Note: This guideline is currently under review.
Introduction
Telemetry is an observation tool that allows continuous ECG, SpO2 monitoring while the patient remains active without the restriction of being attached to a bedside cardiac monitor. The patient group requiring telemetry are children diagnosed with a known/unknown arrhythmia, children at risk of an arrhythmia, or children anticipated to be at risk of sudden cardiac deterioration. Telemetry is not a replacement for patient visualisation and assessment.
Telemetry accuracy relies on skin preparation, electrode and lead placement, equipment maintenance, patient monitoring and education. Studies have shown that with appropriate education to the patient and family, patient safety is improved and anxiety associated with monitoring is reduced. Nurses who are able to identify ECG abnormalities are in prime position to prompt immediate action and lessen patient complications.
Aim
To guide safe and competent nursing and medical practice associated with the use of cardiac telemetry monitoring.
Definition of terms
- Telemetry – A portable device that continuously monitors patient ECG, and/or oxygen saturations while automatically transmitting information to a central monitor.
- ECG – Electrocardiogram is a diagnostic tool that measures and records the electrical activity of the heart via electrodes placed on the skin.
- Electrode – The patch that is placed onto the patient and attaches to the lead wire
- Lead Wire- The lead that connects the electrodes to the telemetry unit
- Arrhythmia – A rhythm in which the heart beats in an irregular or abnormal rhythm
- External Pacing – Temporary means of pacing a patient’s heart. This can occur through transcutaneous pacing or external wires coming from the atrium/ventricle
- Collapse – For the purpose of this guideline – collapse refers to circulatory/hemodynamic collapse
Assessment
Patients should be assessed daily for the appropriateness of cardiac telemetry. Acutely unwell patients at risk of life-threatening arrhythmias should be on strict bed rest and continuously monitored on the bedside monitor and close to emergency equipment. The AUM will be involved in all aspects of care, from patient assessment and daily reviews for appropriateness of telemetry.
Patients aged 2 years and less are not recommended for telemetry. The size of the electrodes are generally too big for patients this age, and this can cause incorrect readings and problems with skin integrity. The algorithm is not strong enough to support infants and neonates (as directed by Philips).
Indications for telemetry include, in consultation with cardiology team, but not limited to;
| Indication for Telemetry |
Duration / Cessation criteria |
| Non-life threatening arrhythmia without haemodynamic compromise |
Monitor until arrhythmia is controlled |
| Post electrophysiology study and catheter ablation |
Monitor as specified by Cardiac Team |
| Stable patients diagnosed with (and not limited to) cardiomyopathy, pericarditis, endocarditis, pericardial effusion or other conditions that may cause arrhythmia |
Continue to monitor throughout treatment, until the risk of arrhythmia has been cleared. |
| Sinus bradycardia without haemodynamic compromise |
Monitor until reversible cause is rectified |
| Pharmacotherapy of pro-arrhythmic drugs causing actual or potential QT prolongation or ventricular dysrhythmias e.g commencement of risperidone |
Duration based on risk stratification |
| Unexplained sudden collapse or other neurological signs/symptoms that might be due to cardiac arrhythmias |
Monitor until cause has been identified, treated and/or the patient is at nil further risk |
For every patient on telemetry – There should be both a daily medical and nursing assessment on the need for continuous cardiac monitoring and this should be documented daily.
Exclusion criteria for telemetry, in consultation with cardiac team;
- Post-operative patients still under post-operative observations
- Patients with any life threatening arrhythmia in the previous 24 hours
- Unwell patients at risk of life threatening arrhythmia (VF, SVT, VT, atrial flutter)
- Patients on inotropic therapy
- Patients being externally paced
- Patients/Families unable/unwilling to follow nursing instructions to stay on the ward
- Frequent unexplained episodes of sudden collapse
Management
- Prior to commencing telemetry monitoring a baseline 12 or 15 lead ECG should be taken as per cardiac team. Additional ECG’s should be performed if ECG changes from patient baseline.
- Nurses looking after patients on telemetry must have completed the following Nursing Competencies: Monitoring (Basic) and Monitoring – Advanced ECG
- A patient on telemetry should be visualised hourly. With every ECG alarm, the patient should be visualised and assessed (refer to Nursing Assessment Clinical Guideline). It is the responsibility of nursing staff to know the where-abouts of their patient at all times
- Children with certain arrhythmias on cardiac telemetry should not lock toilet doors – however laminated signs may be used on doors instead.
