See also
Communicating procedures to children
Minimising distress in healthcare setting
Procedural pain management guideline
Peripheral Intravenous device management guideline
Key points
- Anxiety, pain, distress and subsequent needle phobia are associated with repeated attempts at intravenous (IV) access; appropriate preparation can minimise the distress caused
- It is important to justify the need for the procedure and combine with blood sampling if needed
- If available, consider ultrasound guidance if intravenous cannulation is predicted to be difficult or a longer-term access device if prolonged therapy is anticipated
- Some children are at higher risk of decompensation with multiple IV attempts, eg child with congenital heart disease and single ventricle physiology
Background
- Multiple attempts at intravenous insertion can cause significant distress for patients so alternatives should always be considered within the clinical context:
- oral fluids or medications if child can tolerate
- fluids or medication via NG, or via PEG in a child with gastrostomy tube
- IM or intraosseous medications in emergencies
- Cannulas inserted over joints, in areas of flexion or in the lower limb are more likely to fail than those inserted in the hand or forearm
- Monitor IV site for signs of infection or extravasation
- If prolonged IV therapy is anticipated, plan for longer term access eg PICC or midline
- Remove unused cannulas to minimise infection
Selection of intravenous access
The following guidance should be considered when referring patient for IV access
| Duration IV access required |
Choice of cannula device |
|
<7 days |
Peripheral IV access
Predicted dwell time: forearm > hand > foot > cubital fossa
Ultrasound guided peripheral IV access (may last up to 7 days) |
7-14 days or
failed peripheral IV attempts |
Upper arm midline, PICC (peripherally inserted central catheter) or percutaneous CVAD (central venous access device) |
| >14 days or requiring central access (eg cytotoxic medication) |
PICC, percutaneous CVAD |
| >6 weeks |
Consider tunnelled (surgical) CVAD or port |
If available, consider ultrasound guidance by an experienced clinician if intravenous cannulation is predicted to be difficult or prolonged therapy is anticipated (see table below)
Potential complications
- Unsuccessful procedure or multiple attempts
- Accidental arterial cannulation
- Bright red backflow of blood into IV cannula
- The cannula flashback appears pulsatile or there is pulsatile movement of blood in IV tubing
- Backflow of blood into IV tubing despite fluid bag at level higher than IV insertion site
- IV inserted in a 'high risk' area ie antecubital fossa
- Management if uncertain
- Do not use cannula
- Urgent blood gas analysis from inserted cannula
- Thrombophlebitis or infection
- Extravasation injury
Equipment, analgesia, anaesthesia and sedation
| Child |
Infants <3 months
- Oral sucrose with a pacifier should be used (see Acute pain management), or breastfeeding infant during procedure if practicable
- Give parent or carer option to hold infant during procedure and employ multisensory stimulation
Older infants and children
- Apply topical anaesthetic creams in advance of procedure whenever possible
- Lidocaine 4% cream (LMX®): 30 minutes
- Amethocaine 4% (AnGel®): 45 minutes
- Lidocaine 2.5% and Prilocaine 2.5% (EMLA™®): 60 minutes
- Explain what you are doing in a developmentally appropriate way
