your child has trouble talking in sentences.
- your child is having an asthma emergency.
- asthma first aid is not working.
|
|
Go to a hospital if:
|
- your child is very upset with fast or noisy breathing.
- your child is tired or limp with fast or noisy breathing.
- your child makes deep sucking movements in their throat or chest as they breathe.
- your child needs to use asthma reliever medicine at home more than every three hours.
|
|
See a doctor or health professional if:
|
- you have managed your child’s asthma flare-up at home, using their Asthma Action Plan, and they are recovering.
- your child is working harder to breathe than normal.
- your child still seems unwell after three days.
|
|
Look after your child at home if:
|
- they only need to use their asthma reliever medicine every three to four hours and are otherwise well.
- their condition seems stable, and you are confident you are managing their symptoms well.
|
Common questions about asthma
What is thunderstorm asthma?
Thunderstorm
asthma is a type of asthma caused by high pollen levels and thunderstorms. It is not common but can be sudden, serious and life-threatening. Your child may be at risk of thunderstorm asthma if they have asthma or seasonal allergies like hay
fever (allergic rhinitis). People who have hay fever but have never had asthma can also get thunderstorm asthma.
Should I wake my child to give them asthma medicine if they are asleep?
You generally do not need to wake your child to give them asthma medicine unless they are coughing, wheezing or struggling to breathe. If your child does not have obvious asthma symptoms and they are not working hard to breathe, then you do not
need to wake them.
Is it safe for my child to play sport if they have asthma?
If your child’s asthma is under control, it is safe for them to play sport and lead an active life. You should encourage them to join activities with their peers – there is no need to restrict what they do. Exercise is generally helpful for children
with well-managed asthma. If your child’s asthma worsens when they play sport, it may be best for them to use their reliever 15 to 30 minutes before. Speak with their doctor or a pharmacist for advice.
Should my child take antibiotics when they have a cold to prevent an asthma flare-up?
Antibiotics do not prevent asthma symptoms or flare-ups. They do not help with colds, either, as viruses cause most colds and antibiotics cannot kill viruses.
Why does my child need a preventer?
A doctor may suggest your child use a preventer if they have frequent asthma flare-ups or ongoing and difficult symptoms. Your child will need to use their preventer every day for it to be effective. This should reduce their risk of asthma flare-ups.
Is it safe for my child to have the steroid, prednisolone?
You may have heard about possible side effects from prednisolone. These side effects include poor sleep, increased appetite and mood changes. Longer-term problems can happen when the medicine is given for long courses, months at a time, or repeated
courses, a few days each. Prednisolone is usually only an emergency treatment for serious breathing problems, where the benefits outweigh the side effects. Speak with your child’s doctor or a pharmacist if you have questions about prednisolone.
How long after an asthma flare-up can my child go back to childcare or school?
Your child can safely go back to school or childcare when they only need to use their reliever medicine once or twice a day. Most children may need one day at home to recover after an asthma flare-up. If your child has a viral infection that caused
their asthma to get worse, they should stay at home until they are well again.
What is SMART for asthma treatment?
SMART stands for ‘Single-inhaler Maintenance and Reliever Therapy.’ It is also called MART. In SMART, people use one asthma inhaler containing both preventer
and reliever medicine – they do not need to use two separate devices. Your child must be over 12 years old to start SMART therapy.
Does my child need a nebuliser?
A nebuliser is a machine that turns liquid medicines into mist. An asthma puffer with a spacer works just as well as a nebuliser, so there is no need to have a nebuliser at home. Spacers are also portable, cheaper, and much easier to use than
nebulisers.
For more information
Developed by The Royal Children’s Hospital Emergency department, with input from the General Medicine, Respiratory and Complex Care departments. We acknowledge the input of RCH consumers and carers.
Reviewed November 2025
Please always seek the most recent advice from a registered and practising clinician.