General Comments
This information is provided as general information about the drug treatment of epilepsy. The information is not a substitute for proper medical advice. Consult your doctor for any questions or concerns you have about you or your child's medication. For urgent information about incorrect dosing or overdosage please contact your doctor, pharmacist or the
Poisons Information Centre 13 11 26 Nationwide Australia.
Antieplieptic medications do not cure epilepsy, but rather attempt to prevent seizures. Strictly speaking, these medications are antiseizure or anticonvulsant, rather than antiepileptic. Antiepileptic medications do not alter the underlying problem predisposing to seizures. People with epilepsy are prescribed antiepileptic medications with the aim of decreasing the number, severity, and/or duration of seizures. While seizure freedom is the ideal outcome of treatment, seizures can still occur while taking antiepileptic medication.
Antiepileptic medication is usually prescribed for children with recurrent seizures, ideally after a specific epilepsy syndrome diagnosis is made and the risk of subsequent seizures is known. However, there are instances when a doctor may prescribe medication after a single seizure (eg. when the risk of subsequent seizures is great) and when medication is not prescribed after several seizures (eg. when seizures are a minor and self-limiting problem). Other factors taken into consideration when prescribing antiepileptic medication include the child's age, other medical conditions, findings on an EEG, other medications the child is taking, and potential for side effects.
How antiepileptic medications work?
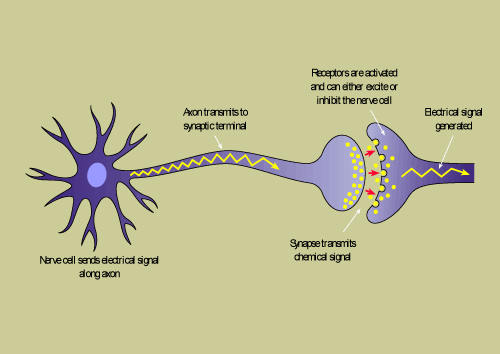
Normal brain function involves "communication" between millions of nerve cells (neurons). At any one time, there are nerve cells which are resting, exciting or inhibiting other nerve cells. A nerve cell is made up of a cell body and branches called axons and dendrites which join other neurons at junctions called synapses. Electrical signals are sent from the cell body along the axon to the synapse, these electrical signals being the result of ion (sodium, potassium, calcium) currents across channels in the nerve cell membrane. Chemical signals (neurotransmitters) pass across synapses between neurons. Neurotransmitters cross the synaptic gap between neurons and fix to receptor points of the adjoining neuron. Some neurotransmitters function to excite the joining neuron (eg. glutamate) to send a further electrical signal. Other neurotransmitters function to inhibit the joining neuron (eg. GABA) and inhibit electrical signals passing down that neuron. It is by these electrical and chemical pathways that the millions of neurons within the brain communicate and function normally.
Seizures occur when there is an imbalance within these excitatory and inhibitory circuits in the brain, either throughout the brain (generalised epilepsy) or in a localised part of the brain (focal epilepsy), such that neurons "fire off" in an abnormal fashion.
Antiepileptic medications work in different ways to prevent seizures, either by decreasing excitation or enhancing inhibition. Specifically, they act by either:
- Altering electrical activity in neurons by affecting ion (sodium, potassium, calcium, chloride) channels in the cell membrane.
- Altering chemical transmission between neurons by affecting neurotransmitters (GABA, glutamate) in the synapes.
- For some drugs, the mode of action is unknown.
As the specific mechanisms that cause epilepsy are mostly unknown, drugs with specific mechanisms of action directed at the underlying "epileptic processes" have not yet been developed.
How do antiepileptic medications reach nerve cells?
