Introduction
Chest drains also known as
under water sealed drains (UWSD) are a drainage system of three chambers
consisting of a water seal, suction control and drainage collection chamber.
UWSD are designed to allow air or fluid to be removed from the pleural cavity, while
also preventing backflow of air or fluid into the pleural space. This allows
for the expansion of the lungs and restoration of negative pressure in the
thoracic cavity. Appropriate chest drain management is required to maintain
respiratory function and haemodynamic stability. Chest drains may be placed
routinely in theatre, PICU and NICU; or in the emergency department and ward
areas in emergency situations. Some patients will have Redivac drains inserted,
these are different from a UWSD. Please refer to Pleural and Mediastinal Drain Management
after Cardiothoracic Surgery guideline.
Aim
To provide a clear guide for nursing staff to promote the safe, correct and competent management of the UWSD in the ward setting. This clinical guideline
is written from the perspective of a cardiac and renal ward management;
however, it also outlines management from the perspective of other speciality
areas where care may differ.
Definition of terms
- Chylothorax: Collection of lymph fluid in the pleural space
- Haemothorax: Collection of blood in the pleural space
- Pleural
effusion: Exudate or transudate in the
pleural space
- Pneumothorax: Collection of air in the pleural space
- Tension Pneumothorax: Air builds up in the pleural space and forces a mediastinal shift leading to decreased venous return to the heart and lung collapse/compression causing acute life-threatening respiratory and cardiovascular compromise.
Indications for Insertion of a Chest Drain
- Chylothorax
- Pleural effusions
- Pneumothorax
- Post cardiac surgery
- Haemothorax
Insertion of a Chest Drain
Please see the Chest Drain Insertion CPG below:
RCH access only:
See Aseptic Technique Policy and Procedure
Chest Drain Assessment & Management
Start of shift checks
-
Ensure
that there is emergency equipment at bedside including:
- At least
two drain clamps per drain (For use in emergency only)
- Two
suction outlets - x1 chest drain and x1 for airway management
- Auscultate
the chest
- Assess
the chest tube and system tubing (i.e. for kinks, dislodgement etc) as well as
the drain dressing to ensure it is intact and for any signs of infection
- Check
that the drain is anchored appropriately
- Labelling
of each drain tube in accordance with EMR documentation (See
image below)
- Drain is on suction (i.e Red bellow out) and
that the amount of suction correlates with the medical team order on EMR (See
image below for labelling of each chamber)
- Assess
for any leakages or movement in water chamber
- Check
that the drain in not clamped (unless ordered by medical staff).
- Significant
risk of tension pneumothorax development if clamped

UWSD Labelling
It is imperative that the UWSD is labelled in a way that is clear and
visible. This is extremely important when removing the drain to ensure the
correct drain is removed. Please refer to the image below for the correct
labelling of an UWSD. The criteria for correct labelling includes the
following:
- How - Clear, visible writing (Dark
font and capital letters) on a label that can be complete stuck down
- What – Include the position (e.g.
Pleural, mediastinal etc) and side (e.g. right, left)
- Where – Top of the USWD & avoid
covering any measurements / numbers
- Who & when – Labelling
should be completed by the Cardiac theatre nurses / surgeons post operatively prior to transfer
of the patient back to the ward. Should a UWSD require changing post
operatively on the ward, the responsibility of labelling lies with the direct
care giver (e.g. Nurse changing the UWSD or bedside nurse).

Patient Assessment
Vital signs
- Auscultate chest at shift commencement
- Routine four hourly observations including
assessment of respiratory effort
- If the
patient is on an opioid infusion continuous monitoring is required and hourly
cardiorespiratory observations (HR, SpO2, BP, RR) should be documented
For ward areas
- On insertion of chest drain monitor and
document on EMR flowsheets patient observations (HR, SpO2, BP, RR, respiratory
effort and temperature):
- 15
minutely for 1 hour
- 1 hourly
for 4 hours then 1-4 hourly as indicated by patient condition
Drain insertion site and dressing assessment:
- Check that the dressing is clean and intact
- Assess for any ooze, bleeding or signs of
infection/inflammation every hour and document this within EMR:
- Small
amounts of ooze can be a normal presentation post operatively, however if any
abnormal presentations are observed: Notify the medical team, consider taking
and sending swabs of the site and take a clinical photo and
upload onto EMR
- Observe that the sutures remain intact and
secure (particularly long term drains where sutures may erode over time)
Skin integrity:
- Assess skin at a minimum four hourly for pressure
injuries particularly where the tubing is in contact with the skin. Effective
anchoring below the insertion sites will assist with preventing this.
