Table of contents will be automatically generated here...
Introduction
- Differences in the proportions of a child's head and skeleton affect outcome in paediatric "maxfax" injury. The relative prominence of the child's cranium, compared to mid-face and mandible, together with the elasticity of the immature facial skeleton, account for the low incidence of facial fractures in
children. However, soft tissue injuries are common.
- Soft tissue injury patterns include burn injury, electrical injury, and lacerations.
- Falls are the most common cause of facial trauma in the paediatric group, followed by blunt trauma from sports activities, motor vehicle accidents and assaults. Non-accidental trauma may also need to be considered.
- Patterns of injury that may lead one to suspect child abuse include multiple bruises in various stages of healing.
- Maxillofacial injuries are commonly associated with cervical spine and intracranial injury.
- Emergency evaluation of a facial trauma patient should always begin with attention to the ABCs. In general, facial injuries rarely require emergency management.
In all aspects of trauma management,
the primary survey is the first priority
Primary survey
The secondary survey should include visual acuity
testing (even in the presence of marked periorbital
swelling).
Adequate exposure is imperative to facilitate a thorough examination.
Airway
Airway assessment is of primary
importance in evaluating facial injuries.
- If no cervical spine injury is suspected, attempts to open the airway may be made carefully with the head tilt/ chin lift manoeuvre. Avoid overextension of the airway by placing the patient in the neutral position for infants or sniffing position for children.
- In cases in which cervical spine injury is suspected, the jaw thrust manoeuvre is preferred. (From Advanced Paediatric Life Support, The Practical Approach, 3rd edition, BMJ Books, 2001, pg. 23-24.)
- Blood, vomitus, tooth fragments and foreign bodies may obstruct the airway, and clearance of the upper aerodigestive tract of all debris is a priority.
- Special anatomic considerations of the pediatric airway that can contribute to airway obstruction include: (From Kaban, Troulis. Pediatric Oral and Maxillofacial Surgery, Saunders, 2004, pg. 86).
- Lymphoid hypertrophy/ enlargement of the tonsils and adenoids between the ages of 4 and 10.
- Relative macroglossia, with the tongue positioned higher in the oral cavity.
- A softer and floppier epiglottis may complicate pediatric endotracheal intubation.
- Tongue-displacement secondary to comminuted anterior mandibular fractures may also compromise the airway.
- Bleeding may be profuse (and occult) from scalp lacerations and fractures of the mid-face.
- Control of bleeding by local pressure and, if required, scalp sutures or staples as well as temporary reduction of fractures may be indicated immediately.
- Concurrently, the cervical spine must be stabilized and protected until further assessment for cervical spinal injury is undertaken.
- A quick method for determining the proper size endotracheal tube includes adding 16 to the child's age in years, and dividing by 4. Ie., the proper sized tube for a 4 year old child would be (16+4)/4 =5mm (internal diameter)
- Fiberoptic intubation may be necessary to control the airway of the pediatric trauma patient.
Trauma x-rays
A chest x-ray to exclude aspiration of dental fragments or foreign bodies may be indicated.
Secondary survey
A detailed craniomaxillofacial examination should be performed during the secondary survey, after initial stabilization of the patient.
Open wounds should be covered with moist, clean dressings and tetanus prophylaxis administered if required.
Management
While facial injuries in children are rarely fatal, they may have significant functional and cosmetic sequelae. Paediatric mortality in trauma is usually secondary to airway compromise or associated neurological injuries. Consultation with a Maxillo-facial Service should be arranged early in
the evaluation of patients with facial injuries.
The principles of managing paediatric facial trauma are the same as for adults. However, there are anatomical differences that influence the approach to treatment.
Factors to consider in the paediatric maxillofacial skeleton:
- The maxillofacial skeleton is growing, and the cancellous space is proportionally larger than in the adult.
- The maxillo-mandibular complex is proportionately smaller in relation to the cranium
- The maxillary and paranasal sinuses are less developed.
- The mandibular condylar neck is shorter, and the articular surface is broader.
