Fracture Guideline Index
See also:
Monteggia fracture-dislocations - Fracture clinics
-
Summary
-
How are they classified?
-
How common are they and how do they occur?
-
What do they look like - clinically?
-
What radiological investigations should be ordered?
-
What do they look like on x-ray?
-
When is reduction (non-operative and operative) required?
-
Do I need to refer to orthopaedics now?
-
What is the usual ED management for this fracture?
-
What follow-up is required?
-
What advice should I give to parents?
-
What are the potential complications associated with this injury?
1. Summary
Monteggia fracture-dislocations can be easily missed on x-ray. If an ulna fracture is present, always look for a radial head dislocation.
All Monteggia fracture-dislocations require an urgent orthopedic assessment. Reduction is always required. Delayed or missed diagnosis is the most frequent complication.
2. How are they classified?
A Monteggia fracture-dislocation refers to dislocation of the radial head (proximal radioulnar joint) with fracture of the ulna. The Bado classification system (Table 1) describes four types.
Table 1: Bado classification of Monteggia fracture-dislocations.
|
Bado Type
|
Frequency
|
Description
|
|
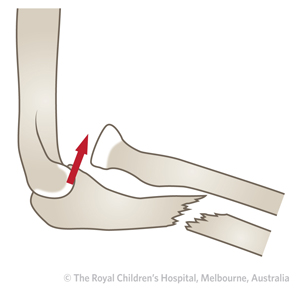
Type I
|
70%
|
Anterior dislocation of the radial head with fracture of the ulna shaft (diaphysis)
|
|
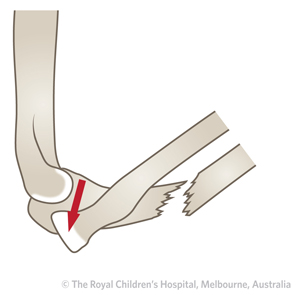
Type II
|
5%
|
Posterior dislocation of the radial head with fracture of the ulna shaft (diaphysis) or metaphysis
|
|
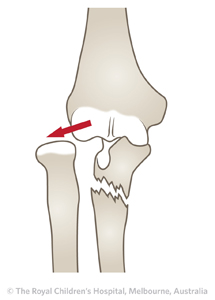
Type III
|
25%
|
Lateral dislocation of the radial head with fracture of the ulna metaphysis
|
|
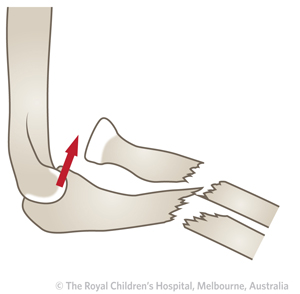
Type IV
|
Rare
|
Anterior dislocation of the radial head with fracture of the shaft (diaphysis) of the ulna and radius
|
3. How common are they and how do they occur?
These fractures are a less common injury compared to forearm fractures. The peak incidence is 4-10 years of age.
Type I fractures are usually a result of a fall on an outstretched hand with hyperpronation or hyperextension of the forearm.
4. What do they look like - clinically?
There may be diffuse swelling around the elbow, but the degree is variable. It will be painful to move the elbow in any plane.
|
!
|
The forearm may look deformed if the ulna fracture is displaced. However if the ulna has a greenstick fracture or 'plastic bowing', deformity is mild and the fracture can be easily missed.
|
5. What radiological investigations should be ordered?
Anteroposterior (AP) and lateral x-rays of the forearm that include the wrist and elbow should be ordered. There must also be a true AP and lateral view of the elbow (not just a forearm view) to assess the radiocapitellar joint.
6. What do they look like on x-ray?
|
!
|
Monteggia fracture-dislocations can be easily missed on x-ray.
If an ulna fracture is present, always look for a radial head dislocation.
To identify this injury, it is essential to have x-rays that include both the elbow and forearm.
