Bedwetting is a problem for many school-age children and their families. The good news is that for many children the problem will resolve itself over time, or can be fixed through fairly simple treatment.
Bedwetting (also called nocturnal enuresis) is very common. As the following graph shows, almost a third of four-year-olds wet the bed. By the time they are six, only one in 10 children wet the bed, and one in 20 by age 10. Bedwetting can sometimes continue
into adolescence.
Percentage of children who wet the bed at different ages
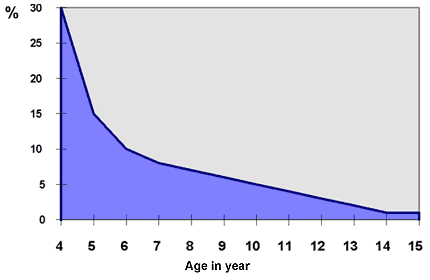
Most children have no lasting problems from bedwetting; however, many will feel embarrassed or ashamed. It is important to reassure your child that they are not the only one who wets their bed. For younger children, there will most likely be many other
bedwetters in the same class at school.
It is common for children to become dry at night for a while and then to start wetting their bed again.
What causes bedwetting?
While not all causes of bedwetting are known, some of the possible factors are:
- genetic tendency (bedwetting tends to run in families; if one or both parents wet the bed when they were children, then it is quite likely their children will be bedwetters)
- a smallish bladder capacity
- the child is a deep sleeper
- the child’s kidneys continue to produce a lot of urine at night (usually, people make less urine when they are asleep)
- constipation (if constipation is causing your child to wet the bed, treating the constipation will help your child to stay dry at night. See our fact sheet
Constipation)
In some rare cases, there may be a medical problem that is the cause of the child's bedwetting.
Bedwetting is not often a behavioural problem and children rarely do it for attention. It is far more likely that they have little control or awareness when they are having accidents overnight.
When to see a doctor
You may wish to see a doctor about your child's bedwetting if:
- your child is at least seven years old (treatment for bedwetting is not recommended before this age as treatment is less effective and many children get better on their own)
- you or your child are troubled or frustrated by the bedwetting
- you punish, or are concerned that you might punish, your child for wetting the bed
- your child wets or has bowel movements in their pants during the daytime
If your child has been dry at night for six months then begins to wet their bed again, it is important to see a doctor for evaluation.
The doctor will consider your child’s details and determine if there is a physical problem that needs to be addressed.
Treatment for bedwetting
Motivation
Most children don't need rewards to motivate them to take part in treatment – the prospect of a regular dry bed is usually enough.
It can be helpful to keep a record chart of wet and dry nights. Your child should make the chart themselves and choose how to complete it. Some children like to put stars or stickers on for dry nights, or to colour it in or draw pictures. Choose something
that fits in with your child's interests, for example, football stickers. Charts used on their own usually have little success, but in combination with other treatments they can be very useful.
Drinking fluids
It is important for your child to drink plenty of fluids spread evenly throughout the day. Don't try to restrict the amount of fluid your child drinks in the evening, as this will not help and can even delay the process of being dry at night. However,
don't give drinks containing caffeine (coffee, tea, hot chocolate, caffeinated soft-drinks like cola etc.) late at night.
Bedwetting alarms
Bedwetting alarms are thought to be the most useful and successful first-step to treat bedwetting. Research has shown these alarms will help 80 per cent of children to become dry, and most children will then stay dry. Children using alarms are less likely
to relapse compared to children taking medication.
A child using a bedwetting alarm needs a supportive and helpful family as it may take six to eight weeks to work.
There are 2 types of bedwetting alarms - Bell and Pad Alarm and Personal (body-worn) alarm. The bell and pad alarm can be hired through RCH Enuresis clinic.
Bell and Pad Alarm Video
Personal Alarm Video
Bell and pad alarm instructions
Bedwetting alarms are available for hire or can be purchased. A rubber mat is placed in the bed under where the child's bottom will be, and is connected by a wire to a box with a battery-powered alarm bell. Others have a smaller sensor that attaches to
a child's underwear. These systems operate at low voltage and there is no risk to your child.
- If using a mat, it should be placed on the bed on top of the bottom sheet and should be covered with a piece of thin material (e.g. an old sheet that has been cut up) just big enough to cover the mat and long enough to tuck in on either side of the
bed.
