1. Summary
This guideline will include the management and referral guidelines for injuries of the fingertip.
2. How are they classified?
Can be classified by:
- Crush or cutting mechanism
- Open or closed
- Subungual haematoma
- Nail bed intact
- Amputation or avulsion
Definitions:
Simple laceration: Single linear laceration.
Stellate laceration: Multiple converging lacerations that typically resemble a star shape.
Crush injury: Complex crush injury that causes fragmentation.
Burst laceration: Laceration pattern caused by high energy blunt force.
Nail bed avulsion: Nail plate is forcefully torn away where a portion of nail bed attached.
Subungual haematoma: Bleeding within the space between nail bed and nail plate.
Partial / complete amputation: Traumatic injury that causes partial or complete removal of fingertip.
3. How common are they and how do they occur?
Fingertip injuries are common in children, particularly younger children ‘exploring’ without the awareness of risk.
The most common mechanism is a crush injury, often a door or hinge, but can also be caused by a direct blow or sharp objects
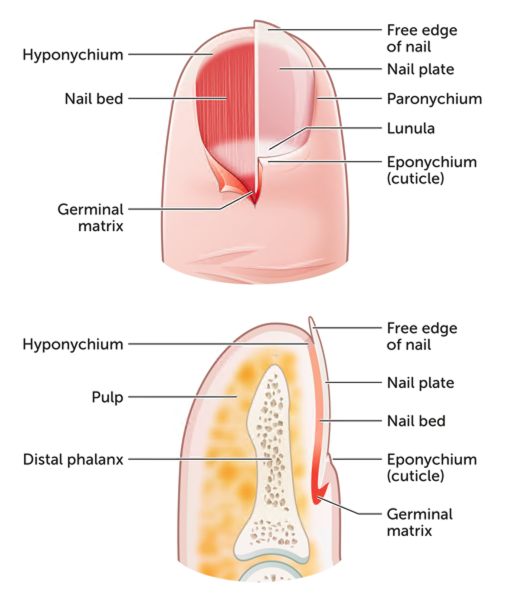
4. What do they look like clinically?
- Nail injuries usually present with localised pain, swelling or bruising.
- The nail plate may be intact or damaged.
- A large (>50%) subungual haematoma or displacement of the proximal edge of the nail plate out of the eponychial fold may indicate an underlying fracture.
- Seemingly minor nail bed injuries may conceal more serious injuries such as a
Seymour fracture or tendon injury.
- Seymour fracture: Injury to the distal phalanx with associated nail bed injury (often seemingly mild), and injury to the growth plate. The nail plate in often displaced superficial to the eponychium.
- Lacerations of the distal phalanx caused by a sharp object (e.g. broken glass) may result in injury to the underlying tendon.
- In young children, awake assessment of tendon function can be very challenging or even impossible.
- Loss or weakness of flexion or extension of the distal interphalangeal joint (DIPJ) may indicate tendon rupture.
5. What radiological investigations should be ordered and what do they look like on x-ray?
Three plain film views should be obtained; a lateral, AP and oblique views
|
Tuft fracture |
 |
|
Seymour fracture |
.png) |
6. Do I need to refer to Hand Surgery now?
- Subungual haematoma extending >50% of nail plate
- Distal phalanx fracture with an associated nail injury
- Nail plate avulsion
- Crushed nail bed
- Lacerations extending into nail bed, paronychial or eponychial fold
- General anaesthetic necessary to get adequate control for fingertip repair
Urgent referral to hand surgery
Precise repair of the nail bed is important to optimise long-term cosmesis of the finger and nail. This is usually best performed by a hand surgery team under anaesthesia, particularly in younger children.
7. What is the usual ED management of this injury?
In young or uncooperative children, consider early analgesia, procedural sedation and age-appropriate distraction techniques. Older children may tolerate repair under a regional block.
Most fractures (tufts) are very small and don’t require reduction of the phalanx.
Check tetanus immunisation status.
Antibiotics:
- Routine antibiotic prophylaxis is not recommended for simple and uncontaminated injuries. This includes clean open fingertip wounds with an associated undisplaced fracture or tuft fracture.
- Irrigation and antibiotic prophylaxis are indicated in animal bites or heavily contaminated injuries. Please refer to cellulitis. These injuries usually require washout in theatre.
Open finger injuries require a secure, robust dressing. Consider reinforcing with a splint and crepe bandage.
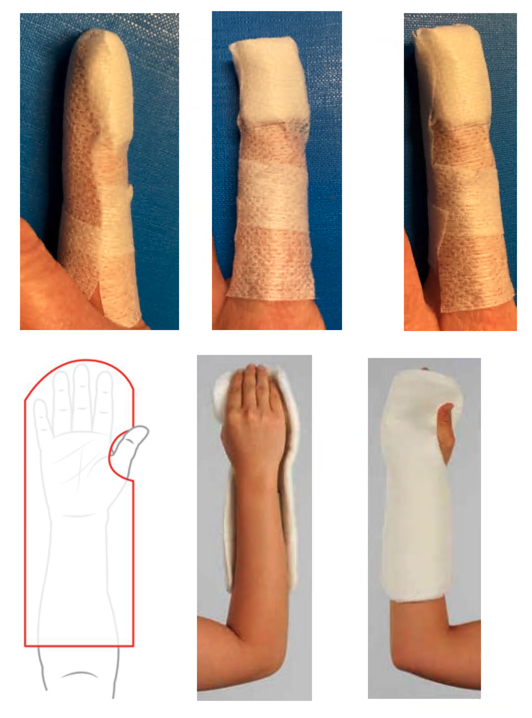
Neutral hand splint, which should be held in place with crepe bandage, with cotton placed between the fingers to protect the skin from maceration over the following week/s.
