See also
Burns: Post acute care and dressings
Trauma: the primary survey
Key points
- Burn injuries should be managed as a trauma case with prioritisation of appropriate burns first aid
- Accurate total body surface area (TBSA) estimation is essential for fluid resuscitation decision making. TBSA does not include epidermal burns
- Provide early and adequate analgesia to facilitate assessment and ensure patient comfort
- Appropriately consented photographs of the burn are helpful for assessment and monitoring
Background
Specific features in children with burns
- Children have thinner skin than adults, predisposing them to a deeper burn for any given temperature
- Assessment of burn depth is difficult, especially early post injury
- Young children are at risk of hypothermia, especially during initial cooling of the burn
Burns are described as epidermal, dermal (superficial/mid/deep) and full thickness
Early first aid with a total of 20 minutes of cool running water provides pain relief, decreased cell damage, improved wound healing and decreased scar formation, when delivered within 3 hours of the burn.
Assessment and initial management
Like all traumas, paediatric burn assessments require a primary and secondary survey with the initial aim of identifying and managing immediate life threats. Do not get distracted by the burn injury
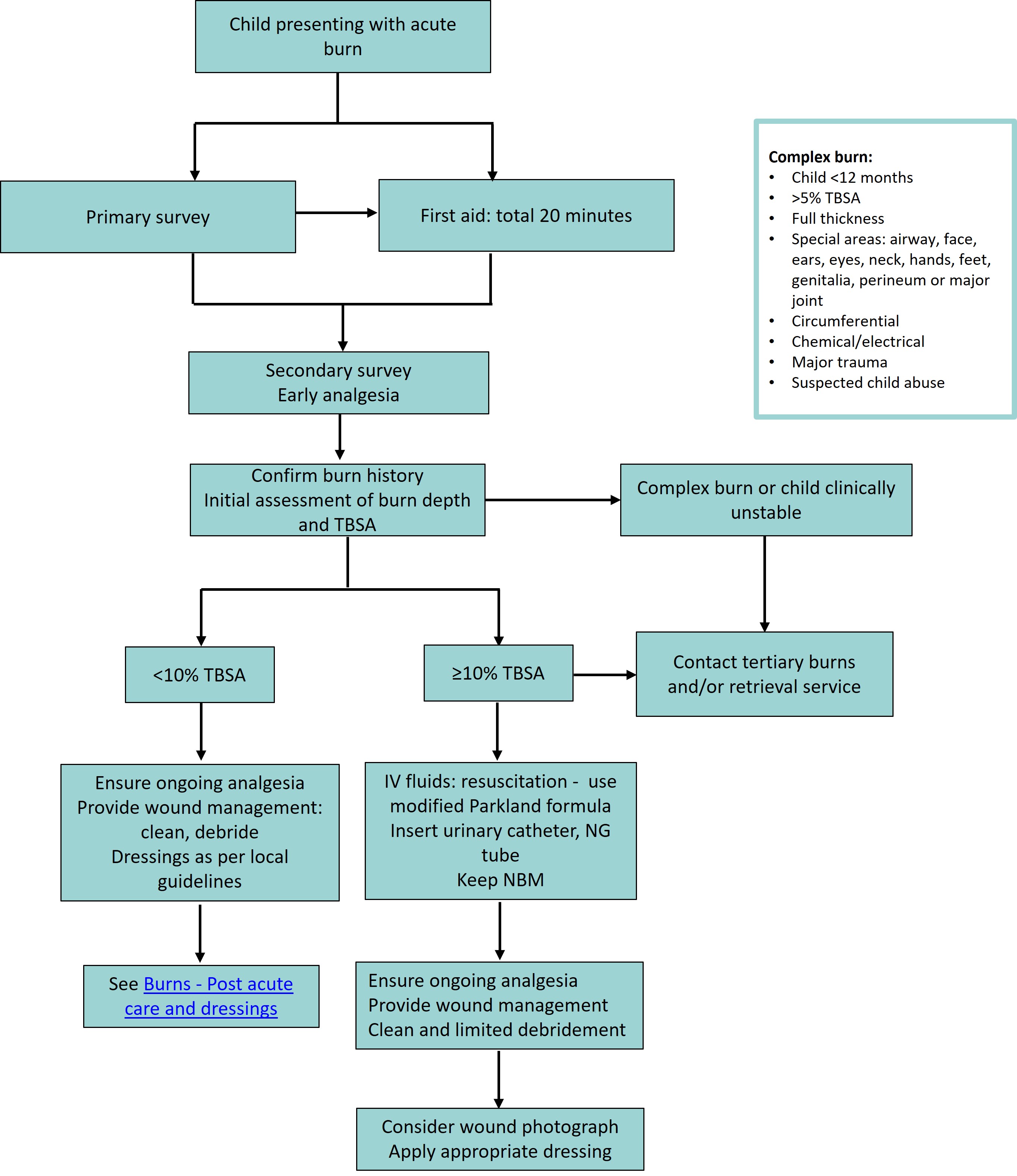
Primary survey
See Trauma: primary survey
Airway
- Signs of airway burn/inhalation injury: stridor, hoarseness, black sputum, respiratory distress, singed nasal hairs or facial swelling
- Sign of oropharyngeal burn: soot in mouth, intraoral oedema and erythema
- Significant neck burn: circumferential, or oedema leading to airway compromise
- If above present, consider early intubation
- If suspicion of airway burns or carbon monoxide intoxication apply high flow oxygen
- Protect the cervical spine with C-spine precautions if there is associated trauma
Breathing
- Assess adequacy of breathing and chest wall expansion
- If abnormal with chest wall or abdominal wall full thickness and/or circumferential burns, consider escharotomy - this will require referral to tertiary burns service
Circulation
- If early shock is present, consider causes other than the burn
- Ideally obtain 2 points of IV/intraosseous access
- Give IV fluid bolus in setting of haemodynamic instability
- Give IV fluid if >10% TBSA using modified parkland formula for rate calculation
- For circumferential burns check peripheral perfusion, elevate limb and need for escharotomy
Disability
- Assess with AVPU (or paediatric GCS), check pupil reaction
- If altered conscious state, consider airway support
- Assess neurovascular status if limb involved
First aid
- Remove clothing, nappy, and jewellery in contact with burn source and distal to the burn
- Cool affected area as soon as possible (within 3 hours from time of burn) for total of 20 minutes with cool running water
