See also
Unsettled or crying babies
Gastroenteritis
Non-IgE mediated food allergy
Key points
- Gastro-oesophageal reflux (GOR) is common in healthy, thriving infants and does not require investigation or treatment
- Gastro-oesophageal reflux disease (GORD) is defined as troublesome symptoms (adversely affecting feeding, growth or respiratory status) related to GOR
- Consider cow milk protein allergy in infants with GORD symptoms
- Do not use acid suppressant therapy as a diagnostic trial for irritable infants
Background
Gastro-oesophageal reflux (GOR) occurs when the lower oesophageal sphincter is immature and either relaxes too often or doesn't close properly. This allows the passage of gastric contents into the oesophagus, often with effortless vomiting,
or 'possets'. It is a physiological process that occurs several times a day in healthy infants.
GOR
- is common, affecting at least 40-65% of otherwise healthy infants
- usually begins before 8 weeks of age, peaks at 4 months and resolves by 1 year of age in the majority of cases
- does not cause crying and irritability in healthy infants. Infant crying peaks at 6-8 weeks, and co-incidentally some babies with simple GOR may also be unsettled, see unsettled babies
- rarely requires investigations
- can usually be managed with parental education, support and anticipatory guidance
There is insufficient evidence to support the diagnosis or management of "silent reflux"
Gastro-oesophageal reflux disease (GORD) is defined as GOR causing 'troublesome symptoms', which may cause pathologic complications such as
- feeding problems eg refusal to feed, pronounced irritability with/after feeding, gagging/choking with feeding
- respiratory symptoms eg aspiration, chronic cough, wheezing, recurrent pneumonia
- slow weight gain
- haematemesis
- anaemia
- dystonic neck posturing (Sandifer syndrome)
GORD is more common in children with known underlying medical conditions such as neurological disabilities, pulmonary dysfunction, and congenital abnormalities such as corrected trachea-oesophageal fistulas. It is outside of the scope
of this guideline to address these specific patient groups.
A subset of infants with non-IgE mediated cow milk protein allergy (CMPA) can present with symptoms of persistent regurgitation, vomiting and irritability indistinguishable from GORD. CMPA is more likely in patients with blood/mucous
in their stool, chronic diarrhea or a personal or family history of atopy. See Non-IgE mediated food allergy
Assessment
- Usually, both GOR and GORD can be diagnosed on detailed history and examination
- Direct observation of a feed by an experienced clinician can be useful to identify exacerbating factors, eg excessive air swallowing caused by poor latch or difficulty managing milk flow
Reconsider diagnosis if any of the following red flag features are present
General signs/symptoms
- Onset of vomiting <1 week or >6 months of age
- Vomiting increasing or persisting beyond 12-18 months of age
- Lethargy or fever
- Excessive irritability
- Weight loss or faltering growth
- Feeding problems or oral aversion
- Respiratory symptoms (aspiration, chronic cough, wheezing, recurrent pneumonia)
Neurological signs/symptoms
- Seizures
- Micro- or macrocephaly
- Developmental delay
- Nocturnal vomiting: may suggest increased ICP
Gastrointestinal signs/symptoms
- Bilious vomiting and/or abdominal rigidity/distension: may indicate intestinal obstruction
- Forceful vomiting: may indicate pyloric stenosis
- Haematemesis: may indicate potentially severe upper GI bleed
- Chronic diarrhoea and rectal bleeding: can be seen in a variety of conditions, particularly bacterial infections, acute surgical causes, IBD, CMPA
- Hepato(spleno)megaly: can be present in a variety of conditions including metabolic disorders
Differential diagnoses include but are not limited to anatomical malformations or underlying gastrointestinal, neurological, metabolic, cardiac, pulmonary pathologies
Management
Investigations
Investigations for GORD are rarely indicated, and there is insufficient evidence to support the routine use of these modalities for a primary diagnosis of GORD.