- Accurate lead placement and good skin preparation will reduce false readings. Skin that is clean and dry will allow better adherence of electrodes and a more accurate ECG.
- Daily assessment of skin is important in preventing skin excoriation and/or pressure area injury at the site of electrodes.
- Nurses are to provide patient education on telemetry and document in EPIC
Roles and Responsibilities
Specific Monitoring Skills
- Able to “pair” and “un-pair” telemetry device to patient’s bedside monitor
- Recognition of limitations of computer algorithms
- Landmarks for accurate lead placement and importance of accurate lead placement
- Set appropriate heart rate (patient specific), age appropriate profile and ST alarm parameters
- Able to manage a patient with a permanent pacemaker
- Maintain yearly mandatory Basic Life Support Competency
- Understand Defibrillation Algorithm
- Assessed as competent in Defibrillation skills
Identify and intervene in specific paediatric arrhythmias;
- Bradycardia (sinus bradycardia, junctional rhythm, asystole)
- Tachycardia (sinus tachycardia, types of SVT, VT, VF)
- Ectopic Beats (Atrial and Ventricular Ectopic Beats, Premature Atrial or Ventricular Complexes, Unifocal or multifocal)
- Heart Block (1st, 2nd, 3rd degree)
Skin preparation
- Wash skin with soap and water
- Rinse well to remove all of the soap residue
- Wipe skin with alcohol swab if skin is oily, exposed to diaphoresis, (if skin integrity is compromised do not use alcohol)
- Rub skin with gauze to increase capillary blood flow and remove skin cells and oil
Electrode Placement
- Electrodes should be replaced daily to prevent skin break down and to allow optimal conduction. Limb electrodes are placed on the torso to reduce muscle artefacts during limb movement.
Covidien Kendall 130 foam electrodes must be used. The Coviden Kendall 1050NPSM neonatal electrodes are not recommended for telemetry or supported by Philips.
- Telemetry functions with 5 leads (see Figure 1):
White - Right arm (RA) is placed in the infraclavicular fossa close to the right shoulder
Black - Left arm (LA) is placed in the infraclavicular fossa close to the left shoulder
Red - Left Leg (LL) is placed below the rib cage on the left upper quadrant of the abdomen
Green – Right Leg (RL) is placed below the rib cage on the right upper quadrant of the abdomen
Brown- (V1) is placed below the rib cage in between (RL) and the xiphoid process
- If the patient has a permanent pacemaker:
Check that the monitor settings are set to ‘paced’, if it is not picking up the pacing spikes then move the RA electrode down to the 5th intercostal space and the LL electrode is moved up to the 5th intercostal space.
- Misplaced leads may lead to misdiagnosis – eg. If RA is moved by 1 intercostal space then VT may be misdiagnosed as SVT or vice-versa.
Patients diagnosed with dextrocardia will need to have the leads swapped to the opposite side of the body, otherwise the ECG will show inverted P and T waves.
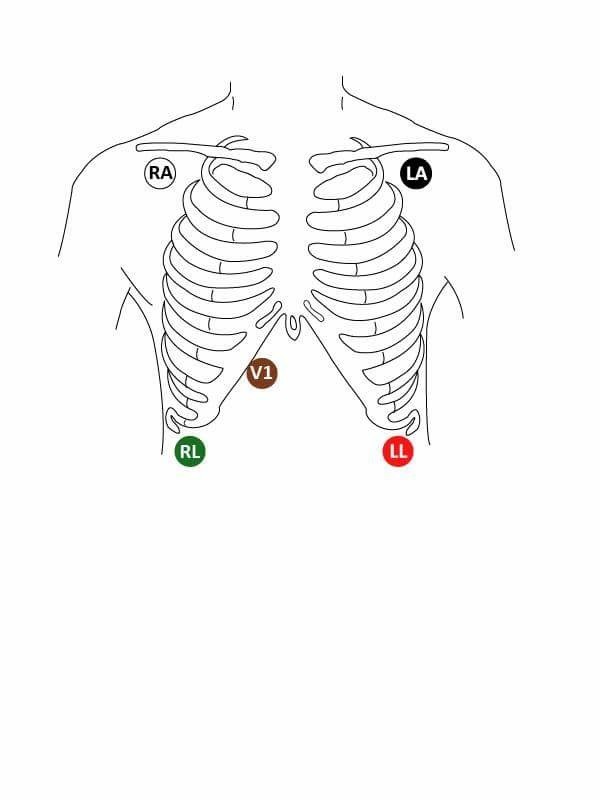
Figure 1 – correct lead placement
Telemetry set up and discontinuation
- The current Telemetry device used at RCH (currently on Koala & Possum wards) is the Philips IntelliVue MX40. For understanding of Device Controls for the MX40 see the manual.