- If unable, consider: frequently changed cold water compresses, immersion in a basin, or irrigation via an open giving set
- Never apply ice and avoid use of hydrogel burn products
- Cooling can be paused to prevent hypothermia and for significant distress, continue when clinically appropriate
- Consider cooling smaller areas sequentially to reduce hypothermia
- Cover burn with plastic cling film lengthways along the burn
- Do not wrap circumferentially
- Do not apply plastic cling film to face or chemical burn
- Use paraffin ointment on facial burns
- Consider topical antibiotics such as chloramphenicol
- Discuss chemical burn decontamination with Poisons Information, phone 131126
- Appropriately consented photos of burns prior to dressings are useful for ongoing management. Parents can also keep photo diary on own phone
- Prevent hypothermia
- Remove wet clothes/dressings after initial cooling
- Try to keep child otherwise warm
- Cover the wound and the child after assessment
- When possible warm the environment or use warming devices
- Consider warm intravenous fluids
Exposure
History of burn
- Time of injury
- Mechanism of injury, including circumstance for specific pattern of burn
- Scald: estimated temperature and viscosity of the liquid
- Contact: estimated temperature and nature of the surface
- Friction
- Flame/explosion: product that burned/exploded, any known accelerant, location (enclosed vs. open space), duration of exposure, any inhalation injury
- Electrical: voltage, type of current (AC or DC), duration of contact
- Chemical: type of product
- Cold: direct contact with cold surface or exposure (frostbite)
- Radiant: sunburn
- Further injury details: location of child when burned, who was present/supervising child
- Any first aid provided prior to presentation
- Time started: was it within 3 hours and maintained
- Agents used
- If clothes and jewellery were removed
- Decontamination method (for chemical exposure)
- Consider co-existing non-burn injuries
- Consider child abuse
- Look for pattern of burn and/or inconsistent history eg immersion scald burns, patterned burn by hot object, mechanism not in keeping with pattern of burn, location of burn, eg back or genitalia
- Tetanus immunisation status
Analgesia
- Ensure adequate pain relief on presentation and ongoing analgesia, especially during dressings and mobilisation: see Acute pain management
- Procedural sedation is recommended for debridement and dressings. See Procedural sedation
Assessment of burn depth
- Burns are dynamic wounds, it is difficult to accurately estimate the true depth and extent of the wound in the first 48-72 hours
- Do not include area with epidermal burn (erythema only)
| Classification |
Depth |
Colour |
Blisters |
Capillary refill |
Sensation |
| Superficial |
Epidermal |
Red |
No |
Brisk |
Present |
| Superficial dermal |
Pale pink |