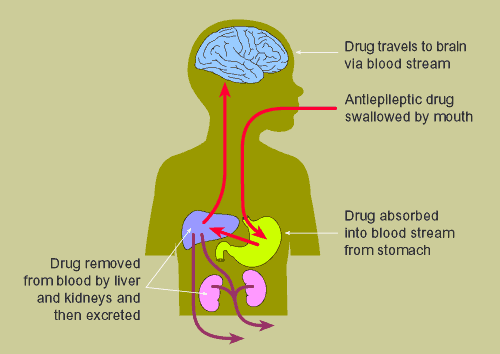
An antiepileptic medication is swallowed by mouth and passes directly to the stomach. Once in the stomach the medication is absorbed into the blood stream where it is then circulated to the brain, via the liver, and acts on the nerve cells. As the drug is circulating in the blood, it is gradually removed by either the liver breaking it down (metabolism) or the kidneys filtering it out (excretion). Some drug metabolites are active and produce either beneficial antiepileptic effects or adverse side effects. Most commonly prescribed antiepileptic medications are removed from the blood at a rate that allows twice daily dosing to maintain adequate blood levels. Some drugs are removed more quickly than others and have to be taken 3 or 4 times throughout the day, whilst others are removed slowly and can be taken once each day.
For some medications, children need to have blood tests to determine the level in the bloodstream (eg. phenytoin, phenobarbitone, carbamazepine). These blood levels are generally measured before a dose is due. Not all antiepileptic medications need to be monitored with drug levels, as there is not a good correlation between drug level and effect.
The dose of medication prescribed is determined by the child's age and weight. Young children and adolescents have greater rates of drug clearance and are often prescribed doses per kilogram of body weight greater than an adult would receive.
In an emergency situation, such as status epilepticus, some antiepileptic drugs can be given directly into the blood stream, into the rectum, nose or buccal to act very quickly to control seizures.
Which medication and how is it prescribed?
The choice of medication and how each is prescribed is a specialist area of paediatrics and child neurology. Prescription of antiepileptic medication is only done by a doctor with knowledge of antiepileptic medication and epilepsy in children. General principles that doctors follow when prescribing antiepileptic medications in children include:
- starting with a low dose and slowly increasing to reach a maintenance dose (this helps to reduce or avoid side effects during the introduction phase and is important for some drugs where there is risk of allergic rash)
- aiming for control of seizures with one antiepileptic medication (monotherapy) where possible
- giving a medication a good trial period to work before changing
- recognising that doses and tolerance of antiepileptic medications vary between individuals
- spacing medication doses appropriately to maintain stable blood levels
- avoiding combinations of antiepileptic medications that are known to not interact well
- slowly withdrawing antiepileptic medications if ceasing treatment, especially the barbituate and benzodiazepine medications
Always follow your doctors instructions about medication.
A-Z of antiepileptic medication
* MIMS links only available from within RCH
Common antiepileptic medication choices for seizures in children
| Seizure Type |
Commonly Prescribed Antiepileptic Medications |
| focal seizures |
carbamazepine, clobazam, lamotrigine, levetiracetam, oxcarbazepine, phenytoin, sodium valproate, topiramate, lacosamide, zonisamide |
| generalised tonic clonic seizures |
carbamazepine, clobazam, lamotrigine, levetiracetam, oxcarbazepine, phenytoin, sodium valproate, topiramate, lacosamide, zonisamide |
| absence seizures |
ethosuximide, lamotrigine, sodium valproate |
| myoclonic, tonic and atonic seizures |
clobazam, clonazepam, lamotrigine, levetiracetam, sodium valproate, topiramate |
| infantile spasms |
prednisolone, vigabatrin, ACTH, nitrazepam |
| neonatal seizures |
phenobarbitone, phenytoin, clonazepam, levetiracetam, topiramate |
Side effects
All medications have the possibility of causing side effects. There are three main types of antiepileptic medication side effects.
- Some mild side effects are common when starting antiepileptic medications, particularly if the dose is increased rapidly. These include nausea, abdominal pain, dizziness, sleepiness, irritability, anxiety or mood changes. These are usually not serious, but may worry some people and should be discussed with your doctor or pharmacist. Your doctor may slow the rate at which the medication is being introduced or may cut back another antiepileptic medication with which it may be interacting.
- Some side effects are common to antiepileptic medications when prescribed at too great a dose and are similar to being "drunk" eg. unsteadiness, poor concentration, sleepiness, double vision, vomiting, tremor. It is important to report these side effects to your doctor immediately if they occur.