- Temporomandibular joints are active growth centers.
- The jaws contain the developing teeth.
- Permanent tooth buds are located close to apices of primary teeth.
- The overlying soft tissues are thicker than in the adult.
Nasal fractures
Isolated nasal fractures are the most commonly seen fractures in facial trauma. However, nasal injuries may be associated with severe mid-facial trauma involving the naso-orbito-ethmoidal (NOE) complex, the frontal sinuses and the orbito-zygomatic complex.
Nasal bones should be X-rayed when:
- There is swelling and deformity of the nasal dorsum, epistaxis and periorbital ecchymosis;
- There is nasal obstruction;
- There is septal deviation due to fracture of the cartilaginous septum.
- Isolated nasal fracture is treated clinically and X-Rays are not normally necessary.
Note:
- A septal haematoma is uncommon, but requires early drainage to avoid necrosis of septal cartilage.
- In NOE fractures there is depression of the nasal radix and telecanthus with posterior "telescoping" of the complex.
- CSF rhinorrhoea may be present if the fractures of the NOE complex involve the base of the skull and a dural breach.
- Crepitus may not be palpable as the immature nasal complex has greater elasticity.
Investigations:
Radiographs:
- Lateral nasal projection
- Waters' view 30 degrees.
However, interpretation of nasal fractures on plain films is difficult due to complex sutural anatomy and cartilaginous components. The need for treatment of an isolated nasal fracture is usually based on clinical evaluation, and X-rays are not considered
routine unless suspicion of other facial injuries exists
- If NOE complex injury is suspected, a CT scan with both axial and coronal views is required. In addition, 3-D CT reconstructions may be indicated.
Treatment:
- Reduction of nasal bones and straightening of the septum should take place at 5-7 days post-injury.
- Support of the reduced nasal bones is often provided by intranasal packing and an external nasal splint.
Note:
- The most common complication is obstruction of the nasal airway caused by undiagnosed or untreated deviation of the septum.
- There is no evidence that mid-facial growth-deficiency occurs after a nasal fracture in childhood.
Zygomatico-maxillary complex fractures (ZMC)
ZMC fractures in children are usually greenstick fractures, and can be managed conservatively. However, when there is marked displacement of the orbital rim, zygomatic prominence and/or arch, open reduction - with or without internal fixation - is indicated.
Clinical Features:
- Periorbital swelling, ecchymosis;
- Subconjunctival hemorrhage with no lateral posterior limit;
- Diplopia secondary to extraocular muscle dysfunction ;
- Enophthalmos;
- Loss and flattening of the zygomatic body prominence;
- Epistaxis;
- Paraesthesia of the infraorbital nerve distribution (cheek, lateral nose, upper lip, upper anterior teeth and gingiva);
- Trismus (limited mouth-opening) due to impingement on the coronoid process of the mandible;
- Tenderness and diastasis at the fronto-zygomatic suture;
- Palpable depression of the infraorbital rim and zygomatic arch;
The development of proptosis of the
globe, reduced or lost vision and severe orbital pain, are features
of retrobulbar haemorrhage. This is an emergency with the potential
for permanent blindness, and requires urgent surgical intervention.
If a retrobulbar haemorrhage is suspected, a facial trauma surgeon
and an ophthalmologist should be contacted immediately, and the
child kept fasted in preparation for surgery.
Investigations:
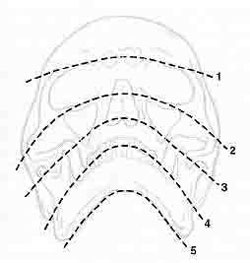
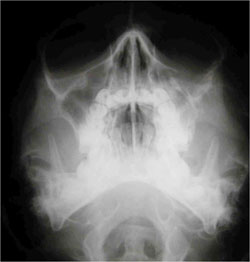
- Radiographs -Waters' sinus (occipitomental) views 150, 300 (fig. 1) -Submental-vertex view.