Present |
Brisk |
Painful |
| Mid dermal |
Dark pink |
Present |
Sluggish |
+/- |
| Deep |
Deep dermal |
Blotchy red |
+/- |
Absent |
Absent |
| Full thickness |
White |
No |
Absent |
Absent |
Assessment of TBSA
- Expose whole body, remove clothing and log roll to visualise posterior surfaces
- Use paediatric specific TBSA tool, eg
- NSW Trauma App
- Paediatric Lund & Browder chart, see below
- Palmar surface, see below
Paediatric Lund and Browder chart
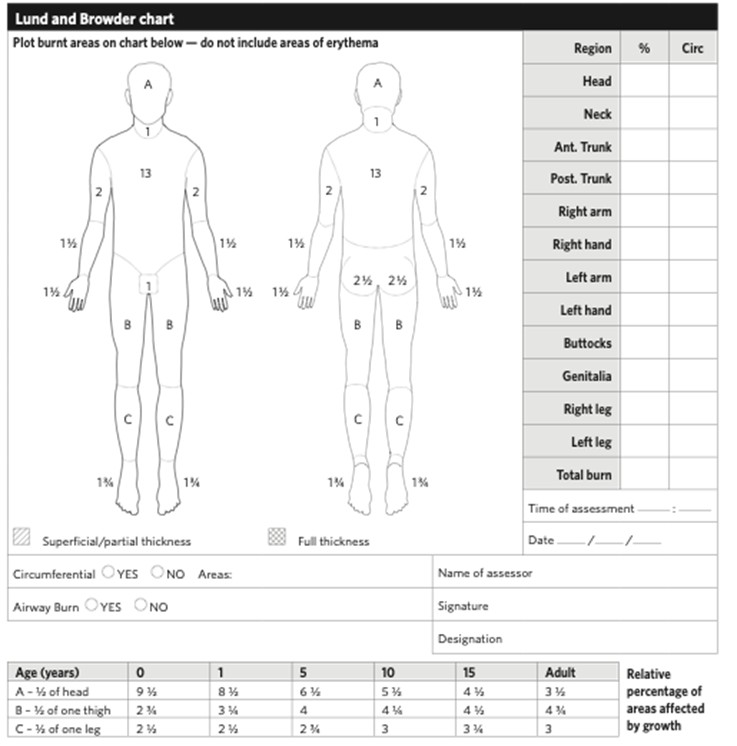
Palmar surface
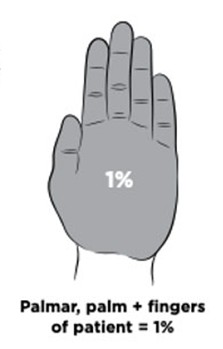
Management
Investigations
Baseline investigations
| Major burn (≥10% TBSA) |
Haemoglobin, electrolytes, BGL, group and hold, VBG |
| Multi trauma |
See Primary and Secondary survey |
| Suspected inhalation injury |
VBG for carbon monoxide or hydrogen cyanide poisoning |
| Electrical burn |
ECG |
Treatment
Acute fluid management in burns ≥10% TBSA
- The goal is optimal replacement of fluid losses to maximise wound and body perfusion, and minimise wound and body oedema and associated adverse effects
- Calculate requirements from time of the burn, not from time of presentation
- Give resuscitation fluids (Hartmann's solution) and, via a separate line, maintenance fluids (sodium chloride 0.9% with glucose 5%)
- Calculate resuscitation fluid volume using Modified Parkland Formula (below)
- Give half the total amount of the first 8 hours then the remainder over the next 16 hours
- Review fluid rate every 1-2 hours and adjust rate according to the urine output and fluid state, total resuscitation fluid volume is estimate and must be individually tailored
- Hartmann's solution is the fluid of choice - if unavailable, use sodium chloride 0.9%
- Insert urinary catheter for strict fluid balance
- Keep nil by mouth and insert nasogastric tube, gastric ileus is a potential complication
- Patients with delayed fluid resuscitation, electrical conduction injury and inhalation injury have higher fluid requirements. Discuss with specialist team

Burn wound management
General burn management
- Debridement
- Wipe wounds to remove clearly loose tissue
- De-roof blisters >5mm or if crossing joint with moist gauze or forceps and scissors. See blister management
- Clean burn wound and surrounding surface with water, saline, QV wash, and/or Prontosan®
- Reassess burn, take photos with appropriate consent
- Refer to state guidelines for dressings selection
- If listed products are not available, contact local Burns service for advice
Burns dressings
See Burns: post acute care and dressing
Specific Burn Management
| Type of burn |
Consideration |
| Circumferential deep burn (deep dermal or full thickness) |
Ensure jewellery removed
Neurovascular compromise
Elevate part of limb distal to burn
Monitor colour, capillary refill time, temperature
Escharotomy may be required
|
| Head and neck burns |
Nurse head up to reduce swelling and oedema |
