Breastfeeding your baby is a natural way to feed your baby, and has short- and long-term benefits for you both. If you have chosen to breastfeed your baby and are able to, you may need some support while learning to breastfeed until you establish a breastfeeding routine with your baby.
Breastfeeding is not always easy. Despite the challenges, it is worthwhile persisting with breastfeeding, as your breastmilk uniquely meets your baby's needs.
If you have difficulties with breastfeeding, a midwife, maternal child health nurse or your GP are available to help and can provide support or answer any concerns.
Benefits of breastfeeding
Breastfeeding is the most natural way to feed your baby. Providing your baby with any amount of breastmilk is better than none.
Breastmilk uniquely meets your baby’s needs and contains protective properties (antibodies) that protect your baby from disease and infection. Breastmilk also helps with gut and brain development and is easy for babies to digest and absorb. If your baby is breastfed, they won’t require any other food or drink until they are about six months old.
Breastfed babies also:
- have a lower risk of developing ear infections, respiratory infections, allergies, asthma, type 1 diabetes and obesity
- benefit by the sucking action, which promotes development of their mouth, teeth and jaw and improves long-term physical development
- learn to recognise when they are hungry or full.
Positioning and attachment
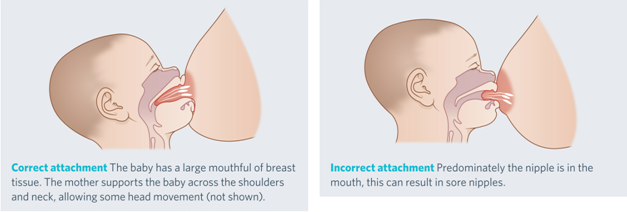
Positioning and attachment is important for breastfeeding. Your baby’s mouth should be wide open and they should have a large amount of breast tissue in their mouth, not just the nipple. This helps your baby take in enough milk and ensures you continue to produce the right amount of breastmilk. If your baby is not attached properly, feeding may be painful and you may not make enough milk to meet your baby’s needs.
- Hold your baby at the level of your breasts, close to you. Place them on their side with their chest and body against your chest/stomach.
- Support your baby’s body along your arm with their bottom and legs wrapped around your side. There should be no gap between you and baby.
- Support your baby’s neck and shoulders with your hand, allowing some head movement.
- When your baby’s mouth is wide open, bring them to your breast gently by moving their upper body.
- Aim the nipple at the roof of your baby's mouth. Your nipple should be in the back of your baby’s mouth and not in the front of the mouth.
- A well-attached baby has lips very wide apart, curved outwards and placed flat against your breast.
Try not to change your position or release your hold on your breast until your baby is rhythmically sucking and swallowing well, and there is no pain in your nipple or breast. If it hurts while your baby is feeding, it could mean that your baby is not attached properly. Always ask for help if you are unsure whether your baby is positioned or attaching correctly.
How often should I breastfeed my baby?
You should breastfeed your baby whenever they seem hungry. Babies may also be breastfed for comfort, when they are tired or when they are upset. Generally, young babies feed every two to four hours (eight to 10 times a day).
- Initially feeds can take up to one hour, but as your baby grows and your volume of milk increases, the time it takes for your baby to feed and the frequency of feeds will decrease.
- Feeding regularly will ensure your body makes enough milk to meet your baby’s needs.
- Encourage your baby to finish one side before offering the second side.
- There is no need to time each feed – your baby will be able to self-regulate and take the amount of milk they need.
You can make sure that your baby is getting enough breastmilk by checking that they have five to eight wet nappies each day, are growing well (using a growth chart) and are generally alert and content when awake.
If your baby seems more hungry than usual, you can try increasing the frequency of their feeds or allow them to feed for a longer period ensuring that your baby ‘drains’ the breast so they get the fatty ‘hindmilk’, which is more satisfying. Some parents believe that offering formula or solids will keep their baby full and help their baby sleep better or for longer periods, however this is not true. Offering infant formula or solid food before six months of age will reduce your milk supply.
You should seek support from a GP or maternal child health nurse if you are worried about your baby’s feeding or their growth and development.
Expressing and storing breastmilk
Sometimes, it may be necessary to express and/or store your breastmilk. This may be by choice (e.g. you are returning to work or study), or if your baby is unable to breastfeed (e.g. if your baby is sick and in hospital).
Expressed breastmilk can be stored in the fridge for three to four days, and in a freezer for three months.
Common problems with breastfeeding
Too much milk
This is sometimes an issue soon after your baby is born, but your body should adjust once your baby establishes a feeding pattern. Until your supply matches your baby’s needs, expressing a small amount at the beginning or end of a feed can help to reduce discomfort.
Not enough milk
Mothers are often concerned that they are not producing enough breast milk, but low supply is usually only temporary. Strategies to increase your breastmilk supply include:
- ensuring your baby is positioned and attached correctly at each feed
- feeding more frequently (e.g. offer the breast between usual feeds)
- offering the breast for comfort
- alternating which breast is offered first at a feed and feeding from each breast more than once each feed
- expressing between feeds.
If supply is low and strategies to increase your supply do not seem to be increasing the volume of breastmilk, you can seek support from your maternal and child health nurse.
Mastitis
Mastitis is inflammation of the breast and can cause fever, pain, swelling and redness. Mastitis occurs when there is poor draining of milk and nipple damage, which causes a blocked milk duct.
Treatment for mastitis includes frequent and effective removal of milk, either by expressing or offering more frequent breastfeeds (ensuring that positioning and attachment are correct).
A warm cloth applied to the breast before and during a feed can be helpful for reducing pain.
Key points to remember
- Breastmilk is the best source of nutrition for your baby.
- Any amount of breastmilk is better than none.
- There are several helpful resources available to mothers for help and support with breastfeeding.
For more information
Common questions our doctors are asked
When is it best to start introducing solids to my baby’s diet?
You should start to introduce solids in addition to breastfeeding when your baby is around six months of age. By the time your baby reaches six months, they will begin to show signs that they are ready for solid food, including being able to sit with support, good head control, showing interest in others eating and opening their mouth when food is offered. While babies are learning to eat, they eat very little.
Around this time, overnight feeds can also be reduced.
Despite starting solids, breastmilk remains the main source of nutrition for your baby. In Australia, mothers are encouraged to breastfeed until at least 12 months of age.
Are there things I should avoid in my diet while I’m breastfeeding?
Most women can eat their normal range of foods without causing problems for their baby. To meet your energy needs, remember to have a sandwich or snack each time you breastfeed or express milk.
Alcohol should be avoided as it can pass through breastmilk to the baby. If you do drink alcohol, you should wait at least 2 hours before breastfeeding your baby. Caffeine (e.g. tea, coffee and energy drinks) should also be limited as large amounts in your diet can cause your baby to become irritable.
There are a small number of medications that can be passed to your baby through breastmilk, so you should always ask your GP to prescribe medications that can be taken while breastfeeding. Also check with your GP before taking over-the-counter medicines like vitamins or other complementary (natural) medicines. Avoid smoking and illicit drugs.
My baby is nearly 12 months old – can I keep breastfeeding her after she turns one?
In Australia, breastfeeding is encouraged until your baby is at least 12 months old, and then beyond as you desire. Benefits for your baby will continue for as long as breastfeeding is maintained.
Developed by The Royal Children's Hospital Dieticians and Lactation Consultants. We acknowledge the input of RCH consumers and carers.
Reviewed January 2018.
This information is awaiting routine review. Please always seek the most recent advice from a registered and practising clinician.
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit
www.rchfoundation.org.au.