- CT scans of the orbits and mid-face with fine-cut axial and coronal views;
- 3-D CT reconstructions, if available, give an additional appreciation of the injury.
Fig 1: Campbell's and Trapnell's lines to guide the survey of an occipitomental x-ray
Treatment:
- Early review by Ophthalmology, if there is difficulty in performing an adequate eye examination or if an injury to the globe is suspected.
- Conservative management of non-displaced fractures: avoidance of nose-blowing, antibiotic prophylaxis and a nasal decongestant.
- Reduction of displaced fractures if there is appreciable contour deformity or functional impairment. Open approaches are performed for fracture reduction, with or without the use of internal fixation. Exploration and reconstruction of the orbital floor may also be necessary.
Isolated orbital fractures
Orbital fractures may present as either:
- an orbital rim disruption, with extension of the fracture on to the orbital floor; or
- an isolated localized fracture of the orbital floor - the "blow-out" fracture. The medial wall of the orbit is often concomitantly involved. It is frequently caused by a direct frontal blow from a round blunt object, such as a squash or tennis ball,
baseball or fist.
- Associated globe injuries must be excluded by early ophthalmological assessment, as eye injuries may occur in over 50% of these fractures.
Clinical features:
- Symptoms and signs are essentially the same as those noted with orbital involvement of zygomatic complex fractures (fig. 2). In addition, the signs and symptoms of a retrobulbar haemorrhage should be examined (see above, section). Particular attention is
required to assess the presence of enophthalmos and muscle entrapment.
- Patients with entrapment due to 'trap-door' type fractures of the orbital floor, may also have significant concomitant nausea and/ or vomiting, bradycardia or hypotension. These symptoms usually resolve promptly following surgical repair.
Fig 2: A 4 year old child with right orbital 'blow out' fracture associated with entrapment

Investigations:
- Radiographs- Waters' sinus views 30, 45 degrees (The classic "tear drop" sign may be present if the orbital soft tissues have herniated through the floor into the maxillary antrum)
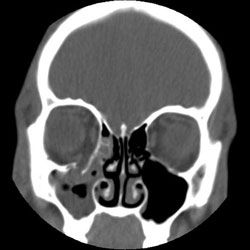
- A CT scan with fine-cut axial and coronal views, provides the best radiological assessment of orbital wall fractures (fig.3)
Fig 3: Isolated right orbital floor fracture
Treatment:
- Large orbital floor defects, resulting in ocular muscle entrapment and/or significant enophthalmos, are indications for surgical management.
- Exploration of the orbit is usually performed at 5-7 days post-injury, following the resolution of swelling and oedema. The prolapsed periorbital soft tissue is reduced and the bony defect repaired with an autogenous bone graft or alloplastic material.
- Patients with symptoms of the oculocardic reflex (nausea, bradycardia and Hypotension) should undergo immediate surgery for exploration of the orbital floor
- Early surgery may be indicated if the injury can be well characterized and/or if the patient is undergoing surgery for other injuries.
Maxillary fractures
Maxillary fractures are uncommon in childhood. The maxillae are proportionately smaller and denser than in adults, with a relative lack of sinus development. Consequently, isolated displacement of part or all of the maxillary complex is rare.
When fractures do occur, however, they are generally a component of more extensive craniofacial injuries. Approximately 40% of children with mid-facial fractures have associated skull fractures, and CSF rhinorrhoea may also be present. There is also a high incidence of
cervical spine injuries in patients with severe mid-facial fractures. The cervical spine must be stabilized until a cervical spine injury can be excluded.
Clinical features:
- Bilateral periorbital swelling and ecchymoses.
- Bilateral sub-conjunctival hemorrhage.
- Facial deformity: asymmetry, facial flattening or elongation may be apparent in older children.
- Infraorbital paraesthesia.