TIP: A line drawn down the shaft of the radius should point to the center of the capitellum (radiocapitellar line) in both AP and lateral x-ray views to exclude joint dislocation.
The posterior border of the ulna should also be assessed. It should be straight, not bowed. If it is not straight, it indicates a plastic deformation injury.
|
|
|
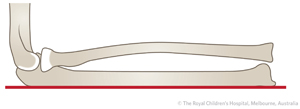
Normal ulna with straight border (red line)
|
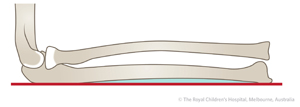
Plastic deformation of the ulna. Notice that the ulna border is not straight (shaded area).
|
Type I Monteggia fracture-dislocation (with ulna mid shaft fracture)
Figure 1: Ten year old girl with type I Monteggia fracture-dislocation. A radial head dislocation is evident as shown by the radiocapitellar line (white line). The line drawn down the shaft of the radius does not pass through the centre of the capitellum (asterix). There is an ulna midshaft fracture.
Type I Monteggia fracture-dislocation (with plastic deformation of ulna)
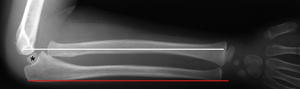
Figure 2: Type I Monteggia fracture-dislocation. A radial head dislocation is evident as shown by the radiocapitellar line. The line drawn down the shaft of the radius does not pass through the centre of the capitellum. There is plastic deformation of the ulna.
Type II Monteggia fracture-dislocations are rare
Type III Monteggia fracture-dislocation
Figure 3: Nine year old girl with type III Monteggia fracture-dislocation.
Type IV Monteggia fracture-dislocation
Figure 4: Lateral x-ray of Monteggia type IV fracture in a six year old boy, as evident by dislocation of the radial head with fractures of both the shafts of the radius and ulna.
7. When is reduction (non-operative and operative) required?
| !
|
Reduction is always required and is urgent. This is usually performed in theatre under a general anaesthetic.
|
8. Do I need to refer to orthopaedics now?
All Monteggia fracture-dislocations require an urgent orthopaedic assessment.
Other indications for prompt consultation include:
- Open fractures
- Neurovascular injury with fracture
- Extreme swelling/compartment syndrome
9. What is the usual ED management for this fracture?
The arm should be splinted and the nearest on call orthopaedic service be consulted.
10. What follow-up is required?
This should be arranged by the consulting orthopaedic team after their reduction and stabilisation of the injury. Follow-up in fracture clinic needs to be in 7 days with an x-ray.
11. What advice should I give to parents?
If identified early, these injuries will do well. Approximately 90% of children with Monteggia fracture-dislocations have good to excellent results.
12. What are the potential complications associated with this injury?
|
!
|
Delayed diagnosis is the most frequent complication.
Treatment after delayed diagnosis is much more complex and the outcomes are much less satisfactory. This is why litigation is common.
|
Other complications include:
- Nerve injury
- The radial nerve is the most commonly injured nerve (10-20%). The posterior interosseous nerve can also be injured due to its proximity to the radial head. The injury is usually a neuropraxia. Peripheral nerve examination needs to be documented. The nerve injury is usually treated expectantly.
See
fracture clinics for other potential complications.
References
Rodríguez-Merchán EC. Pediatric fractures of the forearm. Clin Ortho Relat Res 2005; 432: 65-72.
Scherl S, Schmidt A. Pediatric trauma: Getting through the night. J Bone Joint Surg Am 2010; 92(3): 756-64.
Waters PM. Monteggia fracture-dislocation in children. In Rockwood and Wilkins' Fractures in Children, 7th Ed. Beaty JH, Kasser JR (Eds). Lippincott Williams & Wilkins, Philadelphia 2010. p.446-74.
Feedback
Content developed by Victorian Paediatric Orthopaedic Network.
To provide feedback, please email rch.orthopaedics@rch.org.au