Nosebleeds are very common in children. A nosebleed (also called epistaxis) occurs when a small blood vessel in the lining of the nose bursts. The inside of the nose is delicate and the small blood vessels are fragile and close to the surface. This means they can burst easily, and start
bleeding.
The bleeding is usually minimal and brief, and will typically stop in less than 10 minutes. While it can look like a lot of blood has been lost (especially when soaked in a tissue or on clothing), it is rare for children to lose so much blood that it causes any problems (e.g. anaemia). This
is only to be likely with frequent, heavy nosebleeds over several weeks or months.
Nosebleeds can usually be treated with first aid, and a visit to the doctor is not needed.
What causes nosebleeds?
Nosebleeds often caused by harmless activities such as your child picking their nose, blowing it too hard or too often, or from getting knocked on the nose during play.
Other causes of a nosebleed may include:
- overly sensitive blood vessels that burst and bleed in warm, dry weather
- infections in the nose, throat and sinuses (e.g. common cold)
- allergies (e.g. dust mite allergy or hay fever)
- a foreign body in the nose (e.g. when a child has pushed something up their nose)
- constipation (e.g. excessive straining when going to the toilet)
- certain medications (e.g. anti-inflammatory medicines or nose sprays)
- an underlying medical problem, but this is very uncommon.
Sometimes, children can have multiple nosebleeds over a several weeks.
First aid for nosebleeds
Nosebleeds do not cause pain; however, your child may be very distressed and upset by the sight and taste of blood during a nosebleed.
Try to calm and reassure your child, because crying will make the bleeding worse, then follow these first aid instructions:
- Sit your child upright in a comfortable position, and lean slightly forward.
- Squeeze the lower, soft part of the nose, pressing the nostrils together with your fingers (your child can do this if they are older). Keep squeezing for 10 minutes.
- Do not keep removing your fingers to check if the bleeding has stopped. The blood needs to clot and this takes time. Reading a book can be a good distraction for your child. Have a clock handy so you can be sure 10 minutes has gone by.
- After 10 minutes, release the nose and check if the bleeding has stopped. If the nosebleed continues, squeeze the nostrils for another 10 minutes.
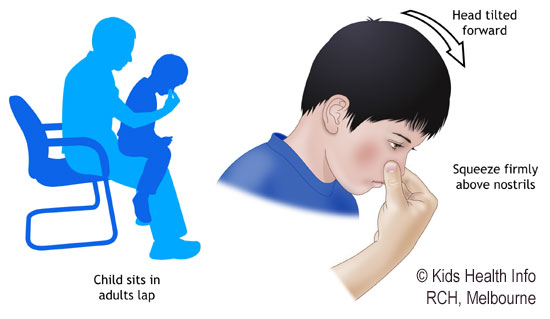
In addition to squeezing the nostrils, try the following:
- If your child can tolerate it, place a cool towel or covered icepack on the back of their neck while they sit on your lap.
- Offer your child an icy pole or cold drink to cool them down and get rid of the taste of blood.
- Encourage your child to spit out any blood that has dripped from their nose into their mouth. Swallowing blood may make your child vomit, which can cause the nosebleed to continue or worsen.
When to see a doctor
If after trying first aid the bleeding continues, take your child to the GP or your nearest hospital emergency department. A doctor will look up into your child's nose with a light to see if they can find the bleeding blood vessel.
The doctor may then:
- Apply a cream or ointment that contains a special medicine to slow the blood flow to the inside of your child's nose.
- Use cautery, which is a special chemical that freezes or burns the blood vessel to stop the bleeding (a process referred to as cauterisation).
- Pack your child's nose with a dressing. The doctor may also prescribe antibiotics to prevent a bacterial infection while the packing is in the nose. Occasionally, children who need nasal packing may be admitted to hospital overnight.
If nasal packing is not needed, your doctor may prescribe an antibiotic ointment to be applied to the inside of your child's nose up to four times a day for a week or so to clear any mild infection that may be present.
For severe nosebleeds, your child may need to have a blood test to check how much blood they have lost.
Take your child to the GP if they:
- have nosebleeds frequently over a period of several weeks
- have nosebleeds and bruised skin anywhere on the body, pale skin or a family history of bleeding disorders.
Your child may be referred to an ENT (ear, nose and throat) specialist.
Care at home
After a nosebleed:
- Rest your child for the next couple of hours if the nosebleed was not severe (you were able to stop it yourself using first aid). Rest for 12–24 hours if it was a severe nosebleed that needed medical assistance. Quiet activities such as drawing or reading a book are
recommended.
- Avoid giving your child hot drinks or food, or hot baths or showers for at least 24 hours.
- Tell your child not pick or blow their nose for 24 hours (and for a week if they have had their nose cauterised).
- If your child's nose has been packed, the gauze will need to remain in place for 24–48 hours. You will need to take your child to the GP for a check-up and to have the gauze removed. Do not try to remove the packing yourself. If it falls out on its own and the bleeding doesn't return, there is
no need to go back to the emergency department or GP.
To help prevent nosebleeds in the future:
- If your child's nose is dry and cracked, apply a petroleum-based gel or ointment (e.g. Vaseline) to the nostrils, generally twice each day for a week. This can be done by using a cotton tip or finger, and gently rubbing it on the inside of the nose. Do not use this method in
children under four years of age as they are unlikely to cooperate or sit still, and their nose may be injured.
- If your child is suffering from constipation, increase their fluid intake and the amount of fibre in their diet, or ask your doctor or pharmacist for a stool softener to prevent them from straining. See our fact sheet
Constipation.
Key points to remember
- Nosebleeds are very common in children and often caused by harmless activities.
- Most nosebleeds cause only minor discomfort to your child.
- First aid is used to treat nosebleeds.
- For severe nosebleeds, a doctor may use an ointment, cauterisation or nasal packing to stop the bleeding.
For more information
Common questions our doctors are asked
After a nosebleed, it's very
difficult to get my child to not sniff or pick at his nose for a whole day.
What can I do?
Having a nose full of clotted blood is not
pleasant, and it is understandable that children may find it difficult to avoid
sniffing, blowing or picking at their nose. Try to distract your child for as
long as possible to give the blood clot time to stabilise – even 15 minutes
without your child sniffing, blowing or picking will help.
Developed by The Royal Children's Hospital Emergency department. We acknowledge the input of RCH consumers and carers.
Reviewed March 2018.
This information is awaiting routine review. Please always seek the most recent advice from a registered and practising clinician.
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit
www.rchfoundation.org.au.