Introduction
The paediatric nutrition screening tool (PNST) should be completed as part of Nursing admission and every 7 days for all inpatients and is a requirement for compliance to NSQHS Standards, Comprehensive Care. The screening tool is used to identify those patients that require nutritional
assessment and interventions. Information can be obtained from parents/carers, medical records and by examining the child.
Aim
The aim is to identify inpatients at nutritional risk.
Definition of Terms
Screening: process of identifying patients who are at; or already have a disease or injury. Screening requires enough knowledge to make a clinical decision
Risk Assessment:
assessment, analysis and management of risks. It recognises which events may
lead to harm in the future and minimises their consequences
Poor nutrition: is the decrease in the intake of food, considered in relation to the body’s dietary needs
Assessment
The PNST is intended to be used on hospital admission of all inpatients. The screening tool consists of 4 “yes/no” which is embedded in the nursing workflow practices within the Electronic Medical Record (EMR) under Admission, Discharge, Transfer (ADT) Navigators within the Admission assessment.
1. Has the child lost weight lately?
- Children should gain weight as they grow and only lose weight if clinically indicated. This question identifies if the child has lost weight and requires further investigation. If there is no weight history, a subjective assessment can be made as to whether the parent/carer/health professions is of the opinion that the child looks like they have lost weight. ‘Lately’ can be over a period of days or six months.
2. Has the child had poor weight gain over the last few months?
- The rate of weight gain of children depends on their age. Refer to growth standards to determine if weight gain is appropriate
3. Has the child been eating/feeding less in the last few weeks
- Assess whether the child has reduced nutritional intake compared to their usual intake. Nutritional intake can be provided via various routes including oral, tube or parenteral. Gastrointestinal symptoms such as vomiting and loose stools can affect oral intake and should be considered.
4. Is the child obviously underweight?
- Examine the child for physical indicators of malnutrition such as loss of fat stores and muscle wasting. Protruding or prominent bones of clavicle and scapular, depression along the inner thigh and small calf are evidence of muscle wasting.
Management
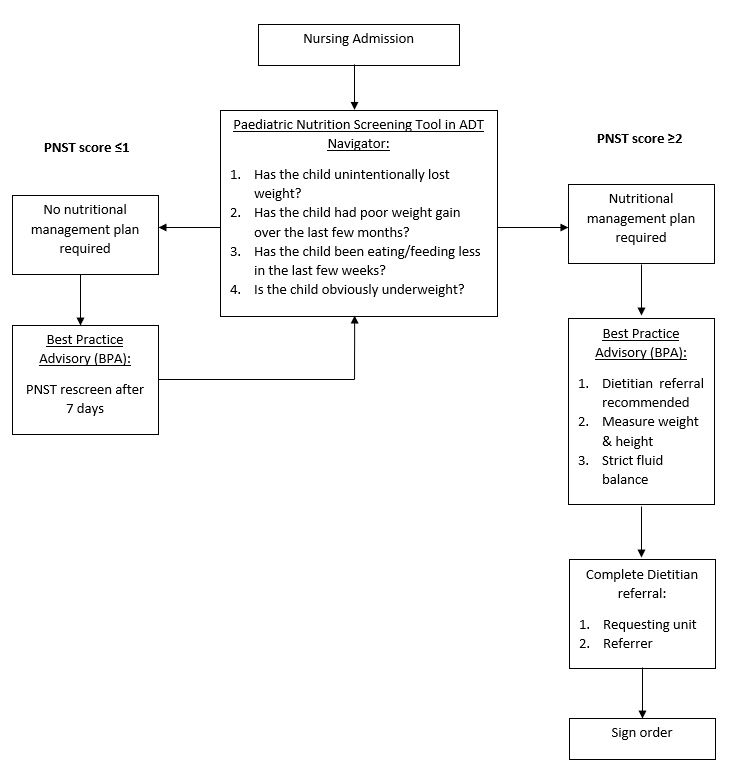
Figure 1. Management flowchart
If the child does not require a nutrition management plan it is important that they are rescreened every 7 days throughout their stay. Regular measurements of weight and monitoring of nutritional intake should be completed.
Companion Documents
Links
Evidence Table
See
attached evidence table for this guideline.
Please remember to
read the disclaimer.
The revision of this nursing guideline was coordinated by Kristyn Ford and Natalie Whitehead, Dieticians and approved by the Nursing Clinical Effectiveness Committee. Updated February 2023.