- The wires should be plugged into the box, which should then be placed as far away from the bed as the wire will allow.
- When going to bed, your child should switch on the alarm and get into bed. It is best if they only wear a pyjama top and underpants, rather than pyjama trousers or a long nightdress.
- When your child wets the bed, a loud alarm will sound. Your child should get out of bed as quickly as possible, turn off the alarm and go to the toilet to finish emptying their bladder. Then your child should dry the mat using the piece of material,
put a new piece of material over the mat, turn the alarm back on and get back into bed. You may have to help your child with some of this, at least for the first few nights and especially if they are a very deep sleeper.
- Practise the whole routine a few times with your child. You can use a glass of salty water, instead of urine, to set the alarm off. Remind your child what the routine is as your child gets ready for bed for the first few nights.
- If your child is a deep sleeper, you may have to wake them up for the first few nights when the alarm sounds. Most deep sleepers will get used to waking to the sound of the alarm. Your job is only to wake your child – they must do the rest themselves.
- Within a week or two your child should start to have some dry nights. This may happen because they wake up and go to the toilet before wetting the bed, or because they learn to hold on all night.
- If your child has seven dry nights in a row, try giving some extra fluid to drink in the evening. This is called ‘overlearning’.
- If your child has 14 dry nights in a row, try leaving the mat on the bed but without the alarm switched on and see what happens. If dry nights continue, try leaving the mat off the bed all together.
Medications
Most children with bedwetting do not need to take medication, but there are some occasions when it can be useful. Your doctor can advise you if this treatment is suitable for your child.
DDAVP (also called Minirin) is a medicine that helps a child's body make less urine at night. It will reduce the likelihood of your child's bladder overfilling during sleep.
DDAVP is usually reserved for children who have not become dry after using a bedwetting alarm – sometimes the two treatments are then given together. Some children use the medication for sleepovers or school camps.
It is safe to uses DDAVP, provided you never exceed the recommended dose, and you avoid excessive fluid intake in the evening after dinner. Be careful to follow the instructions provided with the medication.
DDAVP can work quickly. Some children will be dry after the first night. Many doctors recommend using DDAVP for three months, followed by a tapering off period to determine if your child can stay dry without medication. Some children will resume bedwetting
when the drug is withdrawn. If your child becomes wet again, your doctor may ask you to restart DDAVP and try to stop it again every few months to see whether your child still needs it to stay dry.
General tips
Regardless of which treatment you will be using with your child, there are some general strategies that are useful throughout the treatment process.
- It is very important to be patient and to encourage your child. Punishing or making fun of your child for wetting the bed will only make the situation worse – make sure siblings understand this as well.
- Your child needs to be very involved in the treatment plan if it is to work. Be very positive on the good nights, and try not to be negative on the bad ones.
- If you are putting your child in a nappy or pull-up at night to save on laundry, it is unlikely that they will become dry while this continues. Nappies or pull-ups cannot be worn while using a bedwetting alarm.
- You might like to use some form of protection for the bed while waiting for your child to stop wetting. A variety of pads and covers are available to protect the bed and pillow, and there are underwear pads that can be used for certain occasions (e.g.
school camps, holidays, sleepovers).
Key points to remember
- Bedwetting is very common
- Most children have no lasting problems from bedwetting
- Family members of children who wet the bed need to be supportive and not critical
- Bedwetting alarms are considered the most successful first step to treat bedwetting. Medication is an option if alarms have not helped
For more information
Why does my child still wet the bed?
Common questions our doctors are asked
When will my child grow out of bedwetting?
All children develop at different rates, and some children may wet their bed occasionally until the age of seven or eight. If this is happening regularly, see your GP. If your child is over six years old and bedwetting is causing problems for
them (or for you), take them to the GP, especially if they were previously dry overnight.
My child has school camp coming up. How can I stop him bedwetting at camp?
You could start using a bedwetting alarm for two months before camp to help your child stop bedwetting – it may take six to eight weeks to work for your child. If that doesn’t work, your GP may be able to prescribe DDAVP for your child to use
on school camp. If you don’t wish to use medication, you may like to try underwear pads for camp.
Developed by The Royal Children's Hospital General Medicine department. We acknowledge the input of RCH consumers and carers.
Reviewed July 2020.
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit
www.rchfoundation.org.au.