A lumbar puncture is a test where a doctor uses a needle to get fluid from your child's lower back. This fluid is called cerebrospinal fluid, or CSF. Your child lies on their side and is held still, and a doctor puts a needle between the bones of the lower back. It does not go near the
spinal cord. Lumbar punctures are also sometimes called a spinal tap or LP.
Why does my child need a lumbar puncture?
A lumbar puncture is needed to test the fluid around the brain and spinal cord. This test may be done to find out if a child has meningitis (a serious infection around the brain). Meningitis may be suspected in a baby with a fever, especially in babies less than one month old.
Early diagnosis of meningitis can greatly improve your child's chances of a full recovery. If your child has meningitis, they will need other tests and treatment in hospital.
Lumbar punctures are also done for other reasons, but your child's doctor will discuss these with you before performing an LP.
What to expect
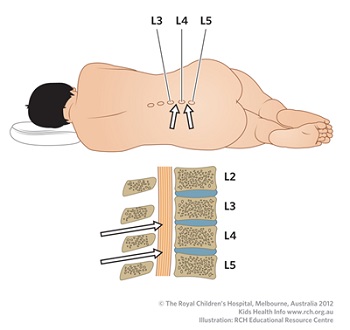
During a lumbar puncture, your child will lie on their side with their knees tucked into their chest and head bent forward. Babies will be curled in a ball to get a better position. Young children and babies will be held in position by an assistant. A doctor then puts a needle into the spaces between the spine
bones (see white arrows in the figure below) to the area where the fluid is. This area is called the subarachnoid space.
A lumbar puncture is an uncomfortable test, and sometimes painful. In addition, babies and small children do not like being held in place and will often cry. Your child may be given some cream or an injection to help numb the area where the needle will go in, and some children can be given
medicine to make them feel calmer and less scared.
What are the risks?
A lumbar puncture is a safe test. Sometimes doctors are not able to get fluid, and they may have to try more than once. A small number of children may have a headache or backache for a day or two after the test. The risk of any serious complications, including bleeding, infection or damage to
nerves, is extremely low.
Care at home
After the procedure, your child can be bathed normally. If there is a dressing or sticking plaster (e.g. BandAid) on your child's back, it can be taken off the next day or left to fall off by itself if your child prefers.
If your child has a headache or sore back, you can give them some paracetamol (see our fact sheet
Pain relief for children).
Key points to remember
- In a lumbar puncture, a doctor uses a needle to take fluid from your child's lower back.
- It is the only way to be sure if your child has meningitis or not, and is also used for other tests.
- A lumbar puncture is a safe test. The needle does not go near the spinal cord.
For more information
Common questions our doctors are asked
What can I do to help keep my
child calm during the procedure?
Encourage them to focus on their breathing or
distract your child by talking about something that makes them happy. You can
be close to your child during the lumbar puncture – let them know you are there
with them and you are impressed by how well they are doing. If they ask before
the procedure if it is going to hurt, it is best to be honest. Say something like,
'It might feel a bit uncomfortable – some children find it a bit painful but
some children think it's not so bad.' If your child is very anxious, medical
staff can give them some medicine to help calm them. Young babies may be given
sucrose solution (a solution of sugar and sterile water), which can have a
calming and pain-relieving effect on babies.
How long will it take?
Once your child is in the correct position and
the area is properly cleaned and prepared, the lumbar puncture should only take
a minute or two. The better your child's position and the more calm they
remain, the more likely the lumbar puncture is to be successful on the first
attempt.
Developed by The Royal Children's Hospital General Medicine and Emergency Medicine departments. We acknowledge the input of RCH consumers and carers.
Reviewed May 2018.
This information is awaiting routine review. Please always seek the most recent advice from a registered and practising clinician.
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit
www.rchfoundation.org.au.