- Use play therapy, distraction, relaxation and other coping skills,
- Consider oral midazolam, intranasal dexmedetomidine or nitrous oxide if available for anxious children (see Procedural sedation)
- Give parent or carer option to hold child during procedure and employ multisensory stimulation (see Minimising distress in healthcare setting)
- Coolsense™ or Buzzy® bee may be used where available
|
| Setting |
- Whenever possible, procedures should be performed away from the bedside ie in treatment room
- Get helpers: at least one other staff member for holding/taping
- Adequate lighting
- For ultrasound guided access, consider infiltration with local anaesthetic with a 30G needle (insulin syringe)
|
| Equipment |
Have equipment ready before the child enters the room
- IV starter pack/dressing pack or equivalent
- Skin preparation: alcohol 70% or chlorhexidine 2% swabs
- IV cannula
- Sterile syringe and blood tubes (for blood)
- 10 mL normal saline
- Sterile syringe to flush
- Saline primed connector or extension set
- Sterile IV dressing eg Tegaderm™
- Taping, splint and crepe bandage or Tubigrip®
Additional equipment if performing ultrasound guided intravenous cannulation
- Ultrasound machine with high frequency linear transducer
- Ensure appropriately disinfected between patients with approved instrument grade disinfectant wipes, including tranducer, leads and screen
- Sterile cover for ultrasound transducer
- Sterile gel
Additional equipment to consider
- Transilluminator, Accuvein® or other vein finder tool as required/available
- Distraction aids such as books or videos
- Towel or pillowcase to obscure child's view of procedure
|
| Proceduralist |
- Decontaminate hands and on clean gloves immediately before cannulation
- Use sterile gloves if midlines or long cannulas are being inserted
- Refer to Latex allergy guideline if necessary
|
Procedure
- Explain the procedure to the child and parents and obtain verbal consent
- Ensure to perform appropriate hand hygiene throughout
Sites
- Using a tourniquet assess for the most suitable vein; in children, the most suitable vein may not necessarily be palpable
- Dorsum of the non-dominant hand is preferred with the vein running between the 4th and 5th metacarpals is most frequently used
- In addition to the usual sites in adults, commonly used sites in children include the volar aspect of the forearm, dorsum of the foot and the great saphenous vein at the ankle
- Consider practicalities of splinting eg areas of flexion such as elbow, foot in a mobile child
Transillumination
- Application of a cold light directly to the skin in a darkened room can be helpful in finding veins in neonates and infants
- Only cold lights (usually fibre-optic sources) should be used. Normal torches can burn the skin and should not be used
- Transillumination is a useful skill which requires practice but is simple once mastered
Ultrasound guided approach
- Scan carefully for the most suitable vein
- The most commonly used vein with the highest success rate in children is the cephalic vein in the proximal forearm
- Other sites include the long saphenous vein at or just proximal to the ankle, or the medial aspect of the upper arm (midline catheter)
Assess difficulty of intravenous cannulation
- History of 'difficult' IV access in the medical record
- Patient or caregiver reports a history of difficulty in cannulating or venepuncture
- Clinical assessment
- The DIVA (difficult intravenous access) score may be helpful
| Predictor |
