Introduction
Constipation is one of the most frequent, adverse reactions that can occur post-operatively secondary to a reduction in fluid intake, immobility and medications such as opioids. Faecal impaction may occur causing pain and discomfort for patients as well as
increasing the length of hospital stay. Conversely, the patient’s medical condition and medications such as antibiotics can also lead to diarrhoea.
Aim
The aim of this guideline is to assist nurses who work within the paediatric field around the prevention and management of constipation in the post-operative patient.
Definition of Terms
- Aperients — Oral or rectal medications which can be given to stimulate or facilitate the evacuation of the bowels.
- Constipation — An alteration in the consistency or ease of passing stool or the failure of the bowels to open for 3 consecutive days.
- Diarrhoea — Passing loose, watery or more frequent stools. A common side effect of aperient and antibiotic use.
- Fibre — Indigestible parts of plant foods (such as wholegrain cereals, fruits and vegetables) that helps to soften and add bulk to faeces; making it easier to pass through the digestive tract.
- Opioids — Analgesics that are useful agents for managing acute or chronic pain. These can be given both orally or intravenously.
- Ileus — A post-operative complication that is characterized by the loss of forward flow of intestinal contents. It is often accompanied by abdominal cramps, increasing abdominal distension, constipation or vomiting, electrolyte disturbances and
dehydration.
Assessment
All post-operative patients are at risk of developing constipation due to a variety of factors, such as changes in mobility status, reduced oral intake and as a side effect of medications. Constipation is a common adverse effect from opioid medication use due to the action upon opioid receptors in the gastrointestinal
tract. This leads to a reduction in gastrointestinal propulsion and an increase in fluid absorption.
If the patient reports difficulty passing stools, has not had a bowel action since surgery, or is currently taking opioids, then the following should be considered:
- When was the last time they opened their bowels? Were they already constipated before surgery?
- What is causing the child to be unwell? What is their reason for admission?
- Does the patient have a history of constipation? Are they on regular aperients at home?
- Are they allowed to eat and drink, or take oral/enteral medications?
- What is their mobility like? Is their mobility decreased? Are they likely to be resting in bed for a long period of time?
Physical Assessment
- Auscultate the abdomen for bowel sounds, if bowel sounds are present, or the patient reports they are passing flatus, clear fluids can commence, and aperients can be administered. Patients must not commence oral fluids if bowel sounds are not present as this finding may indicate an ileus. Decreased or absent bowel sounds may also indicate
constipation.
- Assess their oral intake by monitoring their fluid balance on the fluid balance flow sheet to identify the patient’s input and output. Considerations include oral intake, hydration status, vomiting, urine output and colour.
- Discuss the child’s oral intake at home, including their usual diet and eating patterns before surgery.
- Observe if the child’s abdomen is bloated or distended. Consider using a tape measure to compare abdominal girths over time.
- Palpation of the abdomen, to detect faecal masses in line of the colon.
- Should medical team be concerned about abdominal distension they may order an Abdominal x-ray.
Management of Constipation
Non-Pharmacological
- Encourage oral fluid intake. Water is the best choice for patients over 12 months of age. Consider fluid alternatives such as milk, soup and fresh fruit if the patient does not want to drink water.
See Appendix 2 for daily recommended oral fluid intake by age.
- Encourage mobilisation. Physiotherapy can be utilised to assist patients to mobilise. Continue to encourage patients to get out of bed and walk around. Ensure immobile patients are moved and/or transferred out of bed frequently.
- Discourage use of bedpans and urinal bottles unless it is unsafe, or impractical to get the patient out of bed to the toilet.
- Encourage a healthy, balanced diet with plenty of fibre.
- Consider if nausea (or vomiting) may be contributing to poor fluid intake. Escalate for medical review or administer a prescribed antiemetic.
- If patient is already constipated and toilet-trained, encourage child to sit on toilet or commode for short periods ~30 minutes after meals. Use a footstool to ensure knees are higher than hips when sitting on toilet/commode (where possible). Encourage child to lean forward and place
elbows on knees. This position helps to relax pelvic muscles, making it easier to pass stool (see image below). If patient is unable to leave bed, an upright position on bedpan could also be trialled to assist if tolerated.
- Try to keep toileting experience positive for younger children. Ensure analgesia is given prior to toileting for comfort and to promote relaxation of pelvic muscles.
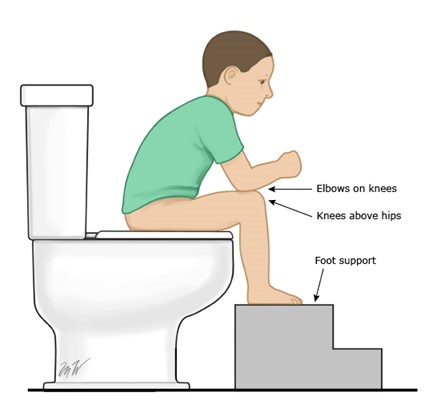
Source: UpToDate® (2021), Constipation
in infants and children: proper positioning on toilet for child,
https://www.uptodate.com/contents/images/PI/126638/ProprpstngtoiletchildPI.jpg
Pharmacological
Prior to giving aperients, the nurse should:
- Identify the age and developmental status of the child – select an age appropriate aperient. Consider if child can tolerate oral medications, or if they can be given via PEG or NGT/NJT.
- Assess for previously used effective aperients by the child. Review if child is on a regular bowel regime at home.
- Review how long the patient will need to take opioid medications. If nil or minimal doses of opioid medication are taken and patient quickly transitions to simple analgesia, aperients may not be needed. Monitor and commence aperients if no bowel action
within 2-3 days post-op.
- Patients undergoing major surgery who are anticipated to have significant analgesia requirements (opioid infusions +/- ketamine, epidural) should have aperients charted in their Medication Administration Record (MAR) as soon as possible unless contraindicated.
- Consider if it is possible to reduce the patient’s opioid intake. Consider options of adjunct analgesics (e.g. tramadol, clonidine, paracetamol, NSAIDs) charted on the patients MAR that could be administered to help reduce opioid use.
Opioid related constipation
Multiple forms of aperients are usually needed to relieve opioid induced constipation in post-operative patients (see
Appendix 1). Recent studies suggest macrogol preparations may produce more frequent stools in the paediatric population compared with other commonly used aperients. If the patient does not already have their own bowel regime in place, consider administering the following (in consultation with medical teams):
- Commence Movicol® (Macrogol 3350 + electrolytes) OR OsmoLax® (Macrogol 3350) if age appropriate and can be tolerated
AND
- Lactulose (liquid) OR Coloxyl with Senna™ (tablets) OR Coloxyl™ infant drops (0-3yrs)
- If patient is not tolerating aperients, consider mixing with patient’s preferred drink, trialling a new flavour (see
Appendix 1), or seek medical team advice for alternative options.
- If patient has been given oral aperients but BNO for more than 3 days after surgery continue to escalate treatment. Consider requesting an enema such as a Glycerol Suppository, a Microlax® or a Fleet® if appropriate.
Management of Diarrhoea
- Intravenous antibiotic use can disrupt the normal, healthy bacteria in the gut, which sometimes leads to inflammation of the colon from Clostridium
difficile (C.diff) overgrowth. Signs and symptoms include frequent, foul smelling watery stools, painful abdominal cramps, nausea, fever and appetite loss. Notify treating medical team if infective causes are suspected and initiate contact precautions.
- Discontinue, or reduce aperient use as appropriate.
- Monitor fluid balance and assess for signs of dehydration.
- Consider patients medical condition and reason for surgery – is diarrhoea expected post-operatively. Ask patient’s family or carers if other contacts are unwell.
- Take measures to preserve patient dignity, privacy and comfort.
Special Considerations
- An ileus is a more serious post-op complication that occurs most commonly after abdominal surgery. Contributing factors can include anaesthesia, post-operative opioids, previous abdominal surgery and early post-operative feeding, thus the importance of audible bowel sounds before commencing oral
diet and fluids is strongly recommended. Postoperative ileus causes delayed bowel movement or flatus with abdominal distention and possible nausea or vomiting. Escalate concerns for medical review.
- General surgical or gastrointestinal patients undergoing abdominal, or bowel surgery will have different bowel patterns in the post-operative period, thus discretion regarding the use of aperients needs to be taken by the treating team. In most cases, the treating team will not prescribe aperients
for this patient group.
- Rectal suppositories and enemas should not be used in the neutropenia/thrombocytopenia population due to the risk of bowel perforation, infection or uncontrolled rectal bleeding.
- Children with cerebral palsy and other complex histories may already have bowel management issues due to decreased gastric motility and inadequate fibre intake. Consequently, they may already have an established plan for aperient use at home. An effective bowel regime should be initiated early with the
treating team and discussed with family to assist in preventing constipation after surgery.
- Unresolved constipation can lead to severe discomfort, and may present as increased pain, irritability, or even respiratory changes (shallow breathing, desaturations +/- tachypnoea) in infants and non-verbal children. Therefore, it is important to consider if constipation is a contributing factor when
assessing pain or respiratory distress in a post-operative patient.
Education
- Provide information for parents on appropriate diets and healthy bowel actions. This can be accessed via Kids Health Info (see Companion Documents).
- Educate patients and their families on the use of aperients if required on discharge.
Companion Documents
Clinical Practice Guidelines
Kids Health Info
Appendix 1: Aperients
| Class |
Medication Names |
Onset of Action |
Side Effects |
Practice Points |
| Iso-osmotic laxative |
Movicol®
Movicol® Junior |
1-4 days |
Nausea and vomiting
Abdominal cramps
Distention |
Dissolve sachet in 125ml of water or cordial (has salty taste)
Available in several flavours |
| Iso-osmotic laxative |
OsmoLax® |
1-3 days |
Abdominal cramps
Diarrhoea |
Mix with 120-250ml of hot or cold liquid depending on dose
(no salty taste) |
| Osmotic laxative |
Lactulose |
1-3 days |
Abdominal discomfort
Flatulence |
Mix with water or juice to improve taste |
| Stool Softener |
Coloxyl™ Infant Drops |
2-3 days |
Loose stools
Abdominal discomfort Dehydration |
Can mix in formula, water or juice
For children 0-3yrs |
| Stimulant laxative |
Senokot®
Coloxyl with Senna™ |
6-12 hours |
Abdominal cramps |
Can be swallowed on its own (tablet) or mixed with water, milk or food |
| Enema |
Microlax®
Fleet®
Glycerol Suppository* |
Within 30 minutes |
Renal patients = dehydration |
Do not use in Oncology patients |
* Can be nurse initiated (at RCH). Must be documented in MAR and immediately communicated to treating medical team.
Appendix 2: Recommended daily oral
fluid intake (by age)
| Age |
Recommended oral fluid
intake |
| Infants 0-3 months* |
150ml/kg/day |
| Infants 3-6 months* |
120ml/kg/day |
| Infants 7-12 months# |
100ml/kg/day |
| Girls and boys 1-3 years |
1000ml (~4 cups) |
| Girls and boys 4-8 years |
1200ml (~5 cups) |
| Girls 9-13 years |
1400ml (5-6 cups) |
| Boys 9-13 years |
1600ml (~6 cups) |
| Girls 14-18 years |
1600ml (6-7 cups) |
| Boys 14-18 years |
1900ml (7-8 cups) |
* from breastmilk or formula
# from breastmilk, formula, plain water and other beverages
Links
Better Health Channel
UpToDate
Evidence table
Click here to view the evidence table.
Please remember to read the
disclaimer.
The development of this nursing guideline was coordinated by Tineke Fitzgerald, CNS, Platypus Ward, and approved by the Nursing Clinical Effectiveness Committee. Updated May 2023.