Key
Points
- A patient with an apparently stable
airway, in the first few hours, may deteriorate quickly due to oedema. Even minor signs should still lead to very
careful observation.
- All patients with a neck injury who
require intubation should be considered to have a difficult airway. Immediate assistance from anaesthetic and ENT
specialists is strongly recommended.
Background
Traumatic neck injuries are rare in children due to their comparatively
short necks, and the relative protection afforded by the mandible and cervical
spine. However, the neck contains a
number of vital structures, that if injured can rapidly lead to a loss of life.
Neck trauma may be blunt, penetrating or a combination of both.
Penetrating neck injuries in the older child may include those from gunshot
wounds, stab wounds, or debris, such as glass or shrapnel, secondary to
experimentation with flammable/explosive materials. Younger children may sustain penetrating
injuries after falls onto objects in their environment (e.g. twigs, fence
posts) or held in their mouth (e.g. toothbrushes) or hands (e.g. pencils,
chopsticks). Blunt injuries tend to be
secondary to motor vehicle accidents, especially if unrestrained, or
motorcyclists (clothes-line or garrotting type injuries). Blunt injuries to the neck may also occur due
to non-accidental injury (strangulation) or hanging.
Patients
with neck trauma have commonly been involved in a multi-system trauma requiring
initial assessment following an ATLS protocol.
During the assessment of the neck, consider the four types of vital
structure in the neck.
- Airway – consists of
pharynx, larynx, trachea and lungs
- Vascular structures
- Arteries - carotid arteries, vertebral arteries, brachiocephalic artery
- Veins - jugular and subclavian veins
- Nerves – Spinal cord,
Brachial plexus, cranial nerves, peripheral nerves
- Gastrointestinal tract –
Pharynx, oesophagus
Blunt injuries - Assessment
Features on
history – any direct blow/trauma to the neck or
severe blow to head/face
- Eliciting the exact
nature of the injury, and the regions of the body injured can be difficult
as the injury may be unwitnessed or “hidden” within the multi-trauma
patient
- Blunt injuries to the
neck can lead to laryngeal injury and airway compromise, vascular injury
with resultant stroke, neurological injury to the brachial plexus or
spinal cord (see C-spine CPG)
|
Mechanism
|
Examples
|
|
Falls
|
- toddlers falling and
striking neck onto the edge of a low table
- older children falling
from bicycles and striking neck on the handle-bars
|
|
Quad bike or motorbike injuries
|
- ‘clothes-line’
(garrotting) type injury in either setting
|
|
MVA
|
- rapid deceleration of restrained passenger, especially
with sash of seatbelt lying across the neck
- rapid deceleration of
unrestrained passenger hitting neck onto dashboard
- other hyperextension or
hyperflexion injury
|
|
Sports injury
|
- hit in neck with
cricket ball
- elbowed in neck during
football game
- martial arts strike to
neck
|
|
Strangulation / assault
|
- Hanging, ligatures
around neck, suffocation, choking
- direct blow or kick to
neck
|
Features on
examination:
- Aero-digestive
signs/symptoms include:
- Bruising / wound to neck
- Dyspnoea / stridor
- Dysponia / hoarseness / aphonia
- Dysphagia / odynophagia
- Laryngeal tendernes
- Cervical crepitus / surgical emphysema
-
Haemoptysis
- Vascular signs / symptoms
include:
- Expanding haematoma to neck
- Bruits / thrills in carotid artery
- Seat-belt mark to neck
- Sensorimotor deficits
- Cerebellar symptoms
- Visual symptoms
- Vomiting
- Loss of consciousness
- Massive epistaxis
- Horner's syndrome / anisocoria
- Neurological signs /
symptoms
- abnormal neurological examination of limbs
A
patient with an apparently stable airway, in the first few hours, may
deteriorate quickly due to oedema. Even
minor signs should still lead to very careful observation.
Management
Investigations:
Plain chest
XR - may show
pneumomediastinum / pleural effusion / hydrothorax / subcutaneous
emphysema in the event of oesophageal perforation
Plain
X-rays of neck (soft tissue views) - May show surgical
emphysema and soft tissue swelling, but are unreliable in demonstrating
laryngeal injury.
