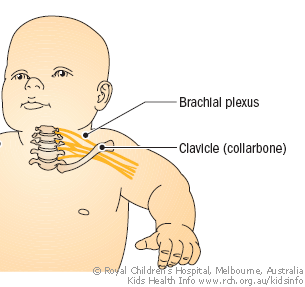
The brachial (brake-ee-al) plexus is a large network of nerves running from the neck to the arm. These nerves provide movement and feeling to the arm and hand. Brachial plexus palsy is weakness or paralysis in parts of the arm as a result of significant injury to the brachial
plexus, which can happen during childbirth. The most common type of brachial plexus palsy is called Erb's palsy.
Brachial plexus palsy may be caused during childbirth. Sometimes after the baby's head has been delivered, the shoulders sometimes get trapped inside the mother's pelvis. To free the shoulders, the head is tilted to the opposite side and this stretches the brachial plexus nerves. Brachial
plexus palsy can also be due to the baby's position inside the uterus, and in rare cases may occur during a Caesarean section.
Signs and symptoms of brachial plexus palsy
The nerves that make up the brachial plexus carry electrical signals (instructions) from the brain to the arm, so that the arm and hand can feel and move. If nerves are injured, the muscles of the arm and hand may not receive all of the instructions from the brain. This may result in:
- the affected arm not moving normally
- the muscles in the arms starting to waste (get smaller)
- limited feeling (e.g. of temperature or pain) in the affected arm.
Your baby may also have other problems as a result of the injury, including:
- a broken collar bone (clavicle)
- a broken upper arm bone (humerus)
- Horner's syndrome (the eyelid droops and the pupil of the eye is slightly smaller on the same side as the weak arm).
When to see a doctor
In most cases, brachial plexus palsy will be noticed during routine checks in hospital after your baby is born. Your Maternal and Child Health Nurse may also pick it up. If you notice any of the signs of brachial plexus palsy, take your baby to the GP or paediatrician. They may involve a
specialised plastic surgeon and/or physiotherapist.
There is no single test to tell how serious the brachial plexus injury is. Your baby's doctors and physiotherapist will assess your baby's arm over a period of time. They will look for improvements in movement, function, shape and size.
Treatment for brachial plexus palsy
Your child may be seen by a team including a plastic surgeon, orthopaedic surgeon, physiotherapist and occupational therapist. Once an assessment has been completed, a treatment and follow up plan will be provided to you which may include regular reviews, stretches, positioning,
splinting and referral to local services if required.
Most babies with brachial plexus injuries recover fully with minimal treatment. However, in rare cases, some children may require surgery for the nerves, muscles and bones.
Care at home
If you have be prescribed exercises or splints by your therapists, you will be shown how to complete these and incorporate these into your baby’s daily routines (e.g. during bath time and dressing).
It is important to take extra care not to injure the affected arm. Because the feeling is reduced, your baby may not feel hot objects (i.e. burning) or pain. Therefore, they may not show distress and it can be difficult to tell if they are injured.
Key points to remember
- Brachial plexus injuries can occur at birth, and cause weakness or paralysis in the affected arm.
- Most babies with brachial plexus injuries recover with physical therapy alone.
- If your physiotherapist has prescribed stretches and exercises, it is important to continue these at home for the best possible outcome.
- About one in 10 children needs surgery to help improve function of the arm.
- It is important to take extra care not to injure the affected arm as your baby may not feel pain normally in that arm.
For more information
Common questions our doctors are asked
Will my child's arm always be weaker than the other arm or will it improve as my child grows older?
In most cases, a full recovery occurs within the first one to three months, but up to one quarter of babies will have ongoing function problems of the affected arm. With physical therapy, most children make a full recovery or are left with minimal impairment.
How likely is surgery to be successful?
Surgery is uncommon and is usually only used in children who do not recover (with full arm function) in the first three to nine months of age. Surgery is aimed at improving function but will not result in a perfect outcome.
Developed by The Royal Children's Hospital Plastic and Maxillofacial Surergy, Physiotherapy and Occupational Therapy departments. We acknowledge the input of RCH consumers and carers.
Reviewed
August 2018.
This information is awaiting routine review. Please always seek the most recent advice from a registered and practising clinician.
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit
www.rchfoundation.org.au.