There can be changes to a person's eyesight after a brain injury has occurred. This can include
problems with the field of vision, the position of the eye and
how the eye moves. There are different treatments and strategies to
help reduce or adapt to vision related difficulties.
What can
happen to eyesight after brain injury?
The visual system is large
and complex. The picture travels from the eyeball to the
occipital cortex at the back of the brain (see Figure 1).
Information is received by the eyeball and then transferred in
special nerves to the back of the brain where it is decoded into what we
'see'. The occipital lobe is the area of the brain
where information processed by the eyes is decoded and information
about what we see (colour, shape and distance) is
understood.
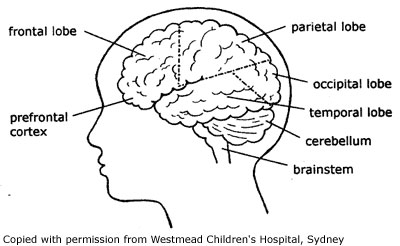
Figure 1
Injury to any part of this
pathway can lead to problems with eyes and vision (see Figure 2).
Problems with eye positions (squint or strabismus, double vision),
eye movements (jerky eyes, nystagmus, poor tracking), visual field
defects and vision problems are common after a brain injury. Over
time these visual difficulties tend to improve.
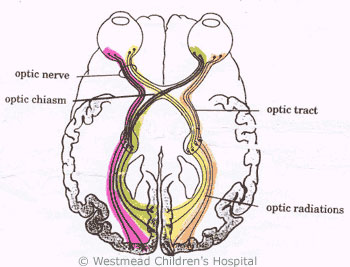
Figure 2: Visual pathwaysSymptoms
Double vision
Double vision (diplopia) is
caused by an imbalance of the eye muscle movements. The two images,
one from each eye, are not aligned properly and so the child sees
this as a double image. A child may close or cover one eye to look at something or have difficulty with balance or judging
depth. They may have difficulty reading and copying. The child may
have a squint or turn of one of their eyes.
Visual field
defect
Visual field defect
(hemianopia) is due to an interruption of the visual pathways in the
brain. The result is a loss of vision in one half of the
visual field in each eye (see Figure 3). A child may not pay
attention to one side, may bump into objects on one side of the
body or only draw on one side of a page.
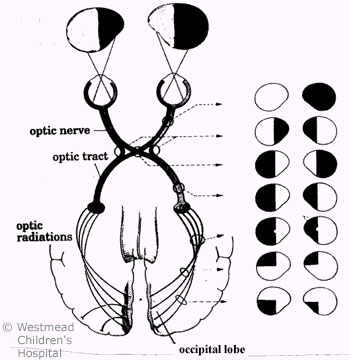
Figure 3: Visual
field defects - depend on the area of the visual pathway
damagedPoor visual acuity
Poor visual acuity is when
you cannot see clearly. This is tested by using eye charts with
letters or pictures. Special tests are available to test those
children who cannot name pictures or read letters.
Squint
Squint (strabismus) is when
the eyes are not in line with each other. Children may tilt or
turn their head to try and line the eyes up because the eyes
cannot correct the position themselves.
Treatment
Eyeball
problems
If the problem with vision
is because of an eyeball problem, glasses can sometimes
help. However, glasses are not usually helpful after a brain
injury. Ways to compensate for the problem are needed while
the child's eyes and vision recover.
Double vision
Patching one eye can
relieve double vision. It is important to swap eyes with the
patch so that one eye does not become weak from lack of use.
Patching can also help strengthen the muscles that cause a squint.
To help a squint, the eye with better vision is patched making the
weaker eye work and straighten its position.
Poor visual
acuity
There are a number of things that can be done to help a child with poor visual acuity:
- reduce the amount of information presented
on a worksheet
- enlarge pictures and writing
- have well contrasted pictures (i.e. strong
black and white) in books
- use felt tipped pens for drawing and
writing
- make sure the child has good lighting and
good seating for school and homework
- use a slope board on desks if the child has
difficulty looking down
If a child has a very
severe vision impairment, Vision Australia should be
involved. They provide a comprehensive service for home and school
to help children with vision difficulties.
Visual field
defects
Teaching children to look
or scan left and right will help them be aware of people or objects
in their 'blind spot'.
When to see a doctor?
Your GP,
paediatrician or neurologist can assess your child's eyes and vision, and they
may refer your child to see an ophthalmologist and an orthoptist.
An ophthalmologist is a
doctor who specialises in disorders of the eye. An orthoptist is a person
who specialises in assessment of eyes and vision. Most children who have
difficulties with eyes and vision after a brain injury see both an
ophthalmologist and an orthoptist.
Key points to
remember
- Problems with eye movements and positions,
visual field defects and vision problems are common after a brain
injury.
- Over time, the visual difficulties tend to
improve.
- A GP, paediatrician or neurologist
can assess your child's eyes and vision, and can refer your child to see an
ophthalmologist and/or an orthoptist.
For more
information
Developed by The Royal Children's Hospital Paediatric
Rehabilitation Service. We acknowledge the input of RCH consumers and carers.
Reviewed August 2020.
Kids
Health Info is supported by The Royal Children’s Hospital Foundation. To
donate, visit www.rchfoundation.org.au.