- Ensure patient is admitted onto central and bedside monitoring.
- Insert battery into the telemetry device.
- Add telemetry as equipment on central monitoring and ensure it is displayed on the bedside monitor. Patient’s name will show on the top of the telemetry screen.
- Attach leads and SpO2 sensor (if applicable) to patient ensuring good skin prep prior and fresh ECG electrodes.
- Adjust ECG settings as required.
- When monitoring is ceased, remove the leads from the patient.
- Remove battery and wipe prior to returning it back to charging port.
- Wipe cables and telemetry device before returning it to storage.
- Remove telemetry equipment from central monitoring.
Maintenance
- Check battery status on telemetry device each shift. The device will alarm when batteries need changing
- Electrodes should be changed on a daily basis
- The need for telemetry should be reviewed on a daily basis, this is the joint responsibility of the treating team, bedside nurse and AUM
Patient care
- Telemetry monitoring occurs on Koala ward up to the green lifts.
- All health professionals involved in the patient’s care will know how far the patient is allowed to mobilise while on telemetry. The patient is required to remain within the boundaries of the hospital telemetry signal. If the patient requires a procedure or treatment outside the telemetry boundary, the patient will require a suitable portable cardiac monitoring device such as Philips Intellivue MP2 or Philips Intellivue X2
- The patient will be supervised by parent or nurse at all times when mobilising, this is to ensure patient safety
- The primary nurse will be aware of patient’s location at all times.
- SpO2 sensors should be checked and replaced every 4 hours
- The ANUM should be consulted if patients with a history of deterioration secondary to an arrhythmia needs to cease telemetry monitoring for personal hygiene. In this case the patient should be supervised at all times, and the medical team made aware.
Special Considerations
- If the patient suddenly becomes unstable while on telemetry the patient must be placed on continuous bedside monitoring and thoroughly assessed +/- rapid review or MET.
- If severe skin irritation occurs remove the electrodes and inform the cardiac team. It is rare that anaphylaxis will result, but perform skin, respiratory, circulatory and disability assessment regularly to ensure patient is stable. If anaphylaxis occurs employ anaphylaxis guidelines.
Links
References
Ericksen, A. (2011). Telemetry Travels. Healthcare Traveler, 18(10), pg 35-38
Estrada et al. (2000). Evaluation of Guidelines for the Use of Telemetry in the Non–Intensive-Care Setting. J med intern med. 15(1), pg 51-55
Dresslor .R, Dryer .M, Colletti .C, Mahoney .D, Doorey, A. (2014). Altering Overuse of Cardiac Telemetry in non-intensive care unit settings by hardwiring the use of American Heart Association Guidelines. JAMA intern med, 174(11), pg 1852-1854
Ivonye. C, Ohuabunwo. C, Henriques-Forsythe. M, Uma. J, Kamuguisha .L, Olejeme .K, Onwuanyi .A (2010). Evaluation of telemetry utilization, policy, and outcomes in an inner-city academic medical center. Journal of the national medical association, 102(7), pg 598- 605
Lee. J, Lamb. P, Rand. E, Ryan. C, Rubal. Optimising Telemetry Utilisation in an Academic Medical Center. B Original Research, 2008, 15(9), pg 435 – 439
No author (2008). Dysrhythmia Monitoring. American Association of Critical Care Nurses, 28(5), pg 90-91
Philips Healthcare (2020). IntelliVue MX40. YouTube video. https://www.youtube.com/watch?v=wpFvfzqsLRY
Philips Medical Systems (2012). IntelliVue MX40 manual. http://incenter.medical.philips.com/doclib/enc/fetch/2000/4504/577242/577243/577247/582636/582882/MX40_B.0_Service_Guide.pdf%3Fnodeid%3D10668578%26ver
Evidence Table
View this guidelines evidence table here.
Please remember to read the
disclaimer.
The development of this nursing guideline was coordinated by Annabelle Santos, CSN Nursing Education and Emily Mohd-Faizal, RN Koala, and approved by the Nursing Clinical Effectiveness Committee. Updated November 2021.