CT
angiogram of neck - Evidence the role of CT
angiogram of the neck to screen for associated cerebrovascular injury to
carotid and/or vertebral arteries is limited in the paediatric population.
Indications for CT
angiogram of neck in blunt trauma include:
- Lateralising neurologic deficit (not explained by CT head)
- Infarct on CT head
- Cervical haematoma
- Massive epistaxis
- Anisocoria / horner's syndrome
- GCS <8 without significant CT head findings
- Cervical spine fracture
- Base of skull fracture - in particular a fracture extending through the petrous temporal bone and involving the carotid canal
- Severe facial fracture (LeForte II or III only)
- Seatbelt sign above the clavicle
NB: A plain
CT neck, i.e. without contrast, may be better able to identify laryngeal
fracture, but should not be performed in the unstable patient
Contrast
swallow
- ENT may advise a contrast
study, but this investigation should not be ordered without ENT
consultation
- Water soluble contrast, if swallowed prior to x-ray may
reveal a contrast leak
- Barium contrast can cause mediastinal and/or
pulmonary inflammation if aspirated so it is better avoided if there is an aspiration risk.
All patients with signs / symptoms of injury to the neck should be
discussed with ENT for consideration of fibreoptic laryngoscopy.
Acute
Management
Initial assessment of
patient along EMST guidelines
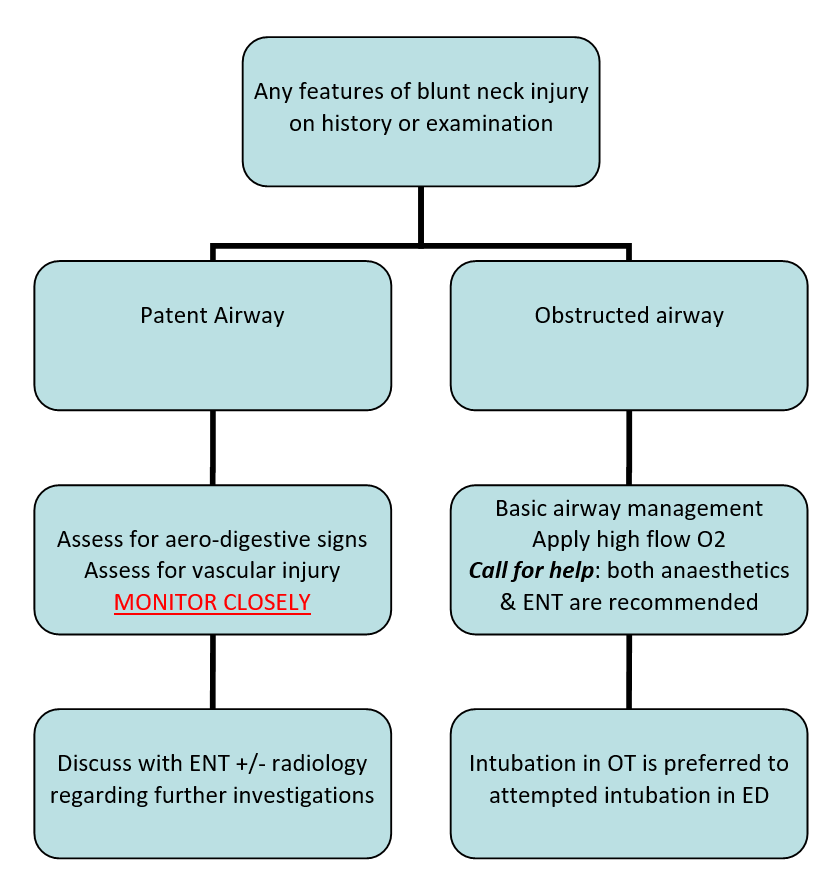
IF airway stable:
- Assess for signs/symptoms of aero-digestive injury - presence of any warrants discussion with ENT for consideration of flexible fibreoptic laryngoscopy. Dyspnoea, dysphonia and stridor are red flags.
- Assess for signs/symptoms of vascular injury - high risk mechanisms are often associated with polytrauma - if concerns discuss with radiology / vascular surgeons the utility of CT angiogram of neck.