Management of specific injuries are listed in the table below.
| Injury type |
ED management |
|
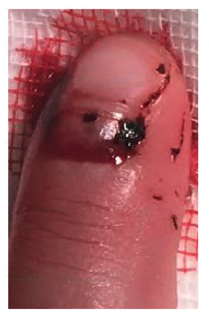
Seymour fracture
|
Suspected
Seymour fractures should be referred to hand surgery for urgent operative management. |
|
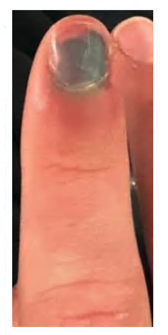
Distal phalanx fracture/Tuft fracture
|
See
Finger fracture
Seymour fractures are open fractures and are associated with significant complications. They may only have subtle radiographical changes. |
|
Subungual haematoma

|
The treatment of a subungual haematoma is controversial:
Most uncomplicated subungual haematoma injuries where nail margins are intact and there is no evidence of a displaced fracture, can be treated with either nail trephination or close follow up.
The degree of pain often influences the decision whether to person trephination. Seek senior clinician advise.
Subungual haematomas that do not meet the above criteria should have nail plate removal for nail bed assessment and repair.
|
|
Nail bed injuries
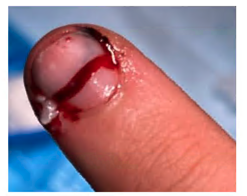
|
Simple nail bed lacerations require removal of the nail plate and repair of the nail bed by a trained clinician.
If a trained operator is not available is not available, refer to hand surgery.
Complicated nail bed injuries or injuries with underlying displaced fractures require hand surgery referral.
|
|
Burst lacerations of the pulp
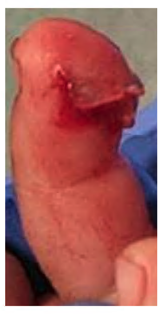
|
Laceration under half the circumference of the finger:
Adhesive strips and in simple non-bleeding lacerations, consider tissue glue.
Lacerations over half the circumference of the finger:
Closure with absorbable sutures
(example as per laceration CPG); may require referral to hand surgery.
|
|
Pulp avulsion
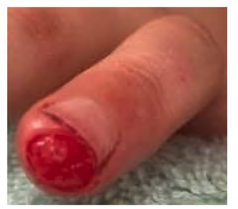
|
Avulsions of the pulp smaller than the size of the nail will heal very well and only require a simple non adherent dressing over the wound and review in 2-3 days.
Larger avulsions require hand surgery referral.
|
|
Fingertip amputations
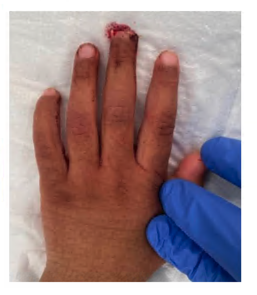
|
See
amputation (within trauma guideline)
Preserve the amputated finger.
- Moisten appropriately-sized sterile gauze with sterile saline solution.
- Wrap the severed part in the moistened sterile dressing, preserving all amputated material.
- Place the severed part in a watertight container (plastic bag) and ensure tightly sealed.
- Place the container on ice or cold packs (if available).
- Confirm identification and place hospital ID sticker on container.
- Keep amputated digit in safe place close to patient.
Do not freeze or use dry ice. |
8. What follow up is required?
Nail bed injuries should have follow up with hand surgery.
Nearly all other injuries can be followed up with GP within a week.
9. What advice should I give to parents?
Increasing pain which is uncontrolled with simple analgesia and distraction should prompt urgent review as it may indicate a tight dressing or infection.
- Elevate limb as possible (eg sling)
- Keep dressing dry (particularly challenging in toddlers and require extra supervision)
- Simple pain relief
- The nail may take up to 9 months to return to normal appearance
- Education of finger injury prevention strategies; door stoppers or finger shield hinges
10. What are the potential complications associated with these injuries?
- Wound Infection
- Nail deformity (particularly when a nail bed injury has been missed)
- Soft tissue deformity
- Unrecognised Seymour fracture causing osteomyelitis, growth arrest and nail deformities
Delayed intervention (more than 2-3 days) has been associated with higher rates of complications.
Reference list
- Venkatesh, A., Khajuria, A., & Greig, A. (2020). Management of Pediatric Distal Fingertip Injuries: A Systematic Literature Review. Plastic and reconstructive surgery. Global open, 8(1), e2595. https://doi.org/10.1097/GOX.0000000000002595
- Weir Y. (2018). Fingertip injuries in children: a review of the literature. Emergency nurse : the journal of the RCN Accident and Emergency Nursing Association, 26(3), 17–20. https://doi.org/10.7748/en.2018.e1795
- Edwards, S., & Parkinson, L. (2019). Is Fixing Pediatric Nail Bed Injuries With Medical Adhesives as Effective as Suturing?: A Review of the Literature. Pediatric emergency care, 35(1), 75–77. https://doi.org/10.1097/PEC.0000000000000994
- Allergott C et al.(2008) Pediatric Fingertip Injuries: do prophylactic antibiotics alter infection rates? Pediatr Emerg Care 2008;24(3)148-52
- Patel, L, (2014) Management of Simple Nailbed Lacerations and Subungual Hematomas in the Emergency Department Pediatr Emer Care 2014;30:742-48
- Cornwall, R. (2012) Pediatric Finger Fractures: Which Ones Turn Ugly? J Pediatr Orthop 2012;32:S25-S31