- Palpable steps of the infraorbital margins and tenderness at the fronto-zygomatic sutures
- Mobility of the maxilla at different levels, usually representing 3 recognizable patterns of fracture (Le Fort I, II, III) (fig 4)
- Le Fort I - maxilla is mobile to the level of the base of the nose with a stable upper mid-face; ·
- Le Fort II - maxilla and nose are mobile as one unit, with movement detected medially at the infraorbital rims;
- Le Fort III (craniofacial dysjunction) - mobility of the complete mid-face, with movement detected at the frontonasal and frontozygomatic sutures.
- Midline palatal fractures may result in independent movement of the right and left maxillae, and are frequently associated with laceration of the palatal mucosa.
- Malocclusion (inability to bring teeth together in a normal "bite" position) may be difficult to assess in the presence of associated dento-alveolar injuries and poor cooperation, but may demonstrate an anterior open bite where the posterior teeth are
occluding with an inability to bring the anterior teeth together.
- CSF rhinorrhoea due to dural tear and fracture of the anterior cranial fossa
- Haemotympanum (blood in the middle ear) if there is a concomitant base of skull fracture.
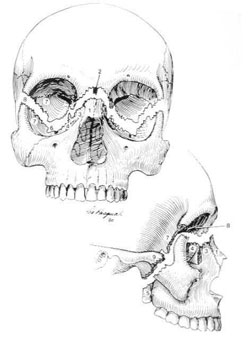
Fig 4: Le Fort fractures
Le Fort I
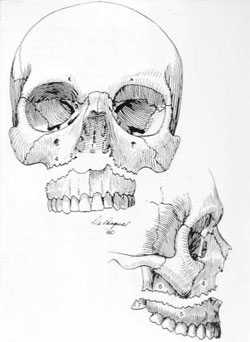
Le Fort II
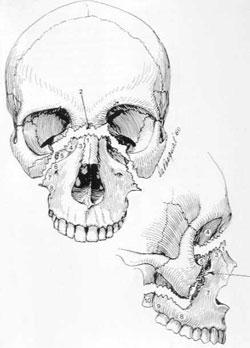
Le Fort III
Investigations:
- Radiology -Waters' views: 150, 300,450 (occipitomental views); -Poster-anterior and lateral skull views; -CT scan of the full facial complex, from vertex to clavicles, with axial and coronal views;
-3-D CT reconstruction if possible. - Assessment of paediatric head injuries often requires an early CT scan of the brain, plus review by the Neurosurgery Unit. Depending on the condition of the patient, this may be an ideal opportunity to continue the scan to include the facial complex(which is often overlooked).
- Examination by the Ophthalmology Unit of any mid-facial injuries, including injury of the orbital region.
- Analysis of any clear nasal discharge for beta 2 transferrin suggesting a CSF leak
- Imaging of mid-facial injuries may be difficult to interpret. It is not a substitute for a detailed clinical assessment whenever this is possible.
Treatment:
- Non-displaced, stable fractures with normal occlusion may be managed conservatively.
- Displaced or unstable fractures are reduced and stabilized to restore functional occlusion, facial contour and symmetry. Internal fixation may be indicated with trans-osseous wire fixation, mini-plate fixation, or the use of resorbable plate and screw
fixation. Intermaxillary fixation is not normally used today. Access to the facial bones may be via a coronal and/or intraoral approach. Incisions for orbital access are placed in the transconjunctival or subciliary skin creases.
- The presence of a persistent CSF rhinorrhoea indicates the need for exploration of the anterior cranial fossa followed by a dural repair.
Frontal bone fractures
Fractures of the frontal bone may occur:
- in association with extensive facial injuries; or
- in isolation, as a result of direct blunt trauma to the forehead in an MVA, sporting collision or assault.
Some frontal sinus fractures may be clinically obvious, with a depression or an open wound permitting direct visualization. In other cases, however, there may be no clinical signs.
A high degree of suspicion is therefore required, based on the presenting history and mechanism of injury.
Considerable force is required to
fracture the frontal bone and the patient should be maintained in
cervical spine precautions until an injury to the cervical spine is
excluded.
Clinical features:
- Soft tissue oedema over the frontal region, periorbital ecchymosis and oedema;
- Soft tissue contusions and/or lacerations over the frontal and glabellar regions.
