Focal seizures arise from a particular part of the brain. This part of the brain which causes seizures is called the epileptic region or focus. During a seizure, brain cells in this epileptic region become overactive and there is a localised increase in electrical activity and blood flow in that part of the brain.
Video EEG monitoring helps to localise the epileptic region by recording the brain's electrical activity during a seizure. SPECT can help further localise the epileptic region by showing the abnormal blood flow associated with a seizure.
What is SPECT?
SPECT is a nuclear medicine test and stands for Single Photon Emission Computed Tomography.
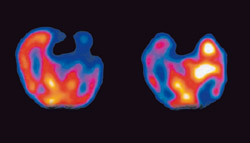
SPECT scans show brain function (what the brain is doing), as opposed to CT and MRI scans which show brain structure (what the brain looks like).
SPECT involves an intravenous injection of two substances, technetium and a blood flow agent. The injection is given during or immediately following a seizure (ictal SPECT). Technetium is a very low energy, radioactive substance that is used in nearly all nuclear medicine scans in infants, children and adults. Ceretec® and Neurolite® are the names of the blood flow agents which bind to technetium and when injected, distribute throughout the brain in proportion to blood flow.
Brain scanning in the Nuclear Medicine Department later reveals images of blood flow at the time of injection.
Is the radiation dangerous?
The total body radiation dose from technetium injection is very small, being less than that which the chest or brain receives with an x-ray or CT scan. However, pregnant women should not nurse or have prolonged close contact with your child for 24 hours following the injection. There are no reported side effects from injection of Ceretec® or Neurolite®. Teenage girls who may be pregnant should not have a SPECT scan.
How and when will SPECT be performed?
SPECT usually takes place in conjunction with
video EEG monitoring in the Epilepsy Monitoring Unit on
Cockatoo ward.
The procedure requires your child to have an intravenous line in the back of the hand or forearm. To minimise discomfort, some local anaesthetic cream can be placed on the skin prior to the intravenous line being inserted. The local anaesthetic cream will remain on the skin for a minimum of 45 minutes. This will numb the skin prior to the small plastic catheter being inserted into a vein. The discomfort of this should be less than that of a blood test.
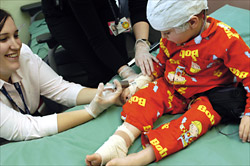
When a typical seizure occurs, the parent or carer alerts the nursing staff by pressing the emergency button and they will make their way quickly to the room, rapidly mix the technetium and blood flow agent (if necessary) and then inject the appropriate dose.
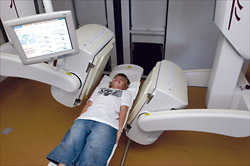
A brain scan is then performed in the Nuclear Medicine Department, within a few hours of the injection. Some children require sedation or a general anaesthetic for the brain scan, as it takes approximately 45 minutes to obtain the pictures and children must lie perfectly still. Some children are given an injection of an anticonvulsant medication to prevent seizures during scanning.
Please note: Not all children having
video EEG monitoring need SPECT scanning. SPECT can only be performed on weekdays between 9.30am and 3.30pm. Medical emergencies, equipment problems and staffing issues can arise from time to time, such that SPECT may not always be possible. The inability to obtain a SPECT scan will not necessarily compromise your child's assessment.
Will more than one SPECT scan be needed?
Only one ictal SPECT scan is usually performed. However, some children require a repeat SPECT scan during another seizure, usually when the child has several types of seizures or the injection was well after the seizure finished. In some children a SPECT scan is done when they are not having a seizure (interictal SPECT). This scan is used as a baseline for comparison and may be arranged as an outpatient. SPECT scans are not repeated within 24 hours.
For more information about SPECT
Contact an Epilepsy Nurse Specialist in the
Neurology Department or a Nuclear Medicine scientist in the
Medical Imaging Department