0 Points |
1 Point |
2 Points |
| Visible Vein |
Visible |
- |
Not visible |
| Palpable Vein |
Palpable |
- |
Not palpable |
| Age |
≥ 36 months |
12-35 months |
< 12 months |
Score of 4 or more means >50% chance of failed initial attempt
If difficult intravenous cannulation is predicted based on the above criteria, ultrasound guided insertion should be considered if the equipment and expertise is available.
Some children are at higher risk of decompensation with multiple IV attempts, eg congenital heart disease with single ventricle physiology. In this scenario if >2 attempts are required involve the senior clinician and consult the treating cardiology team
Technique
Holding
- Ask assistant to stabilise limb, by holding joints above and below if necessary
- When applying tourniquet, be careful not to pinch skin or compress artery
- In infants, when accessing the hand, grasp as shown; this achieves both immobilisation and tourniquet (see Figure 1 below)
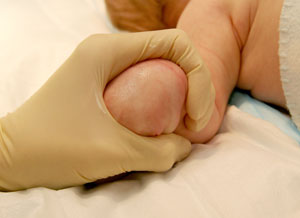 |
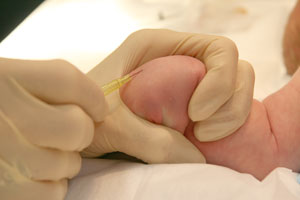 |
| Figure 1: holding an infant's hand |
Figure 2: shallow angle of insertion |
Inserting the cannula
- Decontaminate skin with alcohol 70% or chlorhexidine 2% swabs and leave to dry for at least 30 seconds. Use 'no-touch' technique for insertion after decontamination
- Insert just distal to and along the line of the vein
- Angle at 10-15° (see Figure 2 above), or between 30-45° if using ultrasound guidance
- Advance needle and cannula slowly
- A 'flash back' of blood may not occur for small veins and 24G cannula
- Once in the vein, advance the needle and cannula slowly a further 2-3 mm along the line of the vein before advancing cannula off needle
- Apply slight occlusive pressure to the vein above while preparing to take blood samples
- Dispose of sharps appropriately
Taking blood samples
- For 24G cannula it is often easier to let blood drip passively into collection bottles (see Figure 3 below)
- When taking blood for culture or gas from a small cannula, aspirate blood from the hub of the cannula using a blunt 'drawing up' needle and syringe (see Figure 4 below)
- For a larger cannula, a syringe can be used to aspirate blood
- For 22G or 20G cannula a vacuum connector can be used
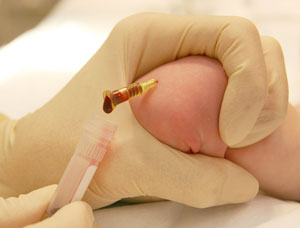 |
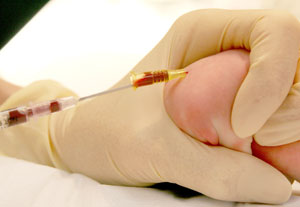 |
| Figure 3: passive blood collection for infants |
Figure 4: aspirating blood for culture or gas
|
Securement
- Remove tourniquet before strapping
- Connect the saline-primed 3-way connector or extension set to the end of the cannula by screwing it firmly on. Flush the connector tubing with more saline to confirm intravenous placement
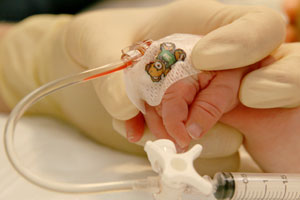
- Use sterile tapes to secure the hub and a clear dressing over the cannula site such as Tegaderm™. Ensure that the proximal tip and area of skin around are always easily visible (Figure 5 below). Extravasation injuries can occur especially if the site
is not readily accessible for regular nursing checks
- Consider placing a small piece of sterile gauze underneath the hub of the cannula to prevent pressure areas
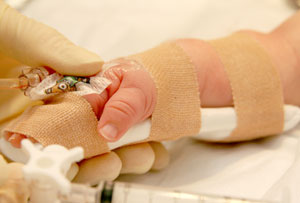
- Tapes and splint should secure the limb proximal and distal to the cannula (keeping thumb free) but not too tightly (Figure 6 below)
- Arm splints are not required for lines placed in the cephalic vein in the forearm (typically ultrasound guided). Cover the whole distal extremity in net bandage (eg surgifix tubular-fast). In very young children, consider bandaging the other hand