| Ocular burns (See Acute eye injuries in children) |
Signs include blepharospasm, tearing, conjunctivitis
All facial burns should have assessment with fluorescein 2% eye drops to assess for corneal damage
Irrigate for at least 30 minutes with sodium chloride 0.9%. Consider topical ocular anaesthesia. Longer irrigation required if chemical injury, see below
Topical chloramphenicol to prevent secondary infection
Urgent ophthalmology review
|
| Limb burns |
Elevate the limb
Monitor perfusion distal to burn |
| Suspicion of associated carbon monoxide (CO) poisoning, Cyanide poisoning |
Liaise early with paediatric burn unit, ICU and Poisons Information, phone 131126
Apply 100% oxygen
|
| Electrical injuries |
Liaise early with Paediatric Burn Service and Intensive Care
Ensure documented history of domestic/low voltage AC, high voltage DC or lightening
Inspect for entrance/exit wounds
Consider spinal precautions
Risk of dysrhythmias, consider 24 hours ECG monitoring
Monitor for elevated CK, urine haemoglobin and haemochromogen
|
| Chemical burns |
Wear personal protective equipment for first aid givers (gloves, mask, gown, eye protection)
Remove contaminated clothing
Brush powdered agent off skin
Areas in contact with chemical should be irrigated with cool water
Irrigate to the floor with appropriate drainage so contaminated water does not cause further injury
Ocular injury:
- Alkaline injury, may require between 2-4 hours of continuous irrigation (continue until pain stops) and eye pH is 7.0-7.2
|
| Tetanus prone wound |
See Management of tetanus-prone wounds |
Consider consultation with local paediatric team when
- Suspected child abuse or self-inflicted burn
- Multiple co-morbidities
- Concern regarding ability to care for burns at home
Consider consultation with local state paediatric burns service when
For discussion, management advice and consideration of transfer for:
- Child requiring care beyond the comfort level of the hospital
- Child with pre-existing illness
- Complex burns
- >5% TBSA
- >5% full thickness burn
- Special areas: face, ears, eyes, neck, hands, feet, genitalia, perineum or a major joint, even if <5%
- All inhalation/airway injuries
- Circumferential burn
- Chemical / electrical mechanism
- Associated with trauma and/or spinal cord injury
- Children <12 months
- Suspected child abuse
For emergency advice and paediatric or neonatal ICU transfers, see Retrieval Services
Additional resources
State paediatric burns service
NSW Statewide Burn Injury Service: Burn Patient Management Clinical Guideline
QLD Paediatric Burns Centre: Management of Paediatric Burn Patient Guideline
SA WCHN Paediatric Burns Service: Burn Service Guidelines
Vic Trauma Victoria: Burns Guideline
WA Perth Childrens Hospital Burns Service: Referral Guideline
Parent information
Burns – medical treatment
Burns – prevention and first aid
Burns – rehabilitation
Last updated April 2026