Table of contents will be automatically generated here...
Introduction
Breathing is a key priority in the Primary survey. It is essential to assess it with the potential life threats in mind. This chapter will describe how breathing differs in children, the causes of breathing problems in the paediatric age
group and their assessment and management.
How are children different?
(see how children are different section)
- They have narrower airways with higher resistance;
- The rib-cage is very compliant, so there may be internal injuries in the absence of external injury, such as rib fractures;
- The diaphragm is the dominant respiratory muscle (which makes them more prone to fatigue);
- Higher respiratory rate;
- Higher oxygen consumption;
- Lower functional residual capacity (FRC)resulting in less oxygen reserves and earlier hypoxia.
Who assesses and manages breathing in paediatric trauma?
At the Royal Children's Hospital, once the trauma team has been activated, a senior anaesthetist should typically be allocated the role of the airway doctor. Typically an emergency department doctor will be allocated the role of the assessment doctor. The assessment and management of breathing in paediatric trauma will typically be jointed co-ordinated by these two team members. When a patient is spontaneously ventilating, the airway doctor will typically examine the nose, mouth and anterior neck, to assess for airway threats. The assessment doctor will then examine the chest of the patient - observing the chest, listening for breath sounds and feeling for crepitus / emphysema and tenderness. Where the patient is ventilated, the assessment doctor may still listen to the chest and report their findings to the group, but the airway doctor - by either hand ventilating the patient, or managing a ventilator - is responsible for the management of breathing. Regardless of how the patient is ventilating, the airway doctor throughout the primary survey is responsible for monitoring airway and breathing.
Primary survey
The life threats to identify and manage with regards to breathing include:
- Tension pneumothorax
- Open pneumothorax
- Massive haemothorax
- Flail chest
Causes of respiratory distress in the injured child
Respiratory distress is common in a severely injured child. Some of the causes include:
- Direct injury to the airway
- Airway obstruction (by contamination with vomitus / blood, by swelling due to injury or loss of pharyngeal tone due to low GCS)
- Chest injury - life threats mentioned above
- Abdominal injury - peritonism or a ruptured diaphragm will lead to respiratory distress
- Aspiration
- Shock/acidosis: causes tachypnoea
- Pain/anxiety/fear: causes tachypnoea.
Breathing assessment
The assessment doctor will typically perform the initial assessment of the thorax during the primary survey. Their goal is to identify any immediate or impending life threats. The following components of the chest examination should be performed:
Expose the chest and look at:
- the work of breathing
- is the child tachypnoeic? - This may be due to injury to the chest or outside of the chest. It may also be due to pain, anxiety or acidosis
- is the child bradypnoeic? - This may be due to head injury or intoxication
- is there grunting or nasal flaring? - These are signs of severe respiratory distress and may be associated with pulmonary contusion / haemothorax / tension pneumothorax or peritonism
- the adequacy of breathing
- look for symmetry of the chest wall - a pneumothorax may cause ipsilateral hyperexpansion of the chest, with decreased movement. Similarly, a massive haemothorax will lead to decreased chest wall movement on the ipsilateral side. Paradoxical chest wall movement indicates a flail chest.
- look at the patient oxygen saturations - most children will saturate at 95% or above - if any patient fails to make sats of this level - especially when on supplemental oxygen, a cause should be sought.
- the effects of breathing
- is the child pale? Is the cyanotic? (Be aware cyanosis is a late sign - it may also be masked in an anaemic child) .
- are there any systemic effects due to hypoxaemia?
- hypoxia initially causes tachycardia; bradycardia is a late, ominous sign
- hypoxia and hypercapnia can both lead to agitation / drowsiness
- the chest for signs of external injury
- wounds, grazes, seat belt marks and bruising give important clues about how force was transmitted during an accident to the child, and this can be informative about what injuries might be predicted
Listen to the chest
- check for equal air entry - this can be difficult in the noisy environment of the resus room, especially with a crying child - however, it is important to listen in multiple areas over the chest.
- listen for heart sounds - are the normal or muffled
Feel the chest for
- Surgical emphysema - either in the chest or extending into the neck - which suggests a pneumothorax
- Clavicle or rib tenderness - suggesting a fracture
- Sternal tenderness
- Check the percussion note
If the anterior neck has not been examined by the airway doctor, ensure that it examined along with the chest. If there is concern for a cervical spine injury (as there is for most severe blunt trauma) then ensure manual in-line stabilisation is provided whilst opening the collar and examining the neck. The goal of the anterior neck injury is to exclude the following:
- Tracheal deviation
- Wounds
- Emphysema (subcutaneous)
- Laryngeal tenderness / crepitus
- Venous distension
- oEsophageal injury (injury unlikely if able to swallow easily)
- Carotid haematoma / bruits / swelling
Breathing management
Airway Ensure is patent and protected (see airway management section)
Breathing
- If breathing support is required, use positive pressure ventilation via anaesthetic T-piece prior to tracheal intubation
- A bag-valve-mask can be used with a positive end-expiratory pressure (PEEP) valve - but is less effective at consistently delivering PEEP
- A bag-valve-mask should not be used in the spontaneously ventilating child with inadequate respiratory effort - children with impaired respiratory function may be unable to generate sufficient negative pressure to open the valves in some commercially available bag-valve-masks.