as well to prevent them from removing the cannula
 |
 |
| Figure 5: secure with TegadermTM so that IV site is visible |
Figure 6: Strap so that joint is immobilised, but avoiding tapes being too tight |
Post-procedure care
- Documentation of procedure and device in child's chart
- Indication for insertion
- Size, site, number of attempts, any difficulties
- Maintenance
- Plan for removal
- Running a 'drug line' (3-5 mL/hr of sodium chloride 0.9%) through the cannula may keep it patent for a longer period of time
- Regularly inspect insertion site for complications (tenderness, blockage, inflammation, discharge) as per local hospital policy. Check the other hand if it has also been bandaged
- Unless complications develop, the peripheral IV should remain in situ until IV treatment is complete
- Daily documented review by medical team regarding ongoing need for IV access or whether it can be removed to minimise infection risk
Difficulty with IV insertion
- Each clinician should have a maximum of 2 attempts before escalating
- Strongly consider ultrasound assistance, if available
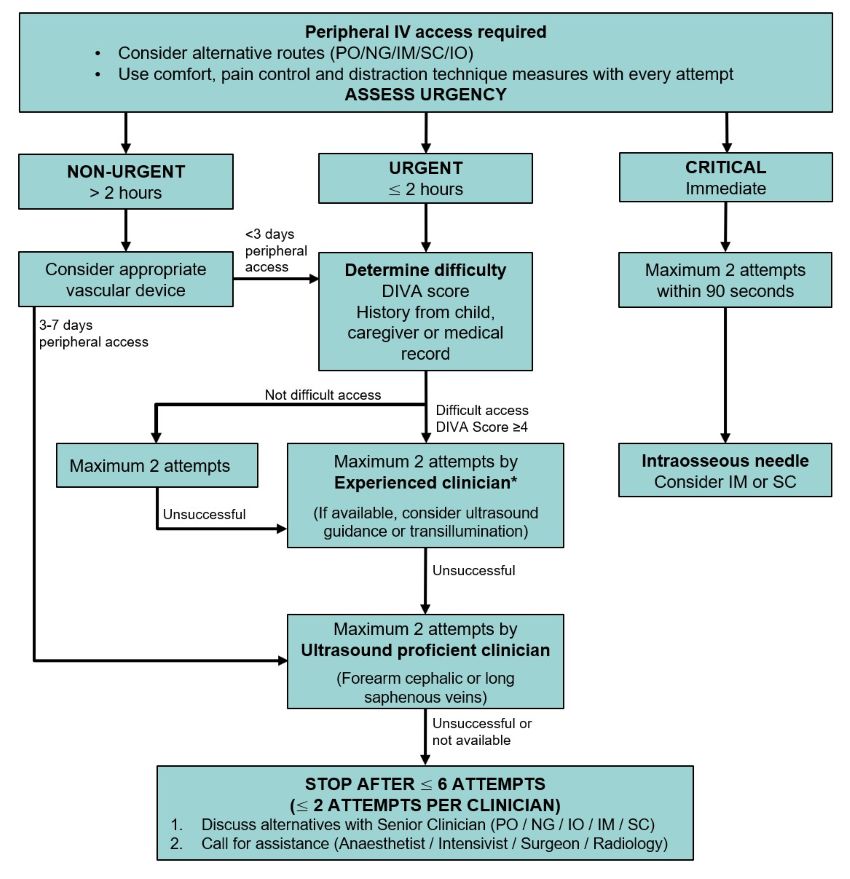
*Experienced clinician with at least 2 years of acute paediatric experience
For emergency advice and paediatric or neonatal ICU transfers, see Retrieval Services
See video
Watch the Intravenous Access Peripheral video:
Parent information
Intravenous cannula factsheet (NSW)
Care of your IV drip (SA)
Cannula (WA)
Peripheral intravenous cannula (WA)
Last updated November 2025
Reference list
- Australian Commission of Safety and Quality in Healthcare
- Bennet J, Cheung M. Intravenous access in children. Paediatrics and Child Health. June 2020. Vol 30, issue 6 pg 224-229
- Lake C, Beecroft C. Extravasation injuries and accidental intra-arterial injection. Continuing Education in Anaesthesia Critical Care & Pain. 2010. 10(4), p109-113
- Queensland Department of Health. Peripheral intravenous catheter. https://www.health.qld.gov.au/__data/assets/pdf_file/0025/444490/icare-pivc-guideline.pdf (viewed 14 November 2024)
- Queensland Paediatric Emergency Care. Peripheral intravenous cannula taping. April 2022 https://www.childrens.health.qld.gov.au/__data/assets/pdf_file/0025/179701/peripheral-intravenous-cannula-PIVC-taping-nursing-skill-sheet.pdf (viewed 14 November 2024)
- Riker MW, Kennedy C,
Winfrey BS, Yen K and Dowd MD. Validation and refinement of the difficult intravenous access score: a clinical prediction rule for identifying
children with difficult intravenous access. 2011. 18(11), p1129-34
- Sen S, Chini EN, and Brown MJ. Complications after unintentional intra-arterial injection of drugs: risks, outcomes, and management strategies. Mayo Clin Proc. 2005. 80(6), p783-95.
- Starship. Intravenous line insertion. 2024 https://www.starship.org.nz/guidelines/intravenous-line-insertion/ (viewed 14 November 2024)
- The Sydney Children's Hospital Network. Peripheral intravenous catheters -- clinical standard. 2024 https://resources.schn.health.nsw.gov.au/policies/policies/pdf/2013-9077.pdf (viewed 14 November 2024)
- Western Australia Child and Adolescent Health Service. Peripheral intravenous cannula insertion and management. August 2024. https://cahs.health.wa.gov.au/-/media/HSPs/CAHS/Documents/Health-Professionals/Neonatology-guidelines/Peripheral-Intravenous-Cannula-PIVC-Insertion-and-Management.pdf?thn=0 (viewed 14 November 2024)