|
Head and face
|
- Face, scalp and skull
- Bleeding, lacerations, bruising, swelling, depressions/irregularities in the skull (to suggest skull fracture), bruising behind the ears (Battle’s sign: may indicate base of skull fracture), periorbital bruising (“Racoon eyes”: may indicate base of skull fracture)
- Eyes
- Palpate bony margins of orbit for fracture. Test eye movements, pupillary reflexes and vision. Inspect for penetrating injury (see Penetrating eye injury), irregular iris, foreign bodies, subconjunctival haemorrhage, hyphema
- Ears
- Bleeding, blood behind tympanic membrane (suggestive of base of skull fracture), tympanic membrane perforation (in blast injuries). Assess hearing
- Nose
- Bleeding, septal haematoma, CSF leak, palpate for bony crepitus or deformity
- Mouth
- Wounds to the lips, gums, tongue or palate
- Teeth
- Jaw
- Identify pain, trismus or malocclusion and palpate for bony step
|
|
Neck
|
Inspect neck, whilst maintaining manual in-line stabilisation if C-spine has yet to be cleared. Open collar to do this
Examine anterior neck for blunt or penetrating trauma by looking/feeling for the following (TWELVE-C):
- Tracheal deviation
- Wounds
- Emphysema (subcutaneous)
- Laryngeal tenderness/crepitus
- Venous distension
- OEsophageal injury (unlikely if child can swallow easily)
- Carotid haematoma/bruits/swelling
Assess C-spine if not completed in secondary survey. See C-spine assessment
|
|
Chest
|
- Observe work of breathing and effectiveness of breathing
- Assess for any asymmetrical or paradoxical chest wall movement
- Inspect for signs of injury such as bruising, seatbelt marks, wounds
- In cases of stabbing or other assault, look for ‘hidden’ wounds by checking areas such as axillae
- Palpate for bony tenderness over ribs, crepitus (indicating subcutaneous emphysema)
|
|
Abdomen
|
- Inspect for bruising (eg from seatbelt or handlebar injury), abdominal distension
- Palpate for signs of peritonism such as guarding or rigidity
- Palpate for tenderness over the liver, spleen, kidneys and bladder
|
|
Pelvis and perineum
|
- Inspect for grazes over iliac crests, bruising, deformity
- Feel for pain or crepitus on gentle palpation of bony prominences
- Assess for pelvic instability by gentle compression of the iliac crests
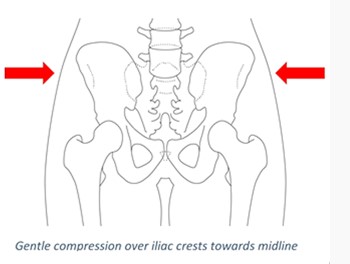
- Stressing/springing the pelvis is not recommended
- Genital, if pelvic injury or high chance of injury needs external examination. Should include perineum
|
|
Limbs
|
Most common missed injuries, especially hands
- Inspect for wounds, bruising, open fractures, burns, abrasions
- Feel for soft tissue and bony tenderness or swelling, joint movement and stability
- Examine pulses and perfusion
- Examine sensory and motor function of any nerve roots or peripheral nerves that may have been injured
- Assess gait if possible
|
|
Back and spine
|
- A log roll should be performed if spinal precautions required
- Inspect entire length of back and buttocks
- Palpate then percuss spine for tenderness
- Palpate scapulae and sacroiliac joints for tenderness
|