- Complex injuries
- Oedema may preclude the palpation of underlying fractures of the anterior table of the frontal sinus
- Epistaxis or CSF rhinorrhoea may be present with nasal fractures and NOE .
Investigations:
- CT scan, with both brain and bony windows of cranium and orbits, axial and coronal views.
Treatment:
- Will be based on the assessment of the involvement of the anterior and posterior tables of the frontal sinus, and on the presence of persistent CSF leak.
- Non-displaced or minimally-displaced fractures of the anterior table can be managed conservatively; i.e. no nose blowing and antibiotic therapy.
- Displaced fractures of the anterior table require surgical management, with open reduction and internal fixation of the anterior table via a coronal approach.
- Displaced fractures of both the anterior and posterior table are managed in conjunction with the Neurosurgery Unit, and may necessitate a transcranial procedure to manage the posterior table fractures.
Mandibular fractures
Mandibular fractures occur in all age groups. Fractures of the condyle and subcondylar regions, are the most common due to trauma to the chin from falls.
Fig 5: Common sites of mandible fractures. (a) symphyseal / parasymphyseal, (b) body, (c) angle, (d) subcondylar, (e) condylar head
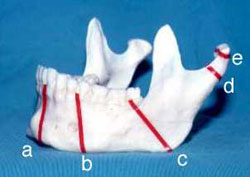
Clinical features:
- Pain and swelling over the fracture site.
- Restricted mouth opening.
- Gingival lacerations.
- Buccal and sub-lingual haematoma.
- Malocclusion - the inability to bring the teeth into a normal occlusion: -step in the occlusal plane (action of muscle attachments of fragments)
- wide displacement between teeth (often mistaken as an avulsed tooth) (fig 6)
- Mobile dento-osseous segments; (do not dismiss as just "loose teeth")
- Paraesthesia in distribution of inferior alveolar nerve (lower lip and chin)
- Bleeding from laceration of anterior wall of the external auditory canal due to a condylar injury
Fig 6: Avulsion of 2 lower incisors and a step in the occlusal plane associated with a mandibular symphyseal fracture
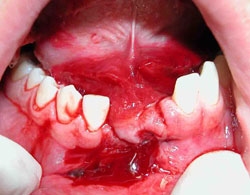
Investigations:
The mandible is ideally imaged in two planes -Orthopantomogram (OPG) -PA mandible (may require paramedian PA view) -Reverse Towne's view (for suspected condylar injuries)
In uncooperative patients, or patients unable to sit or stand for an OPG, right and left lateral oblique views of the mandible or a CT scan are imaged.
Fig 7: Right parasymphyseal and left angle mandibular fractures - (a) OPG (b) PA mandible
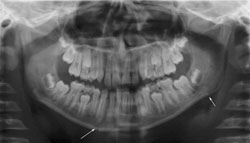
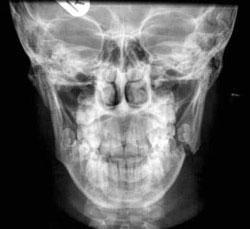
Treatment:
- Generally, early reduction and internal fixation is best for displaced or mobile fractures of the body and angles of the mandible. This helps gain early mandibular mobilization.
- Non-displaced stable fractures may be treated conservatively, with a soft diet and early mobilisation.
- Resorbable fixation is now considered a good option if available
Condylar fractures and temporo-mandibular joint
injuries:
Intra-articular injuries of the
condyle constitute the highest risk of growth disturbance and joint
hypomobility. Treatment should aim for continued normal jaw growth
to maintain symmetry and a balanced occlusion.
- The majority of condylar injuries are managed conservatively with soft diet and early mobilization. A short period of immobilization by intermaxillary fixation may be indicated in older children with bilateral fractures, malocclusion and persistent pain.
- Absolute indications for open reduction of condylar fractures include either central or lateral dislocation of the condylar head with subsequent mechanical blocking of normal movement.