IF unstable airway
injury:
- Apply basic airway
management techniques whilst summoning help
- Apply 100% O2 via high flow non-rebreather mask
- Perform jaw thrust to open upper airway
- Consider gentle mask ventilation (avoid aggressive positive pressure ventilation – which can worsen cervical emphysema and compromise adequate ventilation
- Any patient with an altered conscious state will require a definitive airway and ventilation HOWEVER:
- All patients with a
neck injury who require intubation should be considered to have a difficult
airway - Immediate assistance from anaesthetic and ENT specialists is strongly
recommended
- Be aware that the administration of paralytics to a patient with a laryngeal injury may lead to complete airway obstruction – if at all possible awake fibreoptic guided intubation or rigid bronchoscopy in the operating theatre is preferred to attempted intubation in ED.
- If emergent intubation is required outside of the operating theatre – for example in the peri-arrest patient with acute hypoxia then the following should be considered:
- Smaller than anticipated ETT sizes may be required - due to swelling. Attempted intubation of partially injured trachea risks worsening the injury and potentially converting a partially transected trachea into a complete transection.
- A surgical airway kit must be available an the clinician prepared to use it if orotracheal intubation fails.
- Use of a video device if available.
- Consider the possibility of an unstable cervical spine fracture in neck trauma. Be aware of neck position during emergent intubation.
Management of blunt neck injury
Penetrating
injuries
Historically penetrating injuries to the neck have been considered
along the lines of anatomical location, with all injuries in Zone II (between
cricoid and angle of the mandible) requiring surgical exploration, and those in
Zone I (clavicles to cricoid) and III (angle of mandible to base of skull)
requiring imaging.
Practical management of penetrating neck injury can be considered
along looking for hard or soft signs of injury (see below)
Penetrating Injuries - Assessment
Features
on History
- Penetrating injuries
may be low velocity (e.g. stabbing) or high velocity (e.g. gunshot, explosive
debris)
- Actively look for
injuries elsewhere – patients who have been stabbed / shot may have
multiple wounds. Patients involved
in a blast injury will commonly have multiple injuries.
Features
on examination
- Look for hard / soft signs of vascular and aerodigestive injury[1]
|
|
Hard
signs
|
Soft
signs
|
|
Vascular
|
- Active bleeding
- Large (expanding)
haematoma
- Bruit / thrill
- Reduced GCS
- Shock
|
- Minor bleeding
- Small haematoma
|
|
Aerodigestive
|
- Haemoptysis
- Haematemesis
- Air / Bubbles in
wound
|
- Dysphagia
- Dysphonia
- Subcutaneous air
|
In paediatrics it is prudent to consider stridor as an additional "hard" sign as it may indicate impeding airway loss secondary to bleeding into the airway, or from swelling encroaching on the patency of the airway.
Acute
Management:
- Patients with Hard signs
require operative management - Intubation in the operating theatre is preferred to attempted intubation in ED
- Patients with Soft signs (if
stable) require a CT angiogram
- Patients with No signs can be
observed
All wounds deep to the platysma,
should be discussed with the ENT team.
Severe vascular injury may require
consultation between the On Call Paediatric Surgeon, the Cardiac Surgery
Consultant, the Plastic Surgery Consultant, the RCH Interventional Radiologist
and/or with the On Call RMH Vascular Surgeon as per the following policy: Severe
Vascular Injury in Children
Referral
Consider consultation
with local ENT team:
All injuries
with signs of blunt or penetrating neck trauma should be discussed with ENT
Consider transfer
when:
All children
with major trauma, including blunt / penetrating neck trauma, should have
definitive management in the major trauma centre (RCH)
Children
requiring care beyond the comfort level of the hospital
For emergency advice and
paediatric or neonatal ICU transfers, call the Paediatric Infant Perinatal
Emergency Retrieval (PIPER) Service: 1300 137 650. PIPER will in turn arrange consultation with
the RCH Emergency Deartment and ENT teams, in addition to others relevant to
planned transfer.
References
- Sperry et al. (2013) Western Trauma Association Critical Decisions in Trauma: Penetrating neck trauma. J Trauma Acute Care Surg 2013;75(6):936-940