UWSD Unit and Tubing
- Ensure all connections between chest tubes
and drainage unit are tight and secure
- Assessment of chest tube and system tubing
should occur at the beginning of the shift and every hour throughout the shift.
Tubing should have no kinks or obstructions that may inhibit drainage
- Never lift drain above chest level. The unit
and all tubing should be below patient’s chest level to facilitate drainage.
Ensure the unit is securely positioned on its stand or hanging on the bed
- Drain tubing should always be secured to
patient bed to prevent accidental removal and anchored to the patient’s skin to
prevent pulling of the drain (See image below)
- Ensure the water seal is maintained at 2 cm
at all times
Pain
- Ensure that patients with an UWSD have
appropriate and regular pain relief (IV opioid infusion, PCA etc). A CPMS
referral should also be in place and also consider appropriate administration
of pain relief prior to mobilisation, physiotherapy sessions or other
activities that involve movement etc
- Pain assessment should be conducted and
documented four hourly unless more frequently warranted
Suction
- Ensure that the suction is on and ensure that
the “red bellow” is all the way out
- If suction is required orders should be
written by medical staff and documented within the “Orders” tab on EMR. Suction
on the drainage unit should be set to the prescribed level, please see below. Suction
is not always required as it may lead to tissue trauma and prolongation of an
air leak in some patients.
- -5 cmH20 is commonly used for neonates
- -10 cmH20 to -20 cmH20 is usually used for
children
Drainage
- Every hour, the UWSD tubing should be “tilted
and tipped” in order to ensure the fluid within the tubing accumulates within
the chamber
- Milking
of chest drains using roller clamps is only to be done with written orders from
medical staff. Milking drains creates a high negative pressure that can cause
pain, tissue trauma and bleeding
Volume
Document
hourly the amount of fluid in the drainage chamber (for each drain if multiple
present) in the Fluid Balance flowsheet on EMR
Assess the cumulative total of drainage
output and notify medical staff of the following:
- A sudden increase in amount of drainage
- Greater than 5mls/kg in 1 hour
- Greater than 3mls/kg consistently for 3 hours
- Significantly reduced output over an extended
length of time or if a drain with ongoing loss suddenly stops draining
- Blocked drains are a major concern for
cardiac surgical patients due to the risk of cardiac tamponade
If the
chamber tips over and blood has spilt into next chamber, simply tip the chamber
up to allow blood to flow to original chamber
Colour and Consistency
Colour
and consistency of drainage should be documented hourly along with
documentation of volume amounts. If
there is a change (eg. Haemoserous, bright red, serous, chylous/creamy) notify
medical staff immediately
Air Leak (bubbling)
- The water seal chamber should be assessed
every hour for any potential air leaks. An air leak will be characterised by
intermittent bubbling in the water seal chamber when the patient with a
pneumothorax exhales or coughs.
- The
severity of the leak will be indicated by numerical grading on the UWSD
(1-small leak 5-large leak)
- Continuous
bubbling of this chamber indicates large air leak between the drain and the
patient. Check drain for disconnection, dislodgement and loose connection, and
assess patient condition. Notify medical staff immediately if problem cannot be
remedied.
- If suspected or confirmed leakage, clamp
drain tubing closest to patient and escalate accordingly and document on Fluid
Balance Flowsheet on EMR
Oscillation (Swing)
- The water in the water seal chamber will rise
and fall (swing) with respirations. This will diminish as the pneumothorax
resolves. Assess and document on Fluid Balance Flowsheet on EMR
Other Considerations
- Referral to a physiotherapist should be made to enhance chest movement and prevent a chest infection and mobilisation and transferring should be encourage as appropriate where possible
- Parent education on managing potential accidental dislodgement should be discussed
Patient Positioning
- Patients who are ambulant post operatively will usually have fewer complications and shorter lengths of stay. If a patient is on strict bed rest or is an infant, regular changes in position should be encouraged to promote drainage, unless the patient’s clinical condition prevents doing so
Patient Transport
- If the patient needs to be transferred to another department or is ambulant, the suction should be disconnected and left open to air
- Remember that during transport, the tubing should not be clamped and that the UWSD should remain below chest level
- Clamps must not be used on the patient for transport because of the risk of tension pneumothorax
- When transporting the patient, be weary of tubing getting caught in the bed and utilise a “cart/trolley” where possible for ease of transport especially for multiple drains. Remember to remove anchor from bed before mobilising the patient.