- If able to spontaneously ventilate, provide oxygen at 15 litres per minute via a non-rebreather mask.
- Ensure adequate monitoring - saturation, respiratory rate, pulse, ECG, Blood Pressure.
- Continually reassess and monitor trends.
Self-inflatable bag
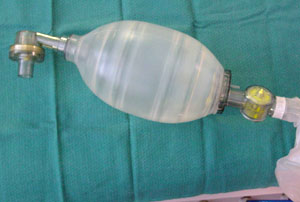
Bag and Mask Ventilation
If the airway is stable with or without an oropharngeal airway, and the patient requires breathing support, bag and mask ventilation, with a self-inflating bag, can be used.
Reassess whilst using bag and mask ventilation. If there is any further inadequacy, consider intubation. See below
Bag and mask ventilation
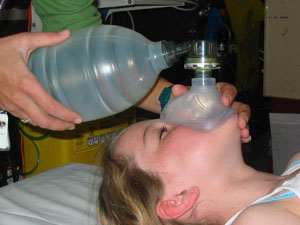
- Choose suitable size mask (chapter 2 practical procedures, bag and mask ventilation)
- Choose suitable size bag
- 3 sizes available -250mls -500mls -1500mls
Sizes of bags
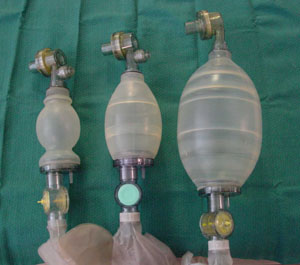
- Attach mask to bag.
- Attach to wall oxygen 15 litres/min.
- Provide insuflations sufficient to inflate chest.
- Ascultate the chest and ensure equal bilateral air entry and chest movement on insuflations.
- Allow passive expiration 3 times longer than inspiration breath.
- Rate of 20/minute.
Indications for Intubation
- Airway obstruction persists despite oropharyngeal (Guedel) airway.
- Inadequate oxygenation despite supplemental oxygen
- Hypoventilation
- Deteriorating GCS
- Needs prolonged ventilation;
- Anticipated airway obstruction - for example due to inhalational burn injury
- Management of agitation or severe distress
- To facilitate safe transport
For tracheal intubation
(see airway management section)
Specific management issues
See breathing procedures section for detailed technique for using a bag-valve-mask.
See
chest injury section for the management of the following;
- Tension pneumothorax
- Open pneumothorax
- Massive haemothorax
- Flail chest
- Rib fractures
- Lung contusions.
Suggested reading list
- Advanced Paediatric Life Support. 3rd ed. London: BMJ Books 2001. Chapters 4 (Basic life support); 5 (Advanced support of the airway and ventilation); 22 (Practical procedures: airway and breathing).
- Taussig L, Landau L, Le Souëf P; Martinez F; Morgan W; Sly P (eds) Pediatric Respiratory Medicine. St Louis: Mosby 1999. Chapters 21 (Assisted ventilatory support and oxygen treatment) and 25 (Lung trauma: toxin inhalation and ARDS).
- Fleisher G, Ludwig S (eds): Textbook of Pediatric Emergency Medicine (4th ed). Philadelphia: Lippincott 2000. Chapters 1 (Resuscitation: pediatric basic and advanced life support); 5 (Emergency airway management: rapid sequence induction); 104 (Major
trauma); 106 (Neck trauma); 107 (Thoracic trauma); 112 (Otolaryngologic trauma); 114 (Burns)
- Bersten A, Soni N (eds): Oh's Intensive Care Manual (5th ed) London: Butterworth Heinemann 2003. Chapters a (The critically ill child); b Upper airway obstruction in children; c (Acute respiratory failure in children; d (Paediatric trauma).
- Macnab a, Macrae D, Henning R (eds): Care of the critically ill child. London: Churchill Livingstone 1999. Chapters 2.6 (Trauma: cranial, spinal and multiple); 4.2 (Smoke inhalation); 4.4 (Trauma of individual systems); 6.2 (Intubation); 6.3 (Securing the
airway); 6.4 (Assisted ventilation).