Investigations such as barium contrast studies, pH-impedance monitoring, upper gastrointestinal endoscopy may be considered on an individual basis after the patient has been assessed by a paediatrician/paediatric gastroenterologist
Treatment
GOR
Physiological GOR does not require investigation or treatment
Suspected GORD flowchart
The steps of this flowchart provide an approach to escalation of treatment and should be used whilst considering severity of symptoms and response to treatment
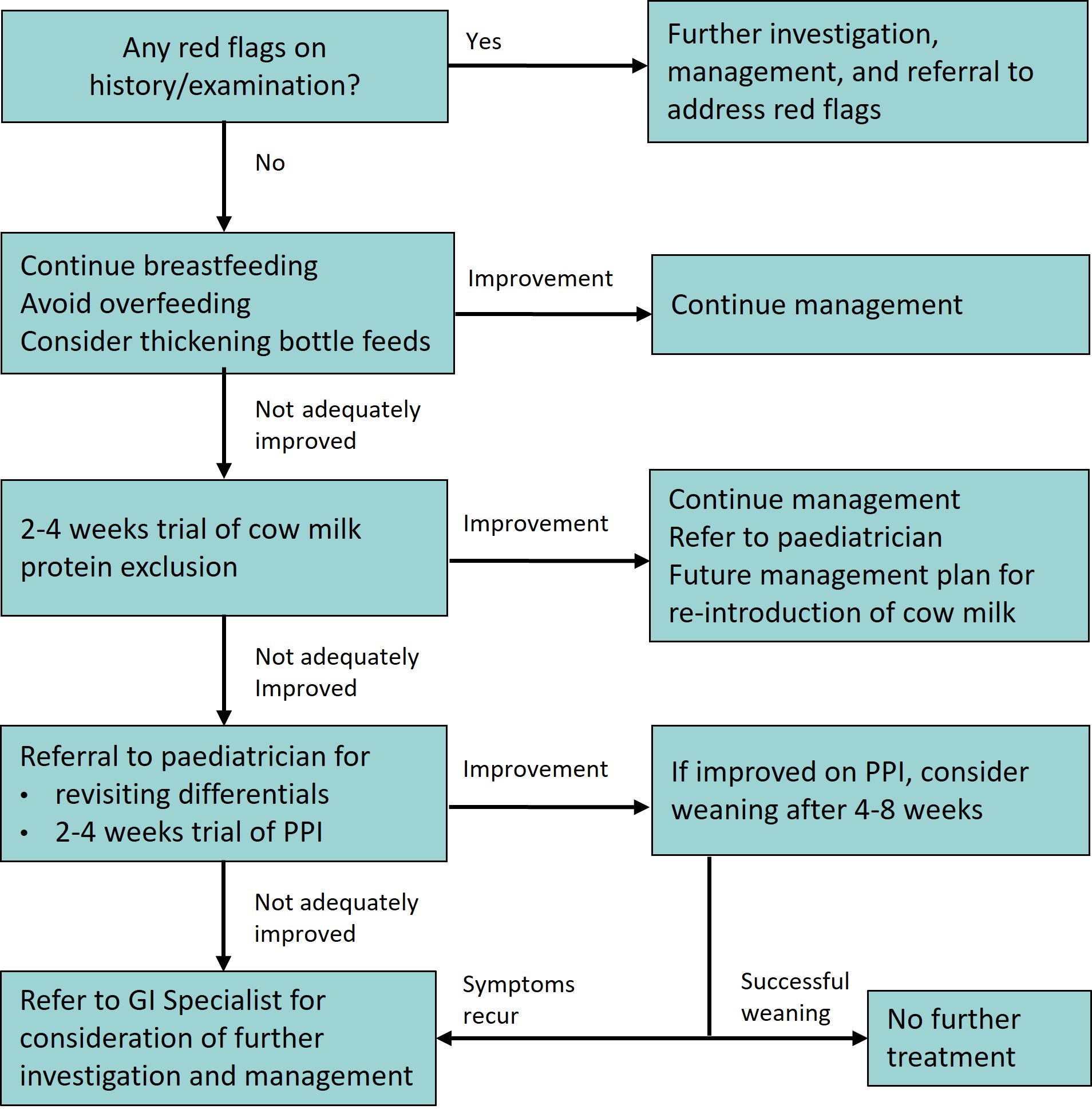
General measures
Positioning
- Holding the infant in a head elevated position for 20–30 minutes after feeding may reduce GOR
- Do not recommend prone/side sleeping or inclining the sleep surface due to the risk of SIDS
Thickened feeds
- Continue direct breast feeding. The benefit of thickening feeds is only modest, and the burden of expressing and bottle feeding is significant
- In bottle fed babies, thickened feeds may reduce frequency of vomiting
- There is no evidence of choosing one thickening agent over another
- "Anti-reflux" formulas are pre-thickened, or alternatively a thickening agent can be added to a standard formula or expressed breast milk. Note that breast milk should not be thickened with cereal-based thickeners given it is digested by amylases
in breast milk
- Thickened feeds may occasionally cause gastrointestinal symptoms such as abdominal pain and altered bowel habits, both diarrhoea and constipation have been reported
- Ensure the infant is not being given alginate product (Gaviscon Infant®) as co-administration may increase the risk of bowel obstruction
Optimise feeds
- Observation and assessment of feeds by an experienced clinician can be helpful
- Consider a trial of smaller, more frequent feeds
- If total feed volume is excessive for infant's weight, consider reducing feed volume.
- GOR alone is not an indication to change formula or stop breast feeding. There is no benefit of any brand of standard cow milk formula over another, nor do they vary in their content of dairy
Complementary treatments
- Complementary treatments such as prebiotics, probiotics or herbal medications are not recommended as a treatment for GOR or GORD
Specific measures for GORD
Consider cow milk protein exclusion
- Where CMPA is suspected, the infant should have a 2-4 week trial of strict cow milk protein elimination from their diet and referral to a paediatrician arranged
- Breast fed infants require strict maternal cow milk protein avoidance
- Formula fed infants require specialised formula
- See ASCIA milk substitutes in CMPA for up-to-date list of formulas available in Australia
Consider pharmacological management for GORD
Acid suppression therapy
- 1st line proton pump inhibitor (PPI), eg omeprazole or lansoprazole - as a 2-4 week trial
- It is important to review need for ongoing therapy
- If clinical benefit seen continue for 4-8 weeks then consider weaning
- Studies have indicated that PPI therapy may lead to increased risk of community acquired pneumonia, gastroenteritis, future fractures and micronutrient deficiencies
- There is no evidence to support empiric use of PPI as a diagnostic trial for irritable infants
Surface agent
- Alginate product (Gaviscon Infant®) increases viscosity of gastric contents and there is evidence suggesting may reduce episodes of visible regurgitation, limited evidence regarding effectiveness
- Long-term use in infants is not recommended
Prokinetic agents
- Only under specialist direction, may be considered prior to surgery in patients where other pharmacological treatment has failed
Surgical treatment
Surgical approaches eg fundoplication are reserved for children who have intractable GORD symptoms unresponsive to optimal medical therapy or with significant complications
Consider consultation with local paediatric team when
- Red flag features present
- GORD not responding to initial management
Consider transfer when
Child requires care beyond the comfort level of the hospital
For emergency advice and paediatric or neonatal ICU transfers, see Retrieval Services
Consider discharge when
- GOR and GORD can almost always be managed as an outpatient
- Ensure caregiver has adequate support and appropriate parent handouts provided
- Timely follow-up to assess effectiveness of interventions and therapy is arranged
Parent information
*Last updated April 2026