Specimen Collection
Collect drainage specimens for culture through the needless sampling
port located by the in-line connector.
Equipment Required
- Specimen container
- Alcohol swab
- 10ml syringe
- Dressing pack
- Gloves
- Eye Protection
Procedure:
1. Wait for the fluid to collect in a loop of
the tubing
2. Perform hand hygiene, then don gloves &
eye protection
3. Clean the sampling port ( See feature
labelled as 1 in the image below) with an alcohol wipe and leave to dry for 20
seconds
4. Temporarily clamp the tubing above where the
fluid has collected
5. Connect a 10ml Luer lock syringe to the
sampling port and aspirate the fluid out of the tubing. Do not pierce tubing/sampling
port
6. Place fluid in sterile specimen container
7. Once the syringe is disconnected remove all
clamps and kinks
8. Perform hand hygiene
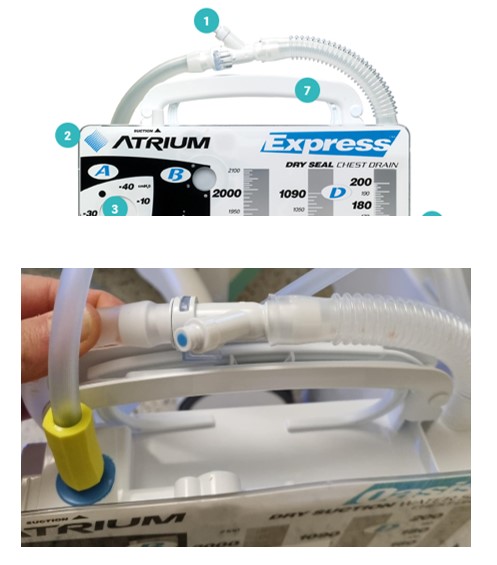
Chest Drain Dressings
Dressing Change
- Dressings should be changed:
- Every seven days unless otherwise indicated
- If they are no longer dry and intact, or signs of infection
- Infected drain sites require daily changing, or when wet or soiled
- Changes are a risk for accidental drain removal. Avoid unnecessary changes
- Dressings should ensure drain is secure
- Dressings should allow site visibility and prevent pressure on skin
Equipment Required
- Dressing pack
- Chlorhexidine solution (Yellow or blue)
- Gloves
- Two small occlusive tegaderm dressings
- Split gauze
Procedure:
1. Perform hand hygiene and then don gloves
2. Remove old dressing
- Preferably get someone who is not sterile to
don latex gloves and remove the dressing
3. Clean the drain site using the appropriate
chlorhexidine solution:
- Use standard aseptic technique with body
temperature sterile normal saline
- If the wound is showing signs of being
infected, contaminated or soiled use the yellow solution (Aqueous
Chlorhexidine 0.15% w/v cetrimide 15%)
4. Once the
site is dry apply two layers of split gauze in the direction where the split
facing up and it wraps around the drain. Another two layers of split gauze
should then be placed on top of the first layer of gauze in the opposite
direction (split facing down).
5. Cover gauze using hypafix TM (approx
two pieces, enough to cover the gauze completely)
6. Remove gloves and perform hand hygiene
For cardiac surgical patients with
drains inserted intraoperatively: Ensure dressing does not communicate with sternotomy dressing or wound
Anchoring
drain tubing
- Apply ComfeelTM or similar to
protect fragile skin from 'tag' of tape
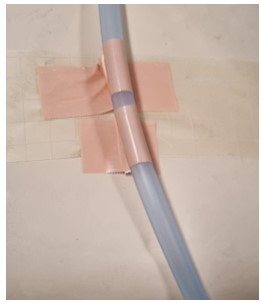
- Use “sleek” TM or “hypafix” TM
to secure the drain tube (see image below). When securing and folding the sleek
around the tubing, ensure that the tubing isn’t secured flat down and that
there is a “gap of tape” between the comfeel TM and tubing
Removal of Dressings
- To remove dressing when placed flat against
the skin - Lift corner from the skin and slowly stretch the in dressing in a
motion that is parallel to the skin
- To remove semi permeable dressing placed in a
sandwich position
- Hold the corners of the dressing on either
side of the drain and pull them away from each other; this should create a
pocket around the drain
- Peel each of the dressings away from each
other until you reach patient skin
- Slowly stretch the rest of the pressing in a
motion that is parallel to the patient’s skin to remove the rest of the
dressing.
Changing the Chamber
Indications
- The chest drain chamber needs to be replaced
when it is ¾ full or when the UWSD system sterility has been compromised e.g.
accidental disconnection.
Equipment Required
- New UWSD
- Dressing pack
- Gloves
- Eye Protection
Procedure
1. Perform hand hygiene
2. Use personal protective equipment to protect
from possible body fluid exposure
3. Using an aseptic technique, remove the unit
from packaging and place adjacent to old chamber
4. Prepare the new UWSD as per manufacturer’s
directions supplied with drain
5. Ensure patients drain is clamped to prevent
air being sucked back into chest
6. Disconnect old chamber by holding down the
clip on the in-line connector to pull the tubing away from the chamber.
7. Insert the tubing into the new chamber until
you hear it click.
8. Unclamp the chest drain
9. Check drain is back on suction
10. Place
old chamber into yellow infectious waste bag and tie
11. Perform
hand hygiene
Removal of Chest Drains
Important considerations for drain removal
- There
must be written documentation for drain removal by medical staff in EMR
specifying which drain/s are to be removed
- The
responsibility of the proceduralist removing drains is to check the patient’s
post-operative x-ray prior to drain removal
- Chest X ray Must be checked by the proceduralist before
any chest drain removal and after removal. The X ray is then reviewed by
surgical team to follow up if further management is required.
- Drain
labelling must be physically checked by proceduralist prior to removal to
ensure removal of correct drain/s. Consult cardiac surgeon for further
clarification.
Indications
- Drainage diminishes to little or nothing
- Absence of an air leak (pneumothorax)
- No evidence of respiratory compromise
- Chest x-ray showing lung re-expansion
Equipment required
- Dressing trolley with Yellow Infectious waste
bag attached
- Dressing pack (sterile towel, sterile gauze)
- Sterile Gloves
- Appropriate skin cleaning solution for
procedure
- Neonates <1500 grams -
Chlorhexidine irrigation solution 0.1% (Blue Solution)
- For all other patients - Aqueous
Chlorhexidine 0.15% w/v cetrimide 15% (Yellow Solution)
- Steristrips
- Suture Cutter
- Band Aids
- Clamps
- Eye Protection
- Occlusive dressing
- Sharps container
Patient and pre-procedure preparation
- Ensure patient is fasted, has been
administered adequate and age-appropriate pain control, sedation (fast
appropriately) and distraction therapy (see Procedural Pain Management Guideline)
- Consider environment e.g. treatment room or
privacy screens if in ward area and the involvement of Child Life Therapy if
required
- Ensure
you have enough staff to assist with the procedure & ensure that the
patient is monitored throughout the procedure
- Heparin
infusions for cardiac patients should not be discontinued prior to drain
removal
- Always
remove pacing wires (cardiac patients) before removing the drains and ensure
that the drains are unclamped during the removal of wires
Procedure
1. Perform hand hygiene
2. Opening dressing pack and add sterile equipment
and 0.9% saline
3. Don disposable gloves
4. Remove all dressings around the area
5. Clamp drain tubing and ensure suction is
disconnected – double check with assisting nurse. If there are multiple drains
in-situ, clamp all drains before removal. Once the required drains are removed,
unclamp remaining drains
6. Remove disposable gloves, perform hand
hygiene and don sterile gloves
7. Place sterile towel under tubes
8. Clean around catheter insertion site and
1-2cm of the tubing with age appropriate skin cleaning solution
9. If purse string present (cardiac patients)
unwind in preparation for assistant to tie
10. Remove
suture securing drain (ensuring purse string suture not cut)
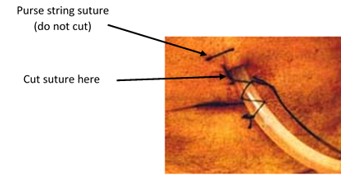
11. Instruct patient to exhale and hold if they
are old enough to cooperate; if not, time removal with exhalation
12. Pinching the edges of the skin together,
remove the drain using smooth, but fast, continuous traction
13. The assistant pulls purse string suture
closed as soon as the drain is removed, tying 2 knots and ensuring the suture
is not pulled too tight. Cut tails of suture about 2cm from knot
14. If there is no purse string present remove
drain and quickly seal hole with occlusive dressing (i.e. TegadermTM)
15. Apply steristrips over insertion site if
needed
16. Remove and discard equipment into a yellow
infectious waste bag and tie
17. Perform hand hygiene
Post Procedure Care
- Attend to patients comfort and sedation score
as per procedural sedation guideline
- CXR should be performed post drain removal,
ideally 2 hours post (max 4 hours)
- Patients in PICU may wait until routine daily
CXR if clinically well
- Clinical status is the best indicator of re-accumulation
of air or fluid. CXR should be performed if patient condition deteriorates
- Monitor vital signs closely (HR, SpO2, RR,
Respiratory effort and BP) on removal and then every hour for 4 hours post
removal, and then as per clinical condition
- Document the removal of drain in the LDA
flowsheet in EMR
- Remove sutures four days post drain removal
- Dressing to remain in situ for 24 hours post
removal unless contaminated
Complications and Troubleshooting
- Pneumothorax - Signs
and symptoms include:
- Decreased
SpO2, increased respiratory effort , diminished breath sounds, decreased chest
movement, complaints of chest pain, tachycardia or bradycardia, hypotension
- Notify
medical staff & request an urgent CXR
- Prepare
for insertion/repositioning of chest drain
- Ensure
drain system is intact with no leaks, or blockages such as kinks or clamps
Bleeding at the drain site
- Don gloves
- Apply pressure to insertion site
- Place occlusive dressing over site
- Notify medical staff
- Check Coagulation results
- Check drain chamber to ensure no excessive
blood loss
Infection of insertion site
- Notify medical staff
- Swab wound site
- Consider blood cultures
Accidental disconnection of system
- Clamp the drain tubing at the patient end.
Clean ends of drain and reconnect. Ensure all connections are cable tied. If a
new drainage system is needed cover the exposed patient end of the drain with
sterile dressing while new drain is setup. Ensure clamp is undone when problem
has resolved.
- Check vital signs and consider getting a CXR
- Alert medical staff
Accidental drain removal
- Apply pressure to the exit site and seal with
steristrips. Place an occlusive dressing over the top
- Check vital signs, consider the need for a
CXR and alert medical staff
- The incident must be documented in the VHIMS by the nurse attending to
procedure
Purse string cut or not present
- Small bore drains such as pigtails do not
require purse strings. Simply apply an occlusive dressing.
- For large bore drains:
- Pinch or
apply pressure to the exit site
- Apply
steristrips to close exit site and cover with an occlusive dressing
- Notify
the responsible medical team to review patient and consider need for a suture
- The
incident must be documented in the VHIMS by the nurse delegated to remove the
drain.
Unable to remove chest drain
- If the drain is unable to be removed with
reasonable traction being applied, notify the responsible surgical team
- If unsafe to be removed on the ward, the
patient might have to go to theatre and have it removed under general
anaesthetic
Retained drain during removal
- If the tube fractures during drain removal
and remnants of the tubing are left within the patient contact the treating
team immediately (Initiate MET call as needed or if patient becomes unstable).
- An urgent chest x-ray should be conducted.
- The patient should be prepared for theatre
e.g. keep fasted
- The whole drain unit should be kept in the
patient’s room until surgical review and will need to be kept for collection to
enable quality review.
- The piece of drain tubing that remains in the
patient will also be kept once surgically removed to allow for appropriate
follow up of the incident’s cause.
- The incident must be documented in the VHIMS by the nurse delegated to remove the
drain.
- Please refer to Surgical Drains (Non Cardiac)
guideline & RCH procedure for Missing or Non-Intact Drains
Family Centred Care
- Explain purpose of chest drain to family and when it is likely to be removed
- Discuss the need for pain relief for the child to be comfortable enough to move and participate in physiotherapy
- Encourage parental involvement with mobilising, sitting out of bed and assisting with chest physiotherapy to aid faster recovery.
- Multidisciplinary care e.g. Physiotherapy referral
Companion Documents
Evidence Table
Please remember to
read the disclaimer
The development of this nursing guideline was coordinated by Charmaine Russell, CNS, Koala, and Emily Mohd Faizal, RN, Koala, and approved by the Nursing Clinical Effectiveness Committee. Updated October 2022.