- Some side effects are peculiar to individual medications and only occur in some people eg. rash, blood problems, liver problems, severe behaviour disturbance, worsening of seizure control. There are some patients or situations in which there may be increased risk of such side effects with a certain medication.
Please refer to the specific drug information provided with your medication for a more detailed list of side effects. As numerous side effects are listed against all medications, your doctor should help you understand which are the more common or potentially serious side effects to look out for. It is important to contact your doctor if you are worried about these or other side effects. For urgent information please contact your doctor, pharmacist or the
Poisons Information Centre 13 11 26 Nationwide Australia.
General considerations
Commencing medication
Always read the consumer information and follow instructions from your doctor and pharmacist carefully. Any concerns or questions should be discussed with your doctor or pharmacist. It is important to take the exact dose that is prescribed by the doctor at approximately the same time each day. It may take many days or weeks to reach the dose that is most effective. The dose that your doctor is building up to may not be the maximum tolerated or prescribed dose for that medication.
Missing a dose
Establishing a regular routine can help to avoid medication being missed. Taking medication with meals or using a medication dosette may help. Maintaining supplies and current prescriptions can avoid running out of medication at the last minute. If a dose is missed it can generally be taken as soon as you remember. Do not double up on doses. It is advisable not to take the missed dose if it is close to the next one. Keep a record of doses that have been missed.
Other medications
Only take medication that is prescribed by your doctor. Never try another person's medication. What medication may control one person's seizures may not be suitable for another. Many drugs interact with each other, so it is very important to always seek the advice of a doctor or pharmacist before taking any other medications with antiepileptic medications. It should also be noted that many "complementary medicines" interact with antiepileptic medications.
Illness
Vomiting and diarrhoea can affect the amounts of medication that are absorbed from the gut into the blood stream. This can result in low circulating levels of antiepileptic medication. Also, viral illnesses are a common trigger for seizures in children with epilepsy. If vomiting occurs within minutes of taking the medication, another dose can be administered. Seek medical advice if vomiting and diarrhoea persist.
Monitoring effectiveness
It is recommended to keep a
seizure diary to record seizures as this helps monitor effectiveness of medication. The diary can also be used to record missed medication, side effects, illnesses and doctors visits.
Some medications require regular blood level monitoring by a simple blood test. These medications include phenytoin, phenobarbitone and sometimes carbamazepine; your doctor will determine if these are necessary.
Teaching children how to swallow tablets and capsules
Teaching children how to swallow tablets and capsules
Contraception and pregnancy
Concurrent use of antiepileptic medication with hormonal contraceptives (the pill) may cause the contraceptive to be ineffective. Higher dose oral contraceptives and additional non-hormonal (barrier methods) are often recommended but you should seek specific advice from your family doctor, neurologist, gynaecologist or Family Planning Centre.
Many complex circumstances exist during pregnancy for women with epilepsy. It is recommended that women taking antiepileptic medication receive pre-pregnancy counselling and discuss their individual circumstances with their doctor.
The Australian Centre of Clinical Neuropharmacology has developed a voluntary
Australian Epilepsy Pregnancy Register of women who become pregnant whilst taking antiepileptic medication. The primary aim of the register is to determine the incidence of adverse foetal outcomes resulting from pregnancies in Australian women who were taking antiepileptic medications. The secondary aims are to identify if certain antiepileptic medications, or combinations of medications, are associated with a higher overall incidence of foetal outcomes or specific types of malformations. As well we will try to identify other risk factors that may increase the risk of malformations occurring.
Precautions
Effects on ability to drive and use machines
Some antiepileptic medications can cause drowsiness, sleepiness, incoordination and slowed reaction time, especially when the medication is being introduced or the dose is being increased. Effects on individuals should be assessed prior to driving or using machinery.
Effects when taken with alcohol
If alcohol is taken in combination with antiepileptic medication, extra sedative effects can occur. Also, alcohol increases the likelihood of seizures.
Antiepileptic medications permitted in sport
For an up-to-date listing of medications permitted in sport, refer to the
Australian Sports